Imaging modalities [2,
5,
6]:
- US/DopplerUS is the first imaging modality for the evaluation of liver graft dysfunction in vascular as well as in biliary complications;
- MR is a problem solving modality,
especially thanks to its angiographic and cholangiographic sequences and the lack of ionizing radiations;
- CT is the imaging technique of choice in emergency,
it can also be used as a guide to percutaneous aspiration and fluid collection drainage;
- interventional radiology techniques allow the detection and treatment of vascular and non-vascular complications in pediatric LT,
with potential improvement in patient's and graft's survival.
The main procedures are: angiography,
pressure gradient measurement,
percutaneous transhepatic cholangiography,
percutaneous and transjugular liver biopsy,
thrombectomy,
percutaneous thrombolysis,
vascular and biliary stent placement,
balloon angioplasty,
balloon dilation,
drainage [4,
6,
7].
Our experience: we reviewed 81 pediatric patients who underwent a LT in our Institution between 1996 and 2016.
Our results are summarized in the following table (Table 1 and 2).
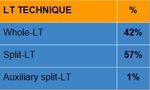
Table 1
References: Radiology Unit - Department of Medicine - University Hospital of Padova
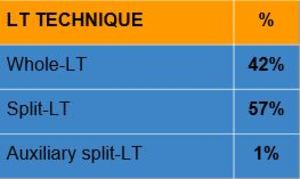
Table 2
References: Radiology Unit - Department of Medicine - University Hospital of Padova
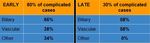
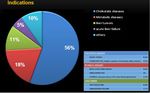
Complications were radiologically evaluated in 49,38% of cases (Table 3).
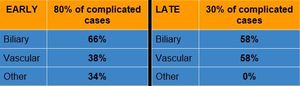
Table 3
References: Radiology Unit - Department of Medicine - University Hospital of Padova
The event of more than one complication was frequent:
- early + late complications in 10% cases
- among early complications: both biliary + vascular and biliary + other had a rate of 19%
- among late complications: biliary + vascular complications had a rate of 17%
Our case series of complications is shown below:
Early biliary complications:
- duct-to-duct anatomosis stricture
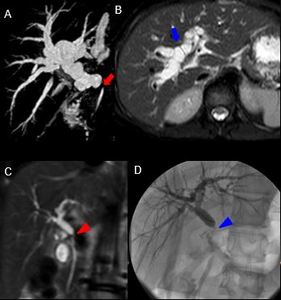
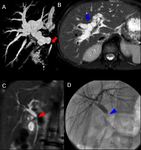
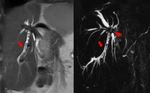
Fig. 5: A cholangiography MR sequence (A) and an axial T2-weighted SPAIR image (B) showing a duct-to-duct anastomosis stricture (red arrow) associated with intrahepatic bile ducts dilatation (blue arrow), 2 weeks after whole-LT in a 11-year-old girl.
A coronal T2-weighted MR sequence (C) showing the duct-to-duct anastomosis stricture (red arrowhead) 28 days after whole-LT in a 14-year-old girl.
The stricture was confirmed by a percutaneous cholangiography (D), that shows the lack of contrast medium transit through the anastomosis (blue arrowhead).
References: Radiology Unit - Department of Medicine - University Hospital of Padova
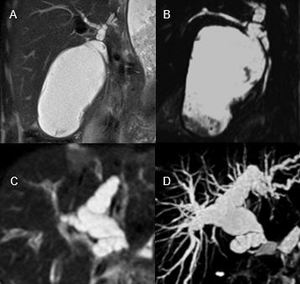
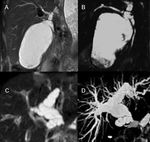
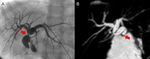
Fig. 6: A case of massive cystic duct mucocele associated with biloma occurred 29 days after a right split-LT, as shown by a T2-weighted image (A) and a cholangiography MR sequence (B), in a 13-year-old boy.
Another case of early cystic duct mucocele, associated with intrahepatic bile duct dilatation in a 2-year-old girl, 10 days after the whole-LT, shown in a T2-weighted image (C) and in the cholangiography MR sequence (D).
References: Radiology Unit - Department of Medicine - University Hospital of Padova
Late biliary complications:
- lithiasis and biliary-jejunal anastomotic stricture
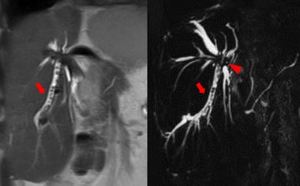
Fig. 7: A 18-year-old boy with biliary lithiasis (red arrow) and biliary stent occlusion, previously positioned for a biliary-jejunal anastomosis stricture (arrowhead).
References: Radiology Unit - Department of Medicine - University Hospital of Padova
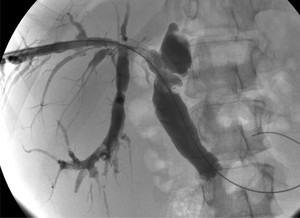
Fig. 8: In the same patient, in-stent restenosis was treated with a percutaneous intervention.
