SONOGRAPHIC TECHNIQUE
The uterus,
adnexa and vagina are best imaged with an optimally filled bladder.
Therefore the patients are asked to be well hydrated and not to void in the hour prior to the examination (bearing in mind that overfilling of the bladder can also modify the uterine shape).
In infants and young children who are unable to maintain a full bladder despite adequate fluid ingestion,
it may be necessary to catheterize and fill the bladder with sterile water.
Transabdominal approach is usually adequate for most pelvic US examinations.
When the transabdominal examination is insufficient in sexually active adolescents,
a transvaginal approach can provide more detailed images.
A transperineal approach can complement the evaluation in children with a pelvic mass or a complex congenital anomaly of the genitourinary tract - in this setting,
sterile water can be used as a contrast agent to help in the identification and characterization of the urethra (hydronosonourethrography),
vagina (hydrosonovaginography),
the rectum (water enema),
the urogenital sinus,
or cloaca and additional fluoroscopic genitography / cystourethrography can be added to the US evaluation – if possible,
at the same time using the same catheters - for further adequate evaluation of these structures.
NORMAL ANATOMY
The size and shape of the uterus and ovaries vary according to the age and the hormonal status of the female.
The Uterus
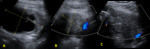
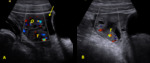
Due to maternal and placental hormones,
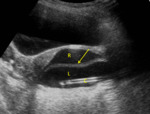
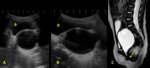
the neonatal uterus is prominent and thickened,
with a brightly echogenic endometrial lining.
The cervix is larger than the fundus (“spade-shaped” uterus with a fundus-to-cervix ratio of 1/2),
the uterine length is approximately 3.5 cm,
and some fluid can also be seen within the endometrial cavity (fig.
1).
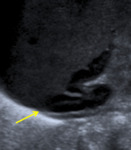
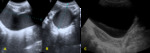
At 2 to 3 months of age the uterus regresses to a smaller size and tubular configuration (with a fundus-to-cervix ratio of 1/1),
with a length of 2.5 to 3 cm,
and with the endometrial lining usually not apparent (fig.
2).
Therefore,
after 2-3 months after birth uterine anomalies can be easily missed due to the small size of the infantile uterus. Around puberty,
with increasing hormone production,
the uterus progressively increases in size and change its morphology.
The postpubertal uterus has the adult pear configuration: the fundus gradually elongates (to 5 to 7cm long) and thickens,
becoming larger than cervix (fundus-to-cervix ratio 3/1).
The echogenicity and thickness of the endometrial lining is seen and undergoes cyclical changes according to the phase of the menstrual cycle.
The Ovaries
The ovaries are not indicative of the postpubertal status,
since they have a similar appearance with visible follicles at all ages.
The difference is mainly in the size of the ovary.
The most reproducible and best described by measurement of the ovarian volume is the ovarian size.
The neonatal ovaries can be found anywhere between the lower pole of the kidneys and the true pelvis due to a typically long pedicle and a small pelvis.
In neonates and girls younger than 6 years,
the mean ovarian volume is 1mL or less.
In premenarchal girls aged 6 to 11 years,
the mean ovarian volume ranges from 1.2 to 2.5mL.
In postmenarchal females,
the ovarian volume averages 9.8mL but it can reach up to 12-15 ml.
STRUCTURAL CONGENITAL ANOMALIES
Müllerian duct anomalies (MDAs) may result from agenesis and/or hypoplasia or abnormalities related to lateral fusion,
vertical fusion,
a combination of both.
The most commonly used classification is the one by the American Society for Reproductive Medicine.
A) Müllerian aplasia: is the congenital absence/atresia of the upper 2/3 of the vagina in association with an absent or rudimentary uterus and normal ovaries.
Renal and skeletal anomalies often coexist.
US confirms the presence of normal ovaries and helps to characterize any müllerian tissue,
and to assure renal presence,
their position,
and morphology.
B) Failure of resorption of the median uterine septum
- Septate uterus: is the most common MDA.
The external surface of the uterus has either a normal configuration or a flat,
broad fundus,
and there are two endometrial cavities.
The septum can be partial or complete,
in which case it extends to the internal cervical os.
There is usually a single cervix.
