Adrenal abnormalities can be classified according to size,
endocrinologic signature,
morphologic features or biologic behavior.
For the radiologist,
however,
it is more important to acknowledge the imaging features that can help distinguish benign from malignant lesions.
Benign adrenal masses include adrenal hyperplasia,
adenoma,
myelolipoma,
hemorrhage,
adrenal cyst and granulomatous disease.
Malignant adrenal masses include metastasis and lymphoma.
Although the ultrasound is not very accurate to identify the adrenal glands,
it is widely used as a screening exam for assessing any abdominal abnormalities and as a follow-up exam,
as it is inexpensive,
noninvasive and does not use ionizing radiation.
An adrenal mass is far easier to identify using cross-sectional imaging such as CT or magnetic resonance,
and,
since these are used to assess the treatment or staging of oncologic patients,
it is essential that the radiologist distinguish suspicious from benign lesions in adrenal glands.
IMAGING EVALUATION
ULTRASOUND (US)
Ultrasonography plays an important role in identifying abnormalities in the abdomen,
as it is a common examination and can potentially detect a silent lesion in its early stages,
which may greatly affect the prognosis of the patient.
The right adrenal gland can be visualized on coronal and transverse oblique scans through the anterior and middle axillary line,
with the liver acting as an acoustic window.
It is located among the deep margin of the right lobe of the liver,
the inferior vena cava,
and the right crus of the diaphragm,
all of which could be routinely assessed.
The left adrenal gland is visualized on oblique coronal scans mainly through the posterior axillary line,
using either the spleen or the left kidney as an acoustic window.
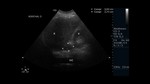
Adrenal abnormality should be suspected when there is a change in the normal shape of the gland,
usually seen as a round mass (Fig. 1).
Some variations in texture are observed in normal glands; therefore,
it is not a reliable characteristic to denote abnormality.
COMPUTED TOMOGRAPHY (CT)
Several studies show that a protocol directed to adrenal evaluation is well suited for the differentiation between benign and malignant tumors.
The interpretation of the imaging findings is more reliable when a combination of unenhanced,
portal and late (15 minutes) phases are realized.
The specificity of this protocol is even greater when the study is performed in patients with known extra-adrenal malignancies who are undergoing examination in search of metastases.
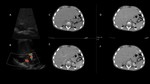
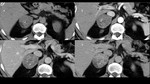
The threshold of 10 HU attenuation on unenhanced CT is suggestive of lipid-rich adenoma and is widely used in clinical practice as a standard,
no contrast-enhanced acquisitions are required for the diagnosis.
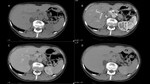
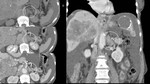
For masses with attenuation above this level,
absolute or relative washout is calculated (Fig. 2) to differentiate between lipid-poor adenoma and non-adenomatous masses.
Absolute washout higher than 60% and relative washout higher than 40% are suggestive of adenomas,
because adenomas are highly vascularized,
and they suffer a significant washout compared to other non-adenomatous abnormalities.
Absence of changes in an indeterminate mass on a follow-up examination after 6 months suggest a benign lesion.
MAGNETIC RESONANCE (MR)
The adrenal glands are very well visualized with MR imaging; therefore,
in some cases,
when there is a suspicious lesion with indeterminate imaging features on CT,
additional imaging exams are requested for further evaluation of the adrenal mass.
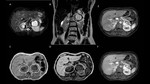
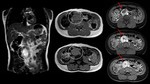
MR images are useful for evaluating the presence of the amount of lipids in the adrenal mass,
separating them into masses with macroscopic or microscopic (intracellular) fat.
Macroscopic fat masses lose signal intensity on fat-saturated images.
However,
the greatest importance of MR lies in the evaluation of the chemical shift phenomenon with in-phase and out-of-phase images,
which is the most sensitive method for differentiating adenomas from metastasis.
Adrenal masses containing intracellular fat lose signal intensity on the out-of-phase if compared to in-phase images.
IMAGING FEATURES OF SPECIFIC ADRENAL DISEASES
ADENOMA
Clinical features
It is the most common tumor found in adrenals,
even in oncologic patients.
Since it is usually asymptomatic,
it ends up representing a large part of the incidentalomas.
Radiologists play an important role in evaluation of these lesions to prevent overdiagnosis,
by not giving emphasis on imaging findings that do not need to be followed,
as they do not represent malignancy and will not change the patient's life expectancy or quality of life,
and further investigation only represents an unnecessary cost.
Adenomas are characterized by the abundant presence of cells with cytoplasm rich in lipids and by a relative and delicate vascular supply network.
Understanding these two characteristics is crucial for a correct interpretation of adenoma imaging findings.
As highlighted earlier,
the presence of a large amount of intracellular lipids is very suggestive of adenoma,
and this is seen both in CT and in MR with tumors with attenuation lower than 10HU,
or which show homogeneous signal decrease on the out-of-phase in MR imaging.
Conversely,
nonadenomatous lesions have higher amount of intracellular water and less lipids; hence,
there is no decrease in signal on out-of-phase.
