|
TECHNICAL/EXTERNAL FACTORS
|
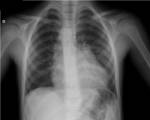
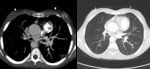
When looking for excluding an hypertranslucent hemithorax due to faulty radiologic technique one must look to the relative exposure of soft tissues in the affected side,
especially of the lateral ribs or around the shoulder girdles.
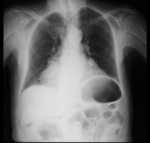
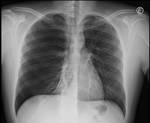
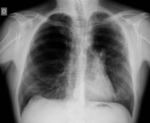
Chest radiography- Fig. 3
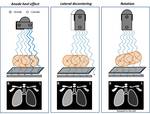
Anode heel effect refers to the intensity of the x-ray beam,
produced from the X-ray tube,
which is not uniform in all portions of the beam,
being comprised of central rays and diverging beams.
The rays towards the cathode end of the tube have more intensity,
as the rays which are parallel or near parallel to the anode get absorbed by the anode itself.
On chest radiography it can be bypassed,
by placing the thicker part of the body on the cathode side,
e.g.
upper thoracic on the anode side and lower thoracic or upper abdomen should be placed on the cathode side.
Schematic- Fig. 2
Erroneous positioning of the x-ray tube lateral to the patient's midline may also cause asymmetric exposure,
since the x-ray beam is more intense to the perpendicular side.
Schematic- Fig. 2
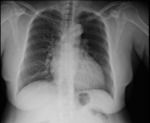
A unilateral hyperlucent hemithorax may be caused by the positioning of the patient,
as rotation away from the radiation beam alters the attenuation of the beam differently on either side of the thorax,
with decreased attenuation on the side towards which the patient is rotated.
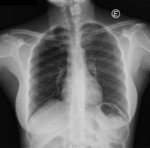
Improper patient rotation is the most frequent cause of unilateral hyperlucency,
seen in around 1% of chest radiographs.
To access if the exam is well-aligned,
one shroud evaluate the spinous processes of the thoracic vertebrae which should lie equidistant from the medial ends of the clavicles.
Rotation of the patient will lead to off-setting of the spinous processes so they lie nearer one clavicle than the other.
Besides changes in lung density,
rotation also limits accurate assessment of the cardiac size.
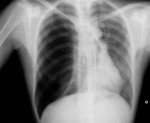
Schematic- Fig. 2
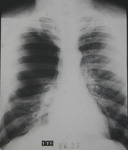
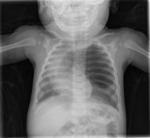
Chest radiography- Fig. 4
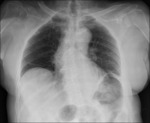
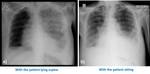
An abnormal curvature of the thoracic spine may also be the cause,
by the same radiographic principles mentioned previously,
as it may lead to an inherent anatomical rotation by uneven compression of the chest wall against the cassette,
besides deviation of the soft tissues.
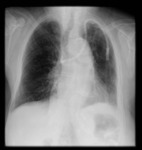
Chest radiography- Fig. 5
|
ASYMMETRIC ABSENCE OF CHEST SOFT TISSUES
|
Congenital,
adquired or post-surgical anatomic variations of the chest wall may also result in the asymmetric appearance of hyperlucent lungs.
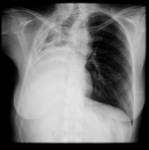
Radical mastectomy is the most common source of this problem,
where relative radiolucency is seen on the side of the breast removal,
and it’s easily inferred by the absence of the ipisilateral mammary shadow.
Surgical clips in the ipsilateral axilla may also be seen.
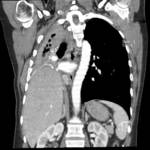
Chest radiography- Fig. 6
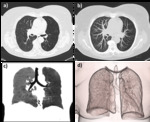
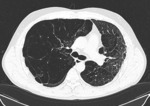
CT scan- Fig. 7
- Absence of pectoral musculature:
A similar appearance is also noted when there is an absence of pectoral musculature,
either congenital,
recognized as Poland syndrome,
or acquired,
following surgical removal for flap surgery.