C) Failure of lateral fusion müllerian ducts:
- Unicornuate uterus: occurs when there is agenesis of one müllerian duct,
resulting in a single horned uterus (“banana-shaped”) with a single round ligament and fallopian tube.
In the majority of cases,
the arrest is incomplete and a contralateral rudimentary horn with or without functioning endometrium is present.
US may demonstrate two uterine horns of different sizes.
The most commonly associated renal anomaly is renal agenesis ipsitlateral to the side of the absent/rudimentary horn.
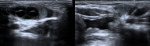
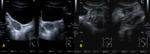
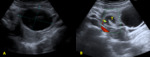
- Didelphys uterus: occurs due to complete nonfusion of both müllerian ducts,
resulting in a duplicated uterus and cervix.
The individual horns are fully developed and almost normal in size.
A vaginal septum may coexist.
The most commonly associated renal anomaly is renal agenesis homolateral to the obstructed horn and the obstructed hemivagina (fig.
3).
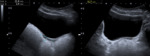
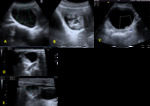
- Bicornuate uterus: results from partial nonfusion of the müllerian ducts.
The external surface is deeply indented,
and the central myometrium may extend to the level of the internal cervical os (bicornuate unicollis – fig.
4) or external cervical os (bicornuate bicollis).
In patients with MDAs,
the kidneys should always be evaluated because renal anomalies occur in increased frequency in these patients.
The most common renal anomalies are absent,
multicystic dysplastic kidney or ectopic kidney and the most common type of MDAs to have associated renal anomalies are uterus didelphys and unicornuate uterus.
In any newborn with those kidney abnormalities,
early postnatal ultrasound should always include the evaluation of the genital inner organs.
Uterine abnormalities can often be depicted in the physiologic prominent neonatal uterus,
whereas after 2-3 months of age uterine anomalies can be easily missed in the small infantile uterus.
CONTRIBUTION OF US IN AMBIGUOUS GENITALIA
In newborns with ambiguous genitalia,
US is used to determine the presence/absence of a uterus,
the location and characterization of the gonads (typical ovary/typical testicle/undefined gonad - bearing in mind that dysplastic gonadal tissue carries a high risk of malignant tumor,
particularly gonadoblastoma),
and to assess the adrenal glands for diffuse enlargement or masses.
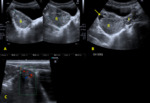
US genitography and/or fluoroscopic genitography (potentially followed by cystourethrography) after saline/contrast material retrograde filling through the urogenital orifice will allow further adequate characterization of the urethra,
vagina (fig.5),
urogenital sinus and cloaca.
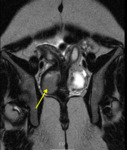
Most cases ambiguous genitalia consist of 46,XX due to congenital adrenal hyperplasia (fig.
6).
In these patients,
the adrenal glands are enlarged,
and there is masculinization of the lower urogenital tract.
US shows a normal uterus and ovaries.
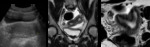
In the rarer cases of ovotesticular DSD (former named true hemaphroditism),
the patient has both ovarian and testicular tissue,
in the form of either separate structures or an ovotestis (fig.
7).
Turner syndrome is the most common form of gonadal dysgenesis and the most common cause of sex chromosome disorders of sex development (DSD). US shows a juvenile appearance of the uterus and absent or streaky ovaries (fig.
8).
US ASSESSMENT OF HORMONAL STATUS
Estrogen stimulation is indicated by increased thickness and volume of the uterus; swelling of the fundus; and the presence of a prominent echogenic endometrium.
The appearance of the ovaries is less useful because of the normal visibility of follicles at all ages.
PRIMARY AMENORRHEA
Causes: gonadal dysgenesis; hypothalamic-pituitary causes; müllerian anomalies; and other disorders (PCOS; congenital adrenal hyperplasia; androgen insensitivity).
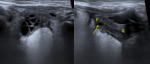
Hydrocolpos or hydrometrocolpos
Obstrution of the genital tract results in accumulation of secretions (hydro) and blood (hemato) in the uterus (metro) and/or vagina (colpos),
with the location depending on the degree and level of the obstruction.
Most cases of hydrocolpos or hydrometrocolpos (fig.
9) in the neonate are associated with a urogenital or cloacal malformation,
with the most common congenital anomalies being an imperforate hymen,
a transverse vaginal septum or a stenotic or atretic vagina. In adolescence,
patients may present with amenorrhea,
cyclic abdominal pain and hemato(metro)colpos (fig.
