Among the 39 patients analyzed,
27 were subjected only to balloon dilatation of the bile ducts; among them,
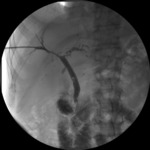
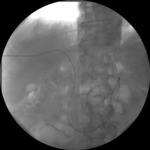
20 were found in the group of primary patency (Fig.
1); namely,
biliary patency was maintained in the long term only with the first round of dilatations.
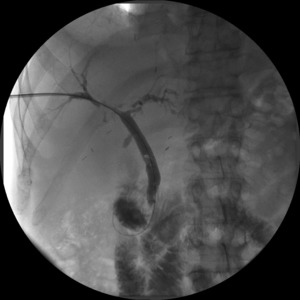
Fig. 1: Cholangiographic control shows primary patency after balloon dilatation.
References: U.O.C. Radiologia Universitaria, Università degli Studi di Padova, Azienda Ospedaliera di Padova - Padova/IT
Compared to the entire cohort,
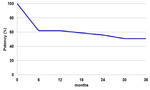
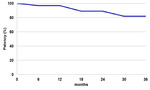
the proportion of patients found in the “primary patency” group was 51% (Table 1).
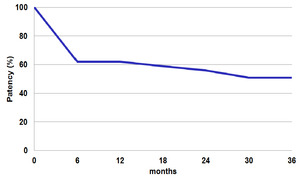
Table 1: Kaplan-Meier chart showing primary success in the management of patients with anastomotic stenosis using balloon dilation only.
References: U.O.C. Radiologia Universitaria, Università degli Studi di Padova, Azienda Ospedaliera di Padova - Padova/IT
In our study,
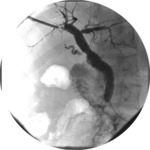
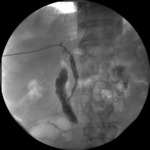
the number of patients belonging to the “secondary patency” group stood at 6 (of 27) (Fig.
2).
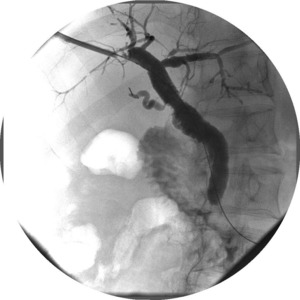
Fig. 2: Cholangiographic restoration of patency with rapid contrast medium transit through the lumen after re-dilatation (secondary patency).
References: U.O.C. Radiologia Universitaria, Università degli Studi di Padova, Azienda Ospedaliera di Padova - Padova/IT
Among all patients analyzed,
those treated effectively with biliary dilation balloon,
belonging to primary or secondary patency groups,
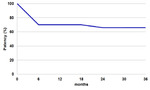
were 66% (Table 2).
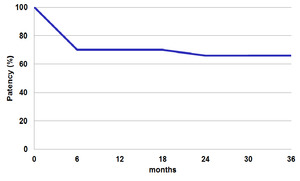
Table 2: Kaplan-Meier chart showing primary or secondary success in the management of patients with anastomotic stenosis using balloon dilation only.
References: U.O.C. Radiologia Universitaria, Università degli Studi di Padova, Azienda Ospedaliera di Padova - Padova/IT
No patient experienced peri-procedural complications in performing bilioplasty.
The results of the stents were then evaluated.
In all cases a metallic stent was placed (Fig.
3),
covered with synthetic material with a mean time to removal of 4.5 months after inserction.
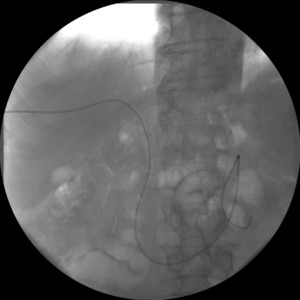
Fig. 3: Cholangiographic control of bare metal stent, correctly positioned.
References: U.O.C. Radiologia Universitaria, Università degli Studi di Padova, Azienda Ospedaliera di Padova - Padova/IT
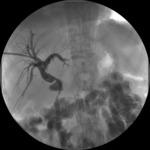
It has been observed that 7 of the 12 patients (58,3%) with a SEMS had an excellent biliary patency (Fig.
