We retrospectively analized the results of 30 consecutive CT-guided hook-wire localization prior to VATS for pulmonary lesions resection,
between May 2013 and June 2017 at our institution.
Thirty lesions: 17 women,
13 men.
Median age 64 years old; range 41-78).
History of extrapulmonary malignancy in 14 of them.
The nodules diameter ranged from 6 to 24 mm (mean 11,53 mm),
measured on axial CT.
19 lesions were ≤ 10 mm (63.33 %).
Distance from the pleura to the outer border of target was 0 - 45 mm (mean 12,53 mm).
GGO or mixed pattern was present in 23 lesions (76.66%)
Median procedure time 14.66 min (range 8-25 min).
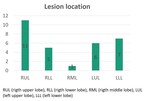
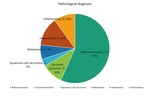
Location and pathological results are reflected in fig.1 and fig.2 respectively.
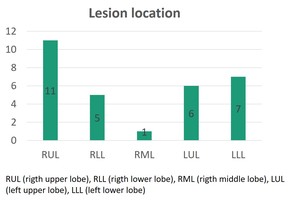
Fig. 1
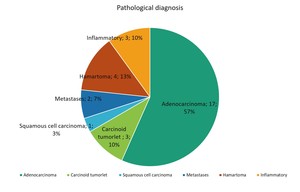
Fig. 2
INDICATIONS:
Small pulmonary nodules of unclear aethiology,
in patients with or without prior history of cancer,
selected for thoracoscopic resection.
The objetive can be diagnostic and/or therapeutic.
CONTRAINDICATIONS:
- Inability to identify an appropiate needle path way
- Uncorrectable coagulopathy
- The mayority of other cotraindications are relative: uncooperative patient,
anticoagulation therapy,
severe emphysema,
deep lesions,
proximity to the mediastinal great vessels...
PREPROCEDURE ASSESSMENT
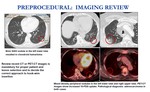
- Review of a chest CT or PET-CT scan is mandatory for patient selection and for planning the route to hook-wire placement.
The indication of localization and the proper access route should be in consensus with the thoracic surgeon.
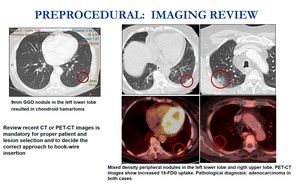
Fig. 3
- Assess the coagulation status.
- Withheld anticoagulant or antiplatelet treatment for a variable period depending on the type of drugs used.
We don´t discontinue 100mg aspirin.
- Obtain informed consent.
THECNIQUE
The wire placement is performed in the CT room at a maximum of two hours before surgery.
The tecnique for hook wire placement is similar to that for percutaneous needle lung biopsy.
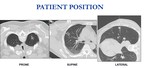
Patient position depends on the location of the nodule (prone position in 15,
lateral position in 12 and supine position in 3 of our patiens).
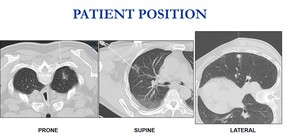
Fig. 4
A Ct scan with sections of 3 mm thickness (length limited to the expected site of the lesion) is performed with a metallic grid pattern on the skin above the region of interest.
That is fundamental to stablish the pathway,
puncture site and distance to the lesion.
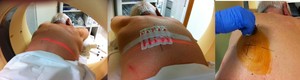
Fig. 5: The puncture point is determined using the CT gantry lights and the grid on the patient’s skin. This point is drawn with a permanent marker. Skin is sterilized (povidone iodine, clorhexidine...)
The shortest and safest route is choosen (avoid vessels in the thoracic wall,
large pulmonary vessels and visible bronchi).
Whenever possible,
do not traverse fissures,
although transfissural route may be eligible if permits a considerable shortening of the distance pleura-nodule.
After sterilization of the skin and local anesthesia injection (lidocaine 1-2%),
the needle housing the hookwire is inserted gradually puncture cannula is advanced near the target,
but not onto it.
Sequential CT scans are obtained to monitor the advance of the needle as needed. Another CT image is obtained to evaluate the tip position,
and if it is adecuate,
the hooked wire is released and anchored within the tumor,
and the cannula is carefully withdrawn.
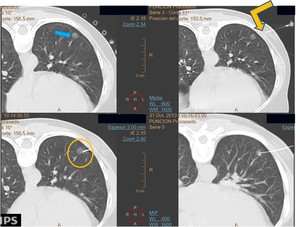
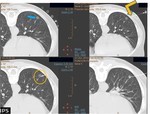
Fig. 6: Initial Ct scan shows a 10mm ground-glass nodule in the left lowerlobe (blue arrow). Scan is performed as deemed necessary to check the needle progression. Tip of the introducer cannula in the chest wall,before entering the pleural cavity, correctly alineated with the lesion (yellow arrow), and then reaching the lesion edge (yellow circle), The final scan despite the correct position of the hook-wire into the nodule.
