Keywords:
Oncology, Interventional non-vascular, Liver, Catheter arteriography, Percutaneous, CT, Chemoembolisation, Chemotherapy, Treatment effects, Cancer
Authors:
F. Carchesio, R. Iezzi, A. Posa, M. Pompili, A. Gasbarrini, R. Manfredi; Rome/IT
DOI:
10.1594/ecr2018/C-3001
Results
A total of 86 treatments were performed.
Technical success,
defined as the ability to deliver the total planned dose or to obtain stop flow,
was achieved in all patients.
No intra- or peri-procedural complications occurred and in particular no signs of liver failure or systemic toxicity were detected.
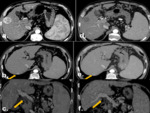
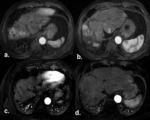
At 1-month follow-up,
an objective response rate (ORR) of 45.9% and overall disease control (ODC) of 79.2% were observed.
In nine patients with ODC and residual viable tumor higher than 50%,
a repeated DSM-TACE treatment was performed.
During the mean follow-up of 18.2 months an ODC of 45.8% was registered.
PFS,
calculated using the Kaplan-Meier method,
was 5.8 months with a median OS of 10.8 months (Fig.
1; Fig.2).
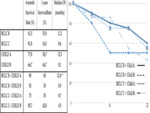
When considering the subgroup evaluation (Fig.3),
significant longer overall survival was obtained for BCLC-B intermediate Child-Pugh A patients compared with BCLC-C advanced Child-Pugh B patients.
The outcome justifies the prognostic pivotal role of liver functional reserve in intermediate/advanced HCC patients with liver cirrhosis which has been previously described by other groups.