Poland syndrome is a rare condition characterized by underdevelopment or aplasia of the pectoralis muscles on one side of the body,
usually associated with ipsilateral ribs/breast aplasia and upper limb abnormalities,
such as syndactyly.
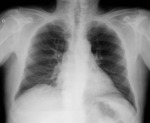
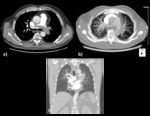
Chest radiography- Fig. 8
CT scan- Fig. 9
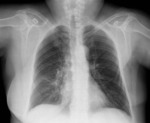
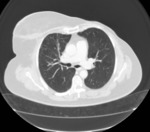
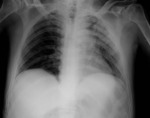
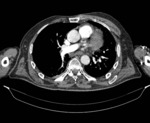
The presence of air in the pleural cavity also results in hyperlucency of the ipsilateral hemithorax.
Air can enter the intrapleural space through a communication from the chest wall (ie.
trauma) or through the lung parenchyma across the visceral pleura (such as the case of spontaneous pneumothorax from blebs rupture).
It can be recognized by observing displacement of the visceral pleural line,
absence of lung markings distal to the displaced pleural line,
and when significant,
causing contralateral shift of the mediastinum and compromised hemodynamic stability,
a life threatening condition entitled Tension pneumothorax.
Chest radiography- Fig. 10 ,
Fig. 11
- Pleural effusion/ thickening (contralateral):
In other cases of hyperlucent hemithorax,
the lucent side is normal and it’s the opposite side that is abnormally radiopaque,
which occur frequently when pleural fluid its layering posteriorly on a supine radiograph or when diffuse pleural thickening is present.
Chest radiography - Fig. 12
|
AIRWAY/PULMONARY PARENCHYMA ABNORMALITY
(ALTERED VENTILATION)
|
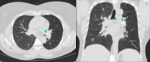
- Air trapping phenomena due to compression or bronchial obstruction:
Bronchial compression (by an hilar mass,
cardiomegaly) or endobronchial obstruction (by an foreign body,
tumour,
mucous plug) lead also to an unilateral hypertranslucent hemithorax due to air trapping, a.k.a.
the retention of excess “air” in all or part of the lung,
especially during expiration,
as a result of complete or partial airway obstruction,
and also due to accessory pulmonary vasoconstriction and consolidation.
Clinically the patient may present with cough,
respiratory difficulty,
wheezing,
hemoptysis,
or recurrent pneumonia.
In children,
especially in those between 6 months and 3 years of age,
foreign body aspiration is the most common cause and can be life-threatening.
It is typically caused by inhalation of food materials or toys.
Generally most aspirated foreign bodies are located within the right main-stem bronchus,
because of its larger diameter and more vertical course.
The radiographic appearance of foreign body aspiration depends on size,
location,
duration and nature of the aspirated material.
It’s important to note that most aspirated foreign bodies are nonradiopaque and thus the diagnosis must be inferred from indirect radiographic signs,
such as hyperinflation and air-trapping on expiratory chest radiographs. Decubitus films lying on the affected side will show little or no change in lung volume.
Even though in about one third of the cases there may be a normal chest radiograph. In this cases CT may directly identify a foreign body lodged in the tracheobronchial tree as well as well sd other associated changes such as hyperinflation,
atelectasis,
and consolidation.
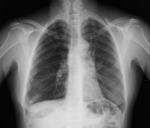
Chest radiography- Fig. 13
CT scan- Fig. 14
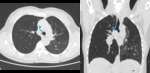
In adults,
the most frequent cause of bronchial obstruction is an endobronchial tumor.
These generally presents with atelectasis distal to bronchial obstruction,
but a small percentage of cases may present as localized hyperexpansion with radiographical hyperlucency.
Furthermore,
attenuated vascular structures,
resulting from pulmonary artery involvement by the tumor,
may contribute to the unilateral hyperlucency.
