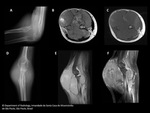
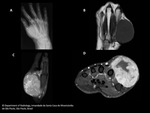
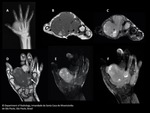
Radiopgraph is usually the first imaging exam performed when patients seek medical attention.
They are normal in about 50% of cases,
particularly when lesions arel small.
Plain radiograph usually show a non-specific round to oval soft-tissue lesion,
usually close to articulations.
Calcification are identified in up to 30%,
and are often eccentric or peripheral within the mass.
Chondroid or osteoid mineralization is rare.
Bone involvement is not rare,
but as SS growth is usyally slow,
when in contact with bones it most commonly determine superficial pressure erosions,
periosteal reaction and osteoporosis.
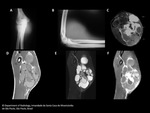
CT typically shows a heterogeneous,
non-infiltrative and well-circumscribed soft-tissue mass with attenuation similar or slightly lower than that of muscle,
often with punctate or peripheral calcifications.
It is better than plain radiograph in identifying small lesions and subtle calcifications as well as in evaluating local bone involvement,
such as erosion or marrow invasion particularly in areas of complex anatomy such as the pelvis,
hip,
or shoulder.
CECT is useful in differentiating SS from cystic lesions and hematomas as it most often shows heterogeneous enhancement.
Areas of nodular enhancement may also be found in synovial sarcomas.
Areas of internal necrosis or hemorrhage are also common.
CT is also the modality of choice to identify pulmonary metastases.
Calcification can sometimes be found in lung nodules.
The US appearance of synovial sarcoma has not been extensively studied.
SS most often present themselves as a nodular,
round or lobulated,
solid mass,
most usually hypoechoic,
that suggests a more slow growing and less aggressive process.
A complex lesion,
with areas of necrosis inside a more echogenic tumor (indicating cellular areas) is the second most common form of appearance.
Doppler evaluation can demonstrate vascularity in the areas of viable tumor,
and is helpful in evaluating biopsy sites.
- · Magnetic Ressonance Imaging
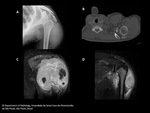
MRI has a superior contrast resolution and is the modality of choice for local staging as well as assessing the intrinsic features of synovial sarcomas.
SS are usually non-specific heterogeneous soft-tissue masses,
but some characteristics can help to differentiate them from other sarcomas.
On T1-wheighted imaging SS present itself as a heterogeneous soft-tissue mass,
usually well-defined with signal intensity equal to slightly higher than that of muscle.
Areas of T1 hyperintensity can also be found and it is usually related to intralesional hemorrhage.
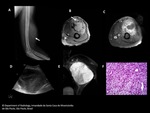
On T2 lesions shows a marked heterogeneity,
with predominant high signal intensity.
The triple sign has been described in T2WI and it is represented by areas of low,
intermediate,
and high T2 signal intensity,
which is thought to be the result of a mix of solid tumor (intermediate T2 intensity),
hemorrhage or necrosis (hight T2 intensity) and calcified/fibrotic areas (low T2 intensity).
Triple sign has been shown to be present in up to 57% of cases.
Fluid levels are also often observed within SS and the combination of cystic areas and/or hemorhagic foci,
creates a bowl of grapes appearance.
Post-contrast imaging usually show heterogenous enhancement,
with marked contrast impregnation in the solid parts of the tumor.
MRI is also useful in post-chemotherapy evaluation,
in which increasing T2 signal intensity is seen as a mark of progressive necrosis.
Tumor size reduction is also a sign of adequate treatment response.
Edema surrounding the tumor is not commonly seen before therapy,
but may develop after adjuvant chemotherapy.
We reviewed 6 cases of synovial sarcomas in the upper extremities from our institution,
all of them with biopsy confirmation.
As reviewed in this text,
they all show the same imaging characteristics as synovial sarcomas of any other sites.