10 ).
In the case of vaginal septum,
there is often a small central or eccentric perforation and patients may present with pyohematocolpos due to ascending infection that occurs through the small perforation.
Sonographycally,
one can see fluid distention of a short or blind-ending vagina and a lesser degree of uterine distension.
Echogenic debris within the fluid is due to mucous secretions in neonates and blood in postmenarcheal girls.
In the case of a vaginal septum,
it can be identified as a septation less than 1 cm in thickness and extending completely or incompletely across the vagina.
Hematometrocolpos can also occur in the absence of amenorrohea,
if a duplicated uterovaginal anomaly with unilateral obstruction occurs.
Transperineal US is useful in documenting absence of the distal vagina and measuring the distance between the proximal vagina and the perineal surface.
Polycystic Ovarian Disease (PCOS)
PCOS is a syndrome of ovarian dysfunction and is the most common endocrinopathy in premenopausal women.
The primary clinical features appear late in puberty and are due to hyperandrogenism and ovarian dysfunction.
In 2003,
the Rotterdam PCOS consensus group defined PCOS as:
- oligo-anovulation and/or polycystic ovaries; and
- clinical and/or biochemical signs of hyperandrogenism and
- exclusion of other androgen excess or related disorders (congenital adrenal hyperplasias,
androgen-secreting tumours,
Cushing's syndrome).
The changes in the ovaries are termed “polycystic ovarian morphology” and the sonographic features have been recently redefined in a task force report from the Androgen Excess and PCOS Society released in 2014:
- 25 or more follicles per ovary
- increased ovarian size (>10 cc) (although less sensitive than the follicle number criteria,
can by routinely used when image resolution does not allow accurate follicle count (e.g.
transabdominal scanning,
older equipment)
Since most adolescent girls will undergo transabdominal US and not transvaginal US,
volume measurements are generally used as the main diagnostic criterion.
Additional sonographic features of polycystic ovaries include round shape and increased stromal ecogenicity,
with the follicles usually located peripherally (“string of pearls”),
although they can occur randomly throughout the parenchyma (fig.
11).
Long-term follow-up is of value in these patients because of the increased incidence on endometrial carcinoma.
PREPUBERTAL BLEEDING
Precocious Puberty
Is the complete sexual development (including secondary sexual characteristics,
gonadal enlargement and ovulation) before 8 years of age.
It is classified into two types: central (gonadotropin dependent) and peripheral (gonatotropin independent).
Pelvic US is used to assess ovarian size and morphology and to confirm or exclude a postpubertal appearance of the internal genitalia,
to diagnose an estrogen-secreting adrenal or ovarian tumor and to monitor the effect of medical or surgical treatment.
Sonographic examination of the liver should always be included because precocious puberty has been associated with hepatoblastoma.
In isolated premature adrenarche (of pubic and axillary hair development) and isolated premature thelarche (breast development),
US shows normal prepubertal uterus and ovaries.
Ultrasonographic investigation of prepubertal bleeding should also include exclusion of:
A) Vaginal foreign body: in children,
toilet paper is the most common vaginal foreign body in the vagina;US can identify both radiopaque and nonradiopaque objects as echogenic material with distal acoustic shadowing (which is characteristic but not always present).
B) Vaginal Masses: in the pediatric population,
although rare,
malignant tumors are more common that benign tumors and the vagina is a more common site than is the uterus.
- Vaginal rhabdomyosarcoma: is the most common primary malignant neoplasm; it usually presents at 6 to 18 months of age with vaginal bleeding or as a protruding polypoid cluster of masses (botryoides) through the introitus,
usually arising from the anterior wall of the vagina near the cervix.
At US,
a vaginal rhabdomyosarcoma appears as a large,
solid,
heterogeneous or homogeneous mass that fill the vaginal cavity.
PELVIC PAIN
Gynecological causes of pelvic pain include adnexal torsion,
ruptured or hemorrhagic ovarian cyst,
pelvic inflammatory disease and ectopic pregnancy. Differential diagnosis with non-gynecological causes of acute lower abdominal pain include acute appendicitis,
Meckel’s diverticulitis,
exacerbation of inflammatory bowel disease,
among others.