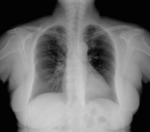
Chest radiography- Fig. 15
CT scan- Fig. 16
- Swyer-James (MacLeod) syndrome:
This relatively uncommon entity,
secondary to postinfectious obliterative bronchiolitis in infancy or childhood,
typically manifests with a unilateral hyperlucent lung as characteristic finding.
The injury to the immature lung typically follows a viral respiratory infection,
such as adenovirus or Mycoplasma pneumoniae,
and results in hypoplasia of the pulmonary artery and its branches,
and variable degree of lung parenchyma destruction,
with bronchiectasis formation.
Some patients,
however,
have little or no sequelae bronchiectasis and may miss their diagnosis until adulthood when abnormal pulmonary asymmetry is seen on an incidental chest radiograph.
It is generally characterized on radiographs by a unilateral small lung with hyperlucency,
but may also show preserved volume,
due to collateral ventilation and air trapping.
On CT the affected lung shows as being hyperlucent with diminished vascularity,
with the majority of the affected lobes being smaller,
and bronchiectasis may be present.
Chest radiography- Fig. 17
CT scan- Fig. 18
- Pulmonary emphysema (asymmetric):
Pulmonary emphysema refers to "abnormal permanent enlargement of the airspaces distal to the terminal bronchioles accompanied by destruction of the alveolar wall,
without obvious fibrosis" and is one of the entities grouped together as chronic obstructive pulmonary disease.
It comprises different morphologic subtypes,
notably centrilobular and panlobular emphysema which can be accompanied by bullous lesions,
and results in increased and usually irregular radiolucency of the lungs.
Plain radiography does not image emphysema directly,
except in the case of very advanced disease with bullae formation,
but rather indirect infers the diagnosis due to associated signs of hyperinflation,
such as flattened hemidiaphragms with widened costophrenic angles,
increased retrosternal space,
horizontal ribs; or vascular changes,
such as paucity of blood vessels and signs of associated pulmonary arterial hypertension.
CT is currently the modality of choice for detecting emphysema,
being sensitive for detection of early emphysema by demonstrating vascular attenuation,
areas of hyperlucency and small bullae,
and is able to discriminate between the different morphologic subtypes.
Chest radiography- Fig. 19
CT scan - Fig. 20
Bullous emphysema also occurs in an isolated form and a giant bullae may be the cause of unilateral increased radioluncency.
Chest radiography- Fig. 21
- Congenital lobar overinflation:
Previously known as “Congenital lobar emphysema” represents progressive hyperexpansion of one or more lobes of a neonate’s lung,
based on a congenital bronchial stenosis producing a check-valve mechanism.
Most infants develop symptoms of respiratory distress in the neonatal period,
from a few days after birth up to six months, with an increased male prevalence of about 3:1.
Most cases are idiopathic,
but several factors have been associated with its development,
with the majority of cases believed to be caused by deficient bronchial cartilage (bronchomalacia),
but can also result from endobronchial lesions,
extrinsic bronchial compression (e.g.
an anomalous vascular structure or mass) and congenital cytomegaloviral infection.
In 40-45% of cases,
the left upper lobe is involved,
even though in general the right hemithorax is the most common side to be affected,
normally the upper and middle lobes.
On imaging,
it classically presents on chest radiographs as a hyperlucent lung segment with overinflation,
resulting in contralateral mediastinal shift and ipsilateral hemidiaphragmatic depression.
In the immediate postpartum period the lobe appear opaque due to retention of fluid but later,
the fluid is replaced with air and the affected hemithorax becomes hyperlucent with a paucity of vessels.
CT is usually performed to confirm the diagnosis,
to rule out other abnormalities and to evaluate the mediastinal vascular structures or the bronchial anatomy before surgery. Furthermore,
by demonstrating hypoattenuated bronchovascular markings permit exclusion of a pneumothorax.
Operative surgery with lobectomy is the commonest mode of treatment.