A final CT scan is performed to verify correct positioning,
into the lesion or in a maximum of 10 mm from its border, and to evaluate complications.
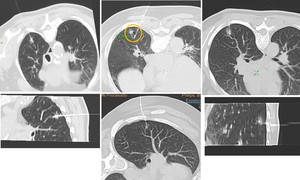
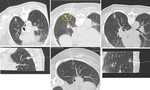
Fig. 7: Differents patterns of correct hook wire emplacement
We use two types of wires: a harpoon shaped wire and an anchor shaped wire.
Both are inserted through a centimeter 20-gauge introducer needle,
10 cm long,
and a 20 cm wire.

Fig. 8: We use wires with an extreme anchor shaped or harpoon shaped.
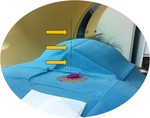
The wire portion extending outside the chest wall is carefully covered with gauze dressings and the patient is immediately transferred to the operating room for thoracoscopic pulmonary wedge resection.
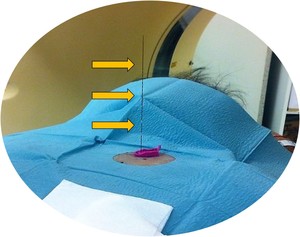
Fig. 9: Wire extending outside the chest wall.
The surgical specimen is sent for frozen-section examination immediatelly with two purposes:
- To determine that the lesion is included.
- In case of benign or metastatic lesions,
the procedure is finalized.
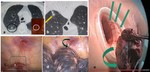
If it seem a primary lung cancer surgery is usually extended to lobectomy and lymphadectomy.
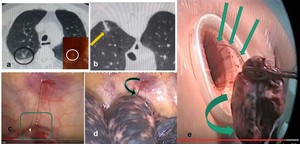
Fig. 10: a) Nodule location. b) Hook wire placement. c),d),e) VATS procedure and tumor extraction with hook wire inside.
COMPLICATIONS
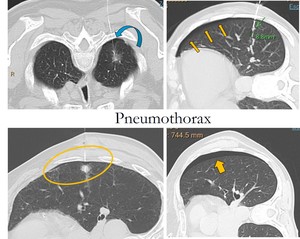
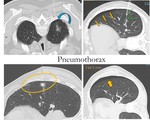
Fig. 11: Pneumothoraces are adjacent to the pleural puncture site and laminar puncture area.
Is the most frecuent complication.
It is considered a minor complication due to the short interval between the procedure and the patient tranfer to the operating room.
Very rarely requieres other than conservative management.
Pleural puncture must be as perpendicular as possible to minimize the risk or pneumothorax.
Pneumothorax appeared in 7 of our patients (23,3%).
Six were minimal and asymptomatic.
One progressive pneumothorax occurred immediately after the hookwire insertion,
leading to wire dislogment.
The air was drained by mean of a 8,5 F pig tail catheter and we intended to place another hook wire,
but it was not possible.
Nevertheless,
lesion could be localized during VATS based on the wire insertion in the thoracic wall.
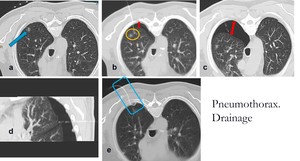
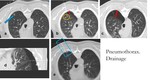
Fig. 12: a) nodule location. b) hook wire placement (nearby the nodule) and small pneumothorax. c/d) growing pneumothorax with hook wire dislodgement to pleural cavity. e) pigtail (placement in CT room) and pneumothorax impprovement.
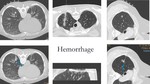
Usually limited to a small oppacity around the lesion or in the wire path.
Eigth patiens (26%) in our study had a small amount of parenchymal bleeding.
Risk increases with longer distance to the pleura.
Minor complication encountered in 4 of our patients (30.8%).
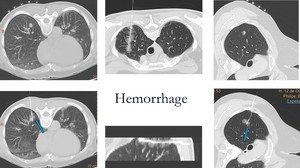
Fig. 13: Mild hemorrhage along the hook-wire traject or around the lesion
It is an unwanted complication that can lead to the loss of intraoperative references.
However,
the small hemorrhage along the needle path and in the pleural surface that is usually present,
help nodule localization even after guide-wire dislogment.
A short length of the wire into the lung parenchyma and a shallow angle between the introducer needle and the pleural surface,
as well as pneumothorax,
are predisposing factors.
After the procedure,
the patient is asked to breathe calmly and any movement during the tranferring to the operating room must be very careful,
as well as traction applied on the wire by the surgeon to tent the lung to facilitate resection.
It happened in 3 of our patients,
1 was the patient with growing pneumothorax during harpoon placement,
1 during the transfer of the patient to the operation room; 1 after pulmonary deflation for VATS.
Nevertheless,
nodule localization was posible,
guided by the pleura puncture site.
There are few cases reported in the literature.
None in our series.
- Other minor complications
Haemoptysis,
chest wall haematoma.
Complications secondary to the surgical procedure are not considered here.