References: Radiology Unit - Department of Medicine - University Hospital of Padova
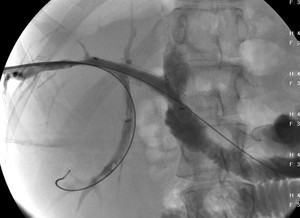
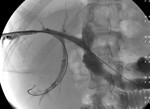
Fig. 9: Post-procedural cholangiography showing stent patency in the previous patient.
References: Radiology Unit - Department of Medicine - University Hospital of Padova
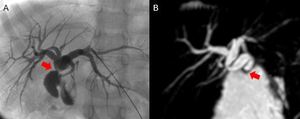
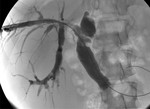
Fig. 10: Biliary-jejunal anastomosis stricture (red arrow) in a 3-year-old girl 2 years after a whole-LT, shown in percutaneous cholangiography (A) and cholangiography MR (B), with slight intrahepatic bile ducts dilatation.
References: Radiology Unit - Department of Medicine - University Hospital of Padova
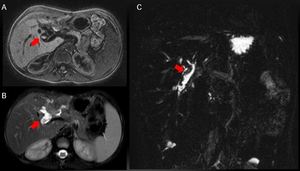
Fig. 11: Biliary plugs (red arrows) in a 9-year-old girl with cholestasis 7 months after a right split-LT, demonstrated by axial T1-weighted GE SPIR (A) and T2-weighted SPAIR (B) sequences and cholangiography MR (C).
References: Radiology Unit - Department of Medicine - University Hospital of Padova
Biliary cast syndrome (BCS) [8]:
BCS is a biliary obstruction that can complicate up to 18% of liver transplantation recipients,
caused by the presence of endoluminal biliary debris and casts,
containing bilirubin,
bile acids and fragments of cholangiocytes.
It is usually diagnosed with endoscopic retrograde cholangiopancreatography (ERCP),
percutaneous transhepatic cholangiography (PTC) and/or MRI.
Biliary casts are seen as endoluminal hyperintensities on non-enhanced T1-weighted images and signal voids on cholangiopancreatography sequences.
With the combination of these sequences,
MRI can be considered the modality of choice for the diagnosis of BCS,
especially in pediatric patients,
due to the lack of ionizing radiations and invasivity.
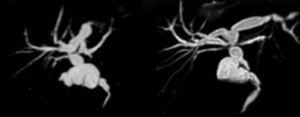
Fig. 12: Cystic duct mucocele can also occur later. The two cholangiography MR images show a case of late mucocele 2 years after a whole-LT in a 4-year-old boy.
References: Radiology Unit - Department of Medicine - University Hospital of Padova
Early vascular complications:
- hepatic artery thrombosis
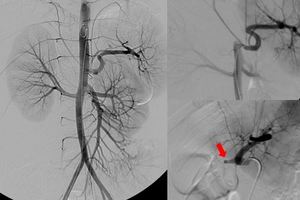
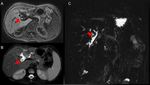
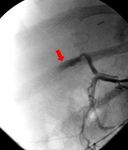
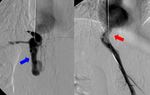
Fig. 13: A 9-year-old girl with hepatic artery thrombosis 22 days after right split-LT: arteriograms demonstrate proximal occlusion of the hepatic artery (red arrow).
References: Radiology Unit - Department of Medicine - University Hospital of Padova
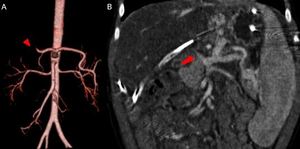
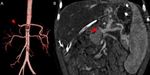
Fig. 14: A case of combined vascular complications in a 2-year-old girl 2 days after a whole-LT: (A) hepatic artery thrombosis (red arrowhead) and (B) portal vein thrombosis (red arrow) with diffuse liver hypoperfusion.
References: Radiology Unit - Department of Medicine - University Hospital of Padova
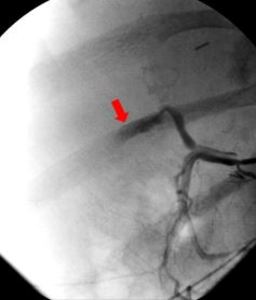
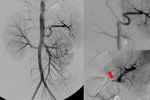
Fig. 15: A 2-year-old boy with hepatic artery thrombosis, 11 days after the liver transplantation: the image shows interruption of the hepatic artery, lack of intrahepatic vascularization and leakage (red arrow).
References: Radiology Unit - Department of Medicine - University Hospital of Padova
Late vascular complications:
- portal vein thrombosis and cavernoma
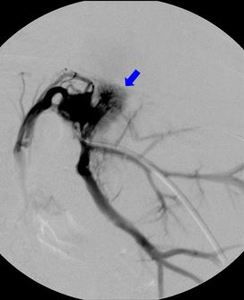
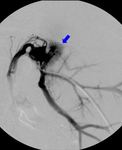
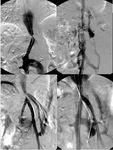
Fig. 16: A 18-month-old girl with extrahepatic portal vein thrombosis and subsequent development of cavernoma, 6 months after the left split-LT. Portography shows the cavernomatous vessels (blue arrow).
