Our purpose is to review the embolization technique as well as the MR images in a series of 21 cases.
Symptomatic uterine fibroids are the main indication for uterine embolization.
The most common clinical syndromes are hypermenorrhea,
dyspareunia or abdominal pain.
Before the procedure a complete gynecological and imaging evaluation is necessary to rule out contraindications.
Adnexal,
endometrial and uterine pathology need to be excluded before the procedure as well as the location of fibroids.
Literature recommends avoiding this technique in pedunculated fibroids.
Uterine embolization technique in our hospital steps are: epidural anesthesia,
sedation and prophylactic antibiotic treatment of the patient followed by the puncture of the common femoral artery.
The uterine arteries are catheterized and embolized using spherical particles.
Finally,
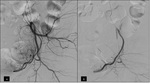
a control arteriography is performed to demonstrate correct embolization (Fig. 1 and Fig. 2).
Absolute bed rest for 24-48 hours,
adequate blood pressure control and pain control are recommended after the procedure.
Morphine is administrated through an epidural catheter for 24 hours.
The complications can be divided in immediate,
acute (first 30 days) or long-term (after 30 days).
Immediate complications include allergic reactions to contrast,
iatrogenic vascular lesions,
thrombosis and infections like septicemia.
Acute complications are recurrent pain,
haemorragia,
genital infection or vaginal expulsion of the fibroid.
The most common long-term complication is post-embolization amenorrhea.
Post-embolization syndrome had been described and characterized by abdominal pain,
nausea,
vomiting,
low-grade fever and leukocytosis.
It appears 24-48 hours after the procedure and usually ends within 48 hours.
The differential diagnosis with sepsis must be done.
Six months after procedure MRI is performed to assess post-embolization changes.
Before embolization,
MRI study of the vascularity of fibroids allows to assess if embolization is the indicated treatment for the patient.
More vascularized fibroids are more likely to respond to treatment,
while fibroids with cystic-necrotic areas with low vascularity will show a lower response to treatment.
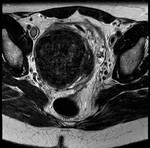
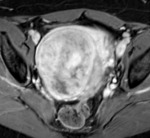
Non-degenerated fibroids have a typical MRI presentation: well-delimited masses with low signal compared to the myometrium in T2-weighted sequences and intense contrast enhancement (Fig. 3 and Fig. 4).
Cellular fibroids have hypersignal in T2 and enhance after gadolinium administration in T1 sequences.
Degenerated fibroids have variable appearance in T1,
T2 and after gadolinium administration.
After embolization,
uterine fibroids MRI findings are: hypersignal in T1 due to hemorrhagic necrosis,
with a variable T2 signal.
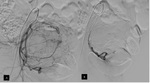
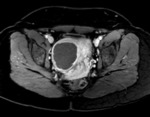
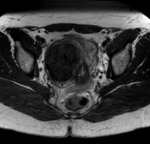
No contrast enhacement is seen if fibroid is necrosed (Fig. 5 and Fig. 6).
Absence of contrast enhancement of the fibroid after embolization is indicative of good prognosis.
Patients that show residual contrast enhancement will probably require re-embolization or other treatments.
Another common finding in MRI after UE include the reduction of uterine fibroid and uterus size.
We have done a retrospective review of a series of 21 patients with uterine fibroids treated by arterial embolization technique during 6 years (2010-2016).
In our series of 21 patients,
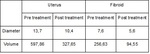
the average maximum diameter of the uterus and fibroids decreased from 13,7cm and 7,6cm to 10,4cm and 5,6cm respectively.
Also the average volume of the uterus and fibroids decreased from 597,86cm3 and 256,63cm3 to 327,65cm3 and 94,55cm3 respectively calculated with the formulas: 4/3 • π • L / 2 • W / 2 • AP / 2 for the uterus and 4/3 • π • r3 for fibroids due to their approximate spherical shape (Table 1).
In patients with several fibroids,
the largest fibroid was measured.
16 of 21 patients did not present contrast enhancement in MRI after uterine embolization.
3 patients had minimal contrast enhancement,
however they had a correct clinical evolution and did not require re-embolization or other treatments.
2 patients had persistence of contrast enhancement and clinical symptoms didn't improve,
so a hysterectomy was performed in both of them.
19 of 21 patients did not required other treatments,
with effectivity of 90% in our series.