Keywords:
Musculoskeletal soft tissue, Obstetrics (Pregnancy / birth / postnatal period), MR, Diagnostic procedure
Authors:
R. M. O'Cearbhaill, H. Moriarty, E. R. Stanley, T. Geoghegan, L. Lawler; Dublin/IE
DOI:
10.1594/ecr2018/C-2749
Results
A total of 77 studies were included.
51 were performed during pregnancy and 26 during the post partum period.
The average patient age was 34.
29.9% of patients had musculoskeletal findings.
Focusing on the prepartum group,
the average weeks gestation was 26.9,
ranging from 9 to 40 weeks.
Musculosketetal pathology was found in 10 studies (22%).
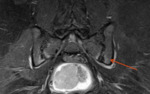
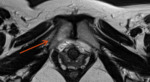
Findings can be divided into those relating directly to pregnancy – pubic symphysis oedema in 4 patients,
oedema of the sacroiliac joints in 2 patients and ps diasthesis in one patient.
Findings where it was unclear whether they related to pregnancy included disc bulge and subcutaneous fluid collection.
Four patients had incidental findings of tarlov cysts.
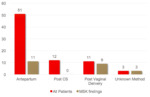
Regarding the postpartum group of patients, 46% had delivered via a caesarean section and 42% via vaginal delivery.
The method of delivery was unknown in 12% of patients.
Compared to the prepartum group,
where only 22% had MSK findings,
a large proportion of postpartum patients were found to have MSK morbidity on MRI with 13 patients (50%) affected.
None of the patients who underwent CS had MSK findings,
90% of those who had undergone vaginal delivery and all patients where the method of delivery was unknown were affected.
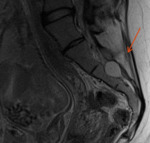
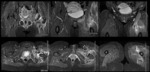
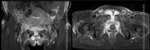
Ten patients had oedema of the pelvic bones and musculature,
in some cases amounting to post traumatic myopathy,
2 patients had pubic symphysis diastasis and one patient was foud to have a lower vaginal fistula.
In comparing MSK findings in the prepartum and postpartum groups,
there is a greater proportion of major finding related directly to pregnancy in the postpartum group.
In the prepartum group there was a much greater proportion of incidental findings and minor changes relating to pregnancy.
With regards to follow up,
the majority of patients had no follow up at our institution.
8 patients were followed up in our hospitals neurology outpatients clinic.
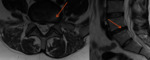
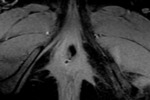
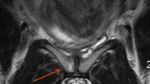
One patient had persisten pudendal neuropathy which required a sacral nerve stimulator,
an example of which is shown on the right.
4 patients had mild neurological deficits at 1 year of follow up and were subsequently lost to follow up.
1 patients had a resolved deicit when seen at 2 years post partum.
2 patients had known neurological deficits following delivery but were not followed up beyond that.