We have gathered special cases from our institution to illustrate the spectrum of the main primary and secondary histiocytic disorders affecting the lungs,
reviewing these diseases and their natural history,
with emphasis on the radiological findings.
Malignant conditions will not be addressed in this study.
1.
Primary Histiocytosis
1.1 Langