Paragangliomas of the head and neck are rare tumours,
representing <0.5% of all head and neck tumours.
Overall,
there is a 3:1 female predominance,
with two-thirds of cases being diagnosed between the ages of 40 and 60.
The classic manifestation of a carotid body tumor is a nontender,
enlarging lateral neck mass which is mobile,
pulsatile and associated wiht a bruit.
The jugulare and tympanicum tumors commonly cause pulsatile tinnitus and hearing loss and may cause cranial nerve compression.
Vagal paraganglioms are the least common and present as a painless neck mass which may result in dysphagia and hoarseness.
Presentation is with pulsatile tinnitus,
cranial nerve palsies (typically IX-XI,
Vernet syndrome),
or conductive hearing loss.
One particular feature of head and neck paragangliomas is that they tend to be innervated by the parasympathetic system.
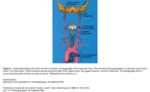
Carotid body tumour:
Arise from paraganglia located in the “crotch” of the carotid bifucation (most common location).
Pathognomonic finding is “splaying” of the External carotid artery (ECA) and Internal carotid artery (ICA) and “filling” the bifucation.
Multiple in 5%-14% of sporadic cases and up to 33% in familial cases.
Only 8% of these lesions are large enough to present as carotid space mass; may have X and/or XII neuropathy.
Malignant in 10%-15% of cases.
Fig (1,2).
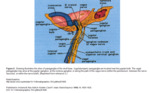
Glomus tympanicum tumour:
Arise from the glomus tympanicum confined to the middle ear, overlying the cochlear promontory, arises from the inferior tympanic branch of glossopharyngeal nerve (Craneal Nerve IX) (or Jacobson's nerve).
Second most common head and neck paraganglioma.Fig (2,3).
Glomus jugulotympanicum tumour:
Early symptoms: conductive hearing loss,
pulsatile tinnitus
Slow growth but locally invasive.
Mortality rate: 15%.
Metastasis are very rare.
Pathology: chief cells (“Zellballen”),
sustentacular cells.Fig (2,3).
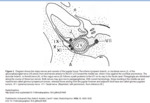
Glomus jugulare tumour:
Arise in adventitia of interna jugular vein (IJV),
from Arnold’s nerve (IX) and Jacobson’s nerve (X).
Represent the most common tumor found in the jugular foramen.
Permeative erosive changes with amputation of the jugular spine
demonstrated on CT.
It is multicentric in 5% of sporadic cases and up to 25% in familial cases
Symptoms: Pulsatile tinnitus; IX-XI cranial neuropathy +/- XII
Malignant with metastasis in approximately 3%.Fig (3).
Glomus vagale tumour:
Arise from paraganglia located around nodose ganglion,
the more caudal of the two vagal ganglia.
Situated just below skull base,
lower than typical jugulare lesions and higher than typical carotid body tumors.
Usually lie entirely within carotid space (post-styloid parapharyngeal space).
As vagus nerve lies dorsal to ICA,
these tumors usually displace ICA anteriorly
Approximately 10% incidence of malignancy.