1.
Fungal infections
1.1.
Aspergillus fumigatus
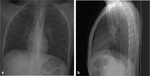
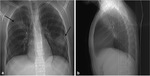
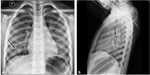
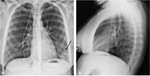
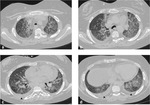
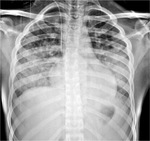
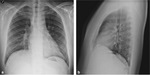
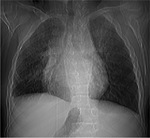
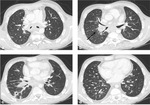
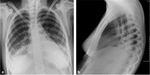
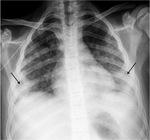
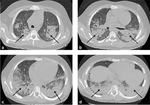
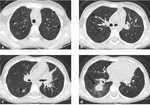
The chest radiographic findings of diffuse infiltrates in children is different from those of adults and bilateral involvement and respiratory insufficiency are negative prognostic factors [8] [Fig. 1 - Fig. 2].
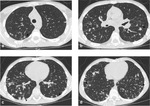
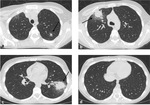
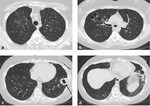
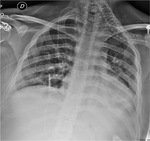
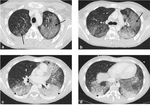
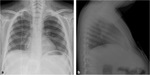
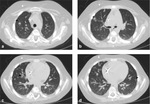
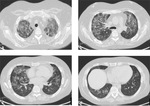
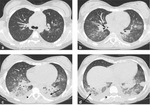
In invasive pulmonary aspergillosis there are many radiological findings including round pneumonic infiltrates,
peripheral wedge-shaped opacity and the characteristic “halo sign” around pneumonic infiltrates [9] [Fig. 3 - Fig. 4 - Fig. 5 - Fig. 6].
The “halo sign” is a zone of ground-glass opacity surrounding nodules or a pulmonary mass and represents the ring of haemorrhage which surrounds septic infarction [10].
During the resolution phase of the illness,
radiography or CT show “air crescent sign”: this corresponds to an air-filled space,
due to the resorption of necrotic tissue at the peripheral region of the lesion [11] [Fig. 7 - Fig. 8].
1.2 Candida albicans
The most frequent appearance in Candida Albicans infection is a focal or multilobar consolidation,
sometimes with linear lesions suggesting an interstitial component.
HRCT shows multiple nodules,
poorly defined or circumscribed,
with areas of ground-glass.
Rare is presence of limphadenomegaly and cavitation [Fig. 9 - Fig. 10].
1.3 Pneumocystis jirovecii
The early radiologic chest findings are peri-hilar ground-glass opacities,
thickning interstitial and poor definition of pulmonary vessels. Characteristic is the absence of pleural effusion.
At HRCT,
extensive ground-glass opacity is the principal finding for accumulation of intraalveolar fibrin,
debris and organism,
with a predilection for the upper lobes [12] and peri-hilar regions.
In advanced stages,
septal lines superimposed on ground-glass opacity (“crazy paving”) [13] and consolidation can be observed [14] [Fig. 11 - Fig. 12].
In many cases,
the pathogenic agent determines the presence of a small cystic area,
pneumatoceles; these air-space are characteristically thin-walled,
involve mainly upper lobes and predispose the development of pneumothorax.
1.4 Coccidioides immitis
When this pathogenic agent determines chest radiographic characteristic findings,
air-space consolidation is observed,
more appreciable in lower lobes.
This consolidation tends to resolve and to reappear in another area (“phantom infiltrates”),
associated with limphadenomegaly and pleural effusion.
The primary infection shows increasing multifocal pneumonia or multiple nodules,
with or without cavitation.
In rare cases,
the consolidation can evolve into a peripheral nodule with central cavitation,
determining a thin-walled small cyst (“grapeskin”),
which spontaneously tends to resolve.
More frequent is the presence of a single nodule rather multiple nodules with a low tendency to calcification.
1.5 Cryptococcus neoformans
In immunocompromised children a diffuse interstitial pattern is observed,
described as reticular or nodular,
similar to P.jirovecii infections.