Adenomas are present in about 3-7% of adults and detected in about 4-5% of the abdominal CT.
They can produce abnormal quantities of hormones,
but more commonly they are not functional.
It is important to remember that adenomas are the most common adrenal tumors even in oncologic patients.
Therefore,
understanding the protocols discussed above to safely exclude metastatic disease directly influences the staging of the patient and,
consequently,
treatment and prognosis.
Imaging findings
- US: Typically,
a well-circumscribed,
round or oval lesion,
slightly heterogeneous mixed echogenicity of less than 3 cm in diameter.
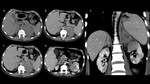
- CT: Also,
a small,
well-circumscribed,
uniform,
with low attenuation mass (<10 HU on unenhanced CT),
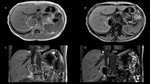
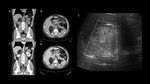
that avidly enhances with contrast media and washes out the agent rapidly (absolute washout > 60% or relative washout > 40%). (Fig. 3)
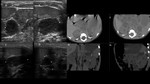
- MR: T1WI and T2WI low to intermediate signal intensity.
Chemical shift imaging with signal loss at out-of-phase T1WI.
Also,
rapidly enhancement and washout after contrast injection.
(Fig. 4)
- Stability at 6 months follow-up exam.
- There is no imaging finding that can reliably differentiate between functional to nonfunctional adenomas.
MYELOLIPOMA
Clinical features
An uncommon benign tumor that is composed of adipose tissue and myelopoietic cells,
in a varied composition.
They are not functional and usually asymptomatic,
unless they grow large enough to cause mass effect or spontaneous hemorrhage.
It is easily identified in any imaging modality because its macroscopic lipid composition.
Imaging findings
- US: Well-circumscribed round or oval lesion that can simulates a renal angiomyolipoma because its proximity with the kidney and hyperechogenicity.
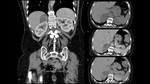
- CT: Low attenuation lesion because of its macroscopic fat is the main imaging feature,
and the diagnosis is accepted when there is at least 50% macroscopic fat (< -30HU) in the adrenal lesion.
If there is a lower amount of lipid content (about 10%),
one must consider the possibility of myelolipomatous metaplasia that can arise from adrenal carcinomas or even adenomas.
Calcifications can be found in up to 20% of cases.
(Fig. 5)
- MR: High fat signal intensity on T1WI and T2WI,
which is reduced on fat-saturated images.
No signal loss at out-of-phase.
PHEOCROMOCYTOMA
Clinical features
Pheochromocytomas are rare adrenal catecholamines-secreting tumors,
originating from chromaffin cells in the adrenal medulla.
Although they are functional tumors,
most of the patients are asymptomatic,
and the lesion is found as an incidentaloma.
The symptoms are related to the adrenergic excess production of hormones such as epinephrine and norepinephrine,
the latter being predominant,
which can cause headache,
facial flushing,
palpitation,
and paroxysmal hypertension.
Unlike other tumors,
benign pheochromocytomas may become large and develop varying degrees of lesion degeneration,
necrosis,
calcification,
fibrosis,
cystic change,
intracellular lipid degeneration or hemorrhage.
Because this broad range of overlapping imaging features with other types of lesions,
pheochromocytoma has earned the nickname of “an imaging chameleon”.
It is also called the “ten percent tumor” because about 10% are bilateral,
10% are extra-adrenal (paragangliomas),
10% occur in children,
10% are malignant and 10% are associated with neuroectodermic syndromes.
Multiple pheochromocytomas tend to be benign,
while extra-adrenal pheochromocytomas,
known as paragangliomas,
are usually malignant.
Imaging features
- US: Adrenal nodule of variable appearance (solid,
solid-cystic,
or cystic),
size,
and echogenicity.
Can be multifocal unilateral or bilateral.
- CT: Round or oval masses of similar attenuation to the surrounding soft-tissue structures at unenhanced CT,
usually 3-5 cm in diameter,
but can reach 10 cm or more.
Variable washout and intracellular-fat can simulate an adenoma.
- MR: Classical appearance of bright T2WI lesions (“light bulb” sign),
for its cystic or hemorrhagic component.
However,
this should not be the only parameter to suggest or exclude the diagnosis of pheochromocytoma.
It may maintain the signal on out-of-phase GRE chemical shift images,
but can have heterogeneous signal drop.
It has intense enhancement with gadolinium due to hypervascularization,
similar to the aorta.(Fig. 6)
- MR imaging is useful for detecting extra-adrenal paragangliomas (Fig. 7) and recurrences after resections due to the high signal on T2WI.
ADRENAL CORTICAL CARCINOMA
Clinical features
The primary carcinoma of the adrenal gland is a rare tumor that arises from the adrenal cortex,
most of which is functioning.
There is a bimodal age distribution,
with peak incidence in 1st decade and middle age (4th and 5th decades).
Of the functioning tumors,
50% manifest as Cushing syndrome,
20% as virilization syndrome,
4% with hyperaldosteronism,
and 4% with both Cushing and virilization syndromes.