4) when we stopped follow-up.
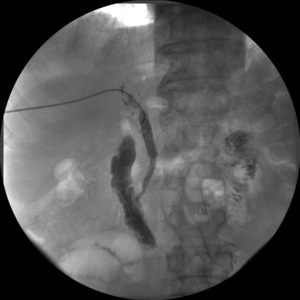
Fig. 4: Cholangiographic control of bare metal stent with rapid contrast medium transit through the lumen.
References: U.O.C. Radiologia Universitaria, Università degli Studi di Padova, Azienda Ospedaliera di Padova - Padova/IT
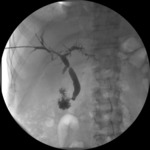
5 patients experienced a biliary restenosis after a variable period of patency (Fig.
5) (6 and 24 months,
mean 16.25 ± 8.73 months).
In 2 of these patients,
we also found the presence of gallstones in the common bile duct.
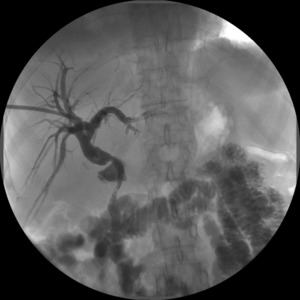
Fig. 5: Cholangiographic control of bare metal stent with incomplete contrast medium transit through the lumen (stent subocclusion).
References: U.O.C. Radiologia Universitaria, Università degli Studi di Padova, Azienda Ospedaliera di Padova - Padova/IT
In one case,
the stent removal was performed urgently,
due to the onset of acute pancreatitis.
This patient was excluded from the analysis.
For 5 patients the final therapeutic solution was a surgical revision with re-evaluation and creation of a new anastomosis.
Considering the case of acute pancreatitis,
overall,
the procedures were properly carried out,
without any complications,
in 97.4% of cases.
In our study,
there was a single case of dilatation failure (Fig.
6),
stenosis lasted even after multiple dilatation cycles.
This patient required early surgical revision of the anastomosis.
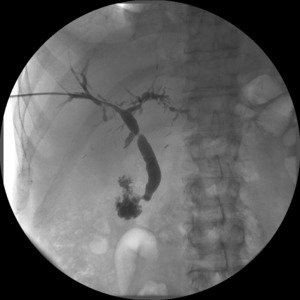
Fig. 6: Percutaneous cholangiographic control in patient with stenosis' dilatation failure after balloon bilioplasty.
References: U.O.C. Radiologia Universitaria, Università degli Studi di Padova, Azienda Ospedaliera di Padova - Padova/IT
The percentage of patients treated with success with balloon dilatation or stenting was,
after 36 months of observation,
81% (Table 3).
An excellent response (100% of patency) was observed in patient with C-C anastomosis,
while patients with bilio-digestive anastomosis showed a patency of 61% after 36 months.
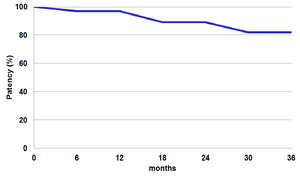
Table 3: Kaplan-Meier curve shows that the percentage of patients treated with success with balloon dilatation and stenting is 81%, after 36 months.
References: U.O.C. Radiologia Universitaria, Università degli Studi di Padova, Azienda Ospedaliera di Padova - Padova/IT
Strong reduction of cholestasis and cytolisis enzymes after 180-240 days was observed (Table 4).
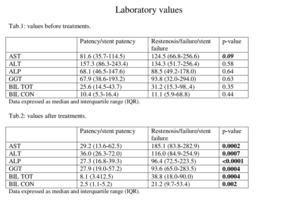
Table 4: Comparison charts of laboratory values before and after the treatment.
References: U.O.C. Radiologia Universitaria, Università degli Studi di Padova, Azienda Ospedaliera di Padova - Padova/IT
Our study has limitations.
First,
it is a retrospective evaluation; second,
because no clear therapeutic algorithm has yet been reported to date,
we used our own criteria to assess the therapeutic effect.
Third,
our study group was small,
and additional studies are needed to further assess the role of this method.