References: Radiology Unit - Department of Medicine - University Hospital of Padova
- portal vein anastomotic stenosis

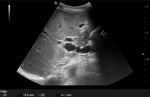
Fig. 17: US imaging of a portal vein anastomotic stenosis developed 6 years after whole-LT in a 18-year-old girl.
References: Radiology Unit - Department of Medicine - University Hospital of Padova
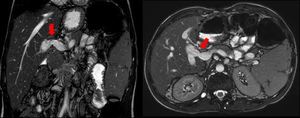
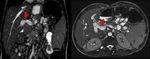
Fig. 18: A 12-year-old boy who developed portal vein anastomotic stenosis (red arrows), 3 years after the right split-LT, as shown in balanced-SSFP sequences.
References: Radiology Unit - Department of Medicine - University Hospital of Padova
- hepatic artery anastomotic stenosis
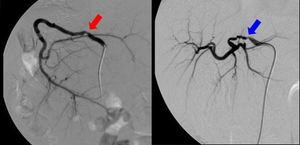
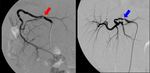
Fig. 19: A 2-year-old girl with 50% hepatic artery anastomotic stenosis (red arrow) 3 months after left split-LT.
Another 2-year-old girl with 70% hepatic artery anastomotic stenosis (blue arrow) 10 months after whole-LT.
References: Radiology Unit - Department of Medicine - University Hospital of Padova
- hepatic vein - inferior vena cava stenosis
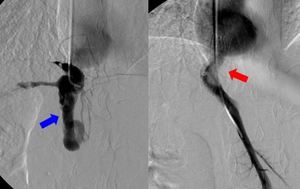
Fig. 20: A 13-year-old boy with hepatic vein stenosis and collateral vessels (blue arrow), developed eleven years after the split-liver transplantation and treated with several angioplasties and a stent positioning (red arrow).
References: Radiology Unit - Department of Medicine - University Hospital of Padova
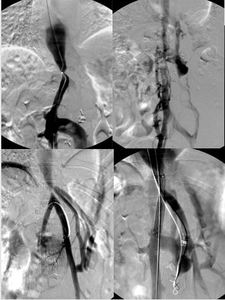
Fig. 21: A 9-year-old girl with hepatic vein stenosis and collateral vessels, developed 9 years after the split-liver transplantation and treated with PTA and a stent positioning.
References: Radiology Unit - Department of Medicine - University Hospital of Padova
Miscellaneous:
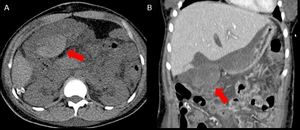
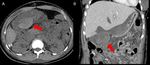
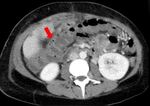
Fig. 22: CT images before (A) and after (B) contrast medium injection show a intra-peritoneal perihepatic hematoma (red arrows) occurred 5 days after whole-LT.
References: Radiology Unit - Department of Medicine - University Hospital of Padova
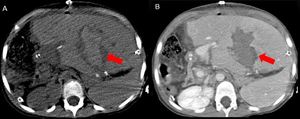
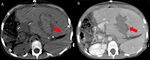
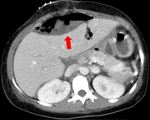
Fig. 23: CT images before (A) and after (B) contrast medium injection show an intrahepatic hematoma (red arrows) 2 weeks after left split-LT.
References: Radiology Unit - Department of Medicine - University Hospital of Padova
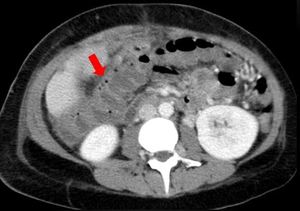
Fig. 24: CT image, performed 10 days after whole-LT, showing gas bubbles inside the transverse colon wall (red arrow). The surgical re-intervention demonstrated multiple transverse colon perforations.
References: Radiology Unit - Department of Medicine - University Hospital of Padova
- intra-abdominal fluid collection containing gas
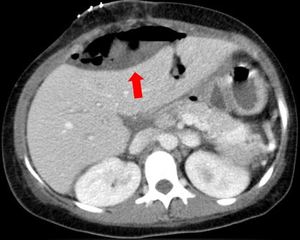
Fig. 25: A case of perihepatic fluid collection containing gas (red arrow) occurred 10 days after whole-LT.
References: Radiology Unit - Department of Medicine - University Hospital of Padova
- iatrogenic bezoar with small bowel occlusion
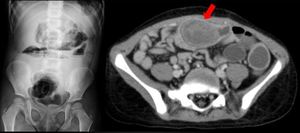
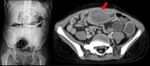
Fig. 26: A curious case of small bowel subocclusion 3 years after whole-LT: contrast-enhanced CT showed the presence of a dishomogeneous mass (red arrow) inside the ileum. Surgical intervention demonstrated a bezoar made of contrast medium from multiple previous percutaneous biliary procedures.
References: Radiology Unit - Department of Medicine - University Hospital of Padova