Miliary nodular pattern,
singular nodule or multiple nodules,
sometimes cavitated,
can be detected.
Presence of lymphadenomegaly and pleural effusion is rare [Fig. 13 - Fig. 14].
2.
Viral infections
2.1 Cytomegalovirus
Lobar consolidation,
diffuse and focal ground-glass opacities and irregular reticular opacities are the main findings on plain chest radiographs and chest CT,
caused by partial filling of alveolar space,
collapse of alveoli and interstitial thickening [15].
[Fig. 15 - Fig. 16] In many cases,
multiple miliary nodules or small nodules with associated peripheral areas of ground-glass can be osserved ("halo sign") [16].
2.2.
Herpes Simplex
In immunocompromised patients the common findings regarding HSV pneumonia are patchy lobular,
subsegmental or segmental consolidations and diffuse ground-glass opacities; centrolobular nodules and tree-in-bud pattern can occur in HSV2 patients [17] [Fig. 17 - Fig. 18].
2.3 Varicella Zoster
This pathogenic agent determines multicentric hemorrhage and necrosis centered on airways [18].
Multiple nodules,
measuring 5-10 mm in diameter,
are the main findings; halo of groud-glass opacity,
coalescent nodules and multiple groud-glass opacity can manifest.
A miliary distribution can occur [19].
In rare cases,
these nodules can calcify and in later stages,
2-3 mm densely calcified nodules can be randomly observed [20].
2.4 Influenza virus
Chest radiograph shows poorly definied and irregular consolidations,
measuring 10-20 mm,
which tend to become confluent.
In HRCT diffuse or patchy ground glass opacities and small centrilobular nodules are frequently seen.
Pleural effusion is rare.
3.
Bacterial infections
3.1 Streptococcus pneumoniae
In immunocompromised children S.
Pneumoniae is the most common cause of bacterial pneumonia [21].
It occurs in alveolar/lobar pneumonia on chest radiography and CT and affects mainly lower lobe; multi-lobe involvement is also common.
This pathological manifestation may be complicated by empyema,
pneumatocele or lung abscess.
A severe and persistent infective pathology may lead to chronic lung disease,
such as bronchiectasis [Fig. 19 - Fig. 20 - Fig. 21 - Fig. 22]
Other causes of bacterial pneumonia in immunocompromised children include gram negative pathogens such as H.
Influenzae,
P.
aeruginosa,
E.
Coli and K.
Pneumoniae.
3.2 Mycobacteria (M.
tubercolosis,
M.
bovis,
M.
avium)
M.
tubercolosis is the commonest pathological agents among mycobacteria,
but localized or dissiminated infection from M.
bovis or M.
avium may occur.
In particular regions where TB has high prevalence,
M.
tubercolosis is an important etiological cause of chronic respiratory infection in immunocompromised children [22].
On chest radiography,
the most common finding is air-space consolidation; occur multiple nodules,
associated to controlateral air-space consolidation,
also occur frequently.
Less frequent is the detection of cavitated nodules,
extra-pulmonary spread or miliary pattern [23].
In many cases mediastinal bulging is appreciated and suggests mediastinal or hilar lymphadenopathy.
On chest CT scan air-space consolidation in the upper lobes is the lesion mainly detected,
associated with multifocal low-attenuation areas and cavitation within the consolidation.
Rarely the pathology shows a necrotic cavity within the consolidation and bilateral bullous lesions.
Mediastinal and hilar lymphadenopathies with central low attenuation,
peripheral enhancement and small calcification levels were frequently observed; bronchiectasis and pleural effusion occur.
4.
Protozoal and helminth infenctions
Protozol and helminth parasitic pneumonias and lung involment are rare and most commonly occur in the tropics [24].
Chest radiographic features of Plasmodium falciparum are lobar consolidations,
bilateral pulmonary infiltrates,
bilateral alveolar opacities and basal ground-glass opacities [25].
Pulmonary manifestations of Toxoplasma gondii are interstitial pneumonia,
diffuse alveolar damage,
necrotizing pneumonia and obstructive or lobar pneumonia [26].
In immunocompromised children,
among other pathological agents that rarely cause interstitial or lobar pneumonia,
there are: Entamoeba histolytica,
Leishmania donovani or infantum and Tripanosoma brucei and cruzi.