Adnexal Torsion
Adnexal (ovarian and/or tubal) torsion results from partial or complete rotation of the ovary,
the fallopian tube,
or both structures,
on its vascular pedicle,
compromising venous and lymphatic drainage and with resulting ovarian edema and adnexal enlargement.
If complete and unalleviated,
the increased pressure on the ovary can cause arterial occlusion and ultimately ischemia and infarction ensue.
Therefore,
pathologic findings range from massive edema to parenchymal necrosis.
Torsion can be partial or complete,
and acute or chronic.
Intermittent torsion is not uncommon,
with periods of spontaneous remission of the symptoms.
The peak incidence occurs in adolescence and young adulthood.
Torsion is nearly always unilateral and most frequently right-sided,
and although most cases of ovarian torsion are associated with an ovarian cyst or tumor,
torsion of normal adnexa can occur (usually in prepubertal girls) and it is thought to be related to excessive mobility of the adnexa.
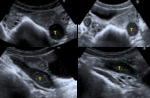
The sonographic findings in acute ovarian torsion are often nonspecific and include (fig.
12; fig.
13):
- Ovarian enlargement (the most constant finding)
- Diameter >5cm or 2,3 times larger than the contralateral ovary
- Volume >75mL or 12 times more than the contralateral ovary
- Peripheral placed follicles
- With or without fluid-debris level
- Associated adnexal cyst or mass (the most common tumor predisposed for ovarian torsion is the benign mature cystic teratoma)
- Heterogeneous internal texture
- Hemorrhagic or necrotic areas
- Abnormal position
- Medial and superior to the uterus
- Abnormal or absent blood flow
Other associated findings include: twisted vascular pedicle with “whirlpool sign” on color Doppler,
hydrosalpinx (if the fallopian tube is involved),
hyperecogeneous adjacent fat tissue and fluid in cul-de-sac.
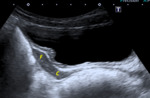
Isolated fallopian tube torsion is a rare event and should be suspected when a cystic mass in a midline position (in the cul-de-sac or superior to the uterus) is demonstrated in association with a normal ipsilateral ovary (fig.
14).
Hemorrhagic Ovarian Cyst
Acute onset of pelvic pain contemporary with the midcycle is clinically suggestive of hemorrhage within a functional ovarian cyst (usually a corpus luteum cyst).
Hemorrhagic ovarian cysts are called “the great imitator” owing to their variety of sonographic appearances depending on the age and the amount of the blood (fig.
15):
- Acute hemorrhagic cyst is usually hyperecoic and homogeneous with posterior acoustic enhancement
- As the clot lysis,
an interior fine reticular pattern is demonstrated,
the so called fishnet appearance,
representing residual fibrin strands - this is the most typical finding
- The retracting blood clot may also be seen as an echogenic focus within an anechoic structure,
with a concave outer margin.
- Color Doppler US will show no flow within the clot but only in the peripheral cyst wall.
Other associated findings include: thick wall,
septations,
fluid-fluid or fluid-debris level within the cyst and ecogenic free fluid in the cul-de-sac.
Follow-up US is performed in 4-6 weeks to ensure regression (the cyst again becomes predominantly anechoic).
Pelvic Inflammatory Disease
Pelvic inflammatory disease affects sexually active girls and is usually due to an ascending sexually transmitted infection (Neisseria gonorrhoeae or Chlamydia trachomatis).
Less common causes include direct extension from appendiceal,
diverticular or postsurgical abscesses that have ruptured into the pelvis.
Sonographic findings depend on the stage of the inflammatory process:
- Acutely,
findings are minimal,
if any imaging abnormalities are detectable;
- Endometritis: it is usually difficult to appreciate; the uterus may be enlarged and more hyperecoic and may have indistinct margins; endometrial thickening or fluid may be present;
- Pyosalpinx appears as dilated,
occluded fallopian tube with thick wall and low-level echoes in its interior due to the presence of purulent debris (fig.
17); anechoic fluid within the tube indicates hydrosalpinx;
- With the progression of the disease,
periovarian adhesions may form and cause fusion of the ovary and fallopian tube,
resulting in a tubo-ovarian complex; further progression leads to total breakdown of tubal and ovarian architecture,
forming a tubo-ovarian abscess,
which appears as a heterogeneous,
multiloculated,
adnexal mass with enhanced through transmission,
internal septations,
irregular margins and low-level internal echoes.