Chest radiography- Fig. 22
CT scan- Fig. 23
- Compensatory hyperinflation:
Compensatory hyperinflation can occur as a consequence to conditions leading to extensive unilateral pulmonary destruction/volume loss,
in an attempt by the remaining normal lung to partially fill the space lost by the affected lung.
This mechanism usually develops with chronic volume loss and is not seen in acute collapse.
It is seen as increased lucency with attenuation of pulmonary vascular markings.
The degree of hyperinflation can often be massive in which the hyperinflated lung herniates anteriorly across the midline and may nearly totally occupy the contralateral hemithorax.
A characteristic although seldom seen radiographic finding is the “shifting granuloma,” in which a preexisting granuloma in the aerated lung changes position as it moves toward the collapsed lobe.
Chest radiography- Fig. 24
CT scan- Fig. 25Fig. 25
Other causes result from surgical intervention,
such as:
- Pneumonectomy: most commonly performed for a primary lung malignancy,
in which the lucent side is normal and it’s the opposite side that is abnormally radiopaque,
associated with volume loss with deviation of the trachea towards the side of the abnormality.
Chest radiography- Fig. 26
CT scan- Fig. 27
- Unilateral lung transplant: an increasingly common treatment for end-stage lung disease,
in which the hyperlucent side may be the native lung,
such as in cases of emphysema and pulmonary hypertension or alternatively the transplant lung,
as in cases of interstitial lung diseases such as end-stage lung fibrosis,
by which evaluation of mediastinal shift,
respectively,
towards or away the transplant lung,
is an important additional radiographic finding that should be considered.
|
PULMONARY VASCULARITY ABNORMALITY
(ALTERED PERFUSION)
|
Caused by embolic occlusion of the pulmonary arterial system,
the majority of cases resulting from dislodgement of a thrombus.
The chest radiograph is often the first imaging study obtained,
but it is neither sensitive nor specific for the diagnosis,
being best used to assess for differential diagnostic possibilities.
Almost half of thromboemboli do not produce any plain film findings,
but a large unilateral embolus can result in a unilateral hyperlucent lung or smaller pulmonary emboli may result in more localized areas of hyperlucency in the peripheral lung,
secondary to a decreased vascularity.
These oligemic lung fields can result from either arterial obstruction or distal vasoconstriction in hypoxic lung,
and constitute the Westermark's sign,
in honor to 20th century Swedish radiologist who first described this sign.
This sign present in about 10% of cases has a low sensitivity (14%),
but high specificity (92%) for the diagnosis of pulmonary embolism,
and is the diagnostic sign with the highest positive predictive value (38%).
Other signs may be present such as the Fleischner sign (enlarged pulmonary artery),
the Hampton hump (peripheral wedge of airspace opacity secondary to lung infarction),
or the Palla and Chang signs (enlarged right descending pulmonary artery sans or with sudden cut-off).
CT pulmonary angiography is the recommended first line diagnostic imaging test in most people,
and besides confirming the occlusive embolus,
better depicts the hypoattenuated peripheral oligemia,
as well as widening and abrupt cut-off of a major pulmonary artery.
Chest radiography- Fig. 28
CT scan- Fig. 29
- Pulmonary artery hypoplasia:
Agenesis or hypoplasia of the pulmonary arteries are among the rarest pulmonary artery anomalies,
with left sided anomalies being reported even less frequently.
They may be associated with deficient or incomplete development of other parts of the lung.
It must be considered as a rare cause of recurrent lower respiratory tract infections in childhood and it should be suspected in asymptomatic patients if a plain chest X-ray shows asymmetric lung fields with a hyperlucent lung and a slightly smaller hemithorax on the affected side.
The affected lung may be hyperlucent due to oligemia,
and because of compensatory hyperinflation,
the contralateral side may also appear hyperlucent.
There often is volume loss,
indicated by elevation of the hemidiaphragm and ipsilateral mediastinal shift.
CT can confirm the diagnosis by showing absence of the main branch of the pulmonary artery.
Chest radiography- Fig. 30
CT scan- Fig. 31
Other causes of decreased pulmonary blood flow as the reason of unilateral hyperlucency,
are congenital heart disease and some of its correction procedures.