Non-functioning tumors are usually larger,
because they are asymptomatic,
and are generally discovered in more advanced stages with presence of local metastasis to adjacent organs such as the liver,
lung,
bone,
regional lymph nodes,
renal or adrenal vein and inferior vena cava; hence,
the worse prognosis.
They may be associated with hemorrhage or necrosis; calcification has been described in 30% of cases.
Imaging features
- US: Round or oblong,
well-circumscribe lesion with lobulated contours,
greater than 6 cm in diameter,
with marked heterogeneous echotexture and hyperechogenicity due to the presence of necrosis,
hemorrhage or calcification.
Functioning carcinomas usually are smaller but can measure up to 6 cm and present as homogeneous hypoechogenicity.
- TC: Well-circumscribed mass,
with heterogeneous attenuation,
usually higher than 10 HU,
with a tendency to do displace regional structures.
Contrast enhancement is also heterogeneous with peripheral predominance,
with slower absolute and relative washout than adenomas.(Fig. 8 and Fig. 9)
- MR: Low T1WI signal and a heterogeneously high intensity on T2WI.
As with CT,
contrast enhanced MR imaging demonstrates a heterogeneous enhancement patter with slow washout.
- Sometimes the imaging features will be inconclusive because some lesions may have higher amounts of intracellular lipids or have a faster washout.
- Despite advances in diagnosis and treatment,
adrenal cortical carcinoma continues to have a poor prognosis.
Early diagnosis with primary resection is required for cure.
METASTASIS
Clinical features
Correct characterization of adrenal mass in oncologic population is critical,
as the presence of metastasis indicates advanced disease,
greatly affecting the patient treatment and prognosis.
The most common tumors to metastasize to adrenal are carcinomas (lung,
breast,
and colon),
malignant melanoma,
and lymphoma.
Usually,
the primary cancer is known,
and bilateral distribution is common.
Despite adenomas being the most common isolated adrenal lesions,
metastases are the most common malignant lesion.
Unfortunately,
the imaging appearance of metastasis is nonspecific.
The investigation using specific adrenal CT protocol can help decide whether the mass is benign or malignant.
In patients with a known primary malignancy elsewhere,
lesions >3 cm tend to be metastasis.
Imaging features
- US: A malignant adrenal mass should be suspected when is larger than 4 cm in diameter,
bilateral.
However,
further investigation with CT and MR are necessary.
- CT: At unenhanced CT,
higher attenuation levels are seen (> 10 HU),
and have slower washout than adenomas on delayed phases (either < 60% absolute or < 40% relative washout at adrenal specific protocol).
When results of CT examinations are equivocal,
MR imaging is the next imaging study of choice for characterizing adrenal lesions.
(Fig. 10)
- MR: Low T1WI signal and increased T2WI signal with progressive enhancement.
However,
the most important diagnostic feature is the lack of signal loss on out-of-phase in comparison to in-phase.
As a rule,
in a patient with a known malignancy,
metastases should be considered unless a definitive diagnosis of a benign lesion can be made.
- In some cases,
a metastasis can occur in a previous adenoma,
or,
less commonly within a myelolipoma.
This arrangement is called “collision tumor”,
which consists of independently coexisting tumors within the same mass.
It represents a diagnostic challenge,
because signal intensity for each tissue type matches that expected for each pulse sequence.
LYMPHOMA
Clinical features
Primary lymphoma of the adrenal gland is rare,
and non-Hodgkin lymphoma is the most common subtype.
Adrenal lymphoma is bilateral in 50% of the cases and is associated with disseminated disease.
Imaging features
- US: Tumors are usually solid mass with variable echogenicity and cystic change.
- CT: Low attenuation mass,
with low level enhancement and slow washout on delayed images.
Usually,
it is seen engulfed by extensive retroperitoneal disease. (Fig. 11)
- MR: Low intensity on T1WI with high signal intensity on T2WI,
with minimal progressive enhancement after contrast material.
MISCELLANEOUS IMAGING FINDINGS
HEMORRHAGE
It can be the result of trauma,
stress,
coagulopathy or underlying adrenal tumors.
Bilateral hemorrhage occurs in 20% of cases,
but adrenal insufficiency secondary to hemorrhage is rare.
It has a variable appearance depending on the amount of blood products that change over time.
(Fig. 12)
ADRENAL CYSTS
Overall,
they are relatively rare.
They can be asymptomatic or grow large enough to cause mass effect.
They are usually seen in 40 to 60-years-old patients.
Adrenal cysts are a heterogeneous group of disorders; therefore,
the cysts are classified into four different categories: vascular,
pseudocyst,
simple cyst,
parasitic cyst (Table 2).
Together,
pseudocysts and vascular cysts represent more than 80% of all adrenal cysts.
HEMANGIOMA
These rare tumors are primarily vasoformative neoplasms that tend to be highly vascular.
They appear as well-circumscribed lesion with phleboliths or calcifications,
peripheral discontinuous nodular enhancement and persistent enhancement on delayed images,
similar to hepatic hemangiomas.
They can be very large when detected,
owing to their indolent nature,
and are usually highly vascular,
demonstrating irregular and profuse enhancement.
(Fig. 13)