Imaging is the primary diagnostic examination for glomus tumors of the head and neck.
Contrast-enhanced computed tomography (CT) scanning,
magnetic resonance imaging (MRI),
scintigraphy and angiography can be performed for proper diagnosis and localization of the tumors.
They are divided according to location:
- Carotid body tumour
- Glomus tympanicum tumour
- Glomus jugulotympanicum tumour
- Glomus jugulare tumour
- Glomus vagale tumour.
Radiographics Features
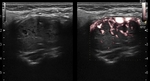
Ultrasound: Useful as the first step in assessment but not the last.
Inexpensive.
Non-invasive.
Readily available.
Ultrasonographic (US) evaluation of paragangliomas is limited to those that occur exclusively in the neck.
US is best in the detection and followup of cervical paragangliomas and in the detection of small paragangliomas.
A preliminary US study of the lateral neck is performed (with a 5-MHz transducer) for tumor localization,
followed by a high-resolution study (with a 7.5–10-MHz transducer) for tumor characterization.
In general,
skull base masses are poorly evaluated with US.Duplex Doppler imaging and color Doppler imaging demonstrate the intrinsic hypervascularity of the cervical paraganglioma and the characteristic splaying of the common carotid bifurcation in carotid body tumors. Fig (4).
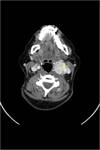
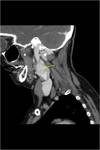
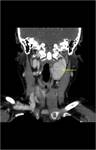
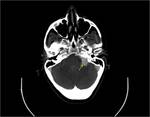
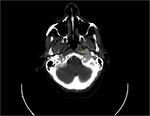
CT: is excellent for defining the exact location of a mass and visualizing its effect on adjacent structures.
Combined with a knowledge of anatomy and epidemiology,
it can help distinguish among congenital,
inflammatory,
and neoplastic processes that all result in neck masses.
It is quicker and more available than MRI. Useful when bone erosion occurs.
Smoth-eaten pattern is typical.
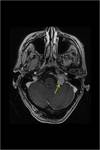
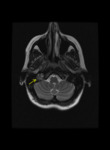
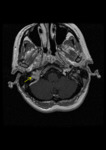
MRI: helps diagnose paragangliomas by representing their hypervascularity as multiple low-signal areas due to flow void.
It is superior to CT scanning in delineating these tumors and in distinguishing them from inflammation and hemorrhage.
MRI is also better able to demonstrate the relationship of carotid body tumors to adjacent vascular structures.
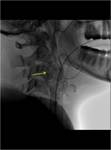
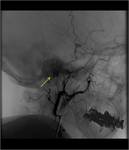
Angiography
Should demonstrate an intense tumour blush,
with the most common feeding vessel being the ascending pharyngeal artery.Fig.(9,13).
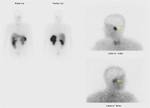
Scintigraphy
This tumors demonstrate high uptake with 111In-ctreotide.
Fig (8).
Typical radiological characteristics of these tumours are,
as follow:
Carotid body tumour:
Carotid body tumours are located at the carotid bifurcation with characteristic splaying of the ICA and ECA,
described as the lyre sign.
In all modalities,
the dense vascularity of these tumours is manifested as prominent contrast enhancement.
Contrast enhanced CT is excellent at depicting these lesions.
Typical appearances are:
- Soft tissue density on non-contrast CT (similar to muscle)
- Bright and rapid (faster than schwannoma) enhancement
- Splaying of the ICA and ECA.
Fig.
(5,6,7).
MRI
T1
- iso to hypointense compared to muscle
- "salt and pepper" appearance when larger,
representing a combination of punctate regions of haemorrhage or slow flow (salt) and flow voids (pepper).
-intense enhancement following gadolinium
T2
- hyper intense compared to muscle
- "salt and pepper" appearance also seen on T2
Glomus tympanicum tumour
CT demonstrate a round mass with flat base on the cochlear promontory proyecting in to the mesotympanum.
Larger lesion may resemble "New jersey" on coronal image when fill middle ear cavity.
Focal enhancing mass on cochlear promontory. Fig.(10,11,12).
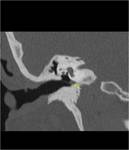
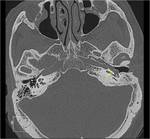
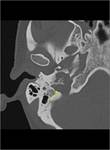
Glomus jugulotympanicum tumour
CT: irregular margins,
“moth-eaten” erosion
Glomus jugulare: may extend down carotid sheath.Fig.
(14,15).
MR: “Salt and pepper” appearance. “Salt”: hyperintense foci (slow flow,
hemorrhage).
“Pepper”: serpentine flow voids
Intense enhancement. Fig.
(16).
Angiography: ascending pharyngeal artery. Fig.(9).
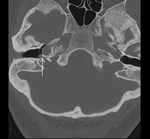
Glomus jugulare tumour
Bone CT demostrates a mass in the yugular foramen with "permeative- destructive" changes of the adyacent bone.Fig.(17).
MR:
T1W1 greater than 2 cm demostrates characteristic "salt and pepper" appearance.
T2W1 shows mixed hyperintense mass with flow voids.
Intence enhancement. Fig.(18,19).
Glomus vagale tumour
Avidly-enhancing ovoid carotid space mass.
Anteromedial displacement of ICA and posteriolateral displacment of internal jugular vein.
No widening of the carotid bifurcation.
MRI imaging findings similar to carotid body paraganglioma.
Ultrasound
Difficult to sonographically differentiate between other lesions that can potentially occur in this location.
May be seen as a solid heterogeneously hypoechoic lesion comprising of small vascular structures.
MRI
T1: usually low signal
T2: high signal with multiple flow voids which may give a salt and pepper appearance.
T1C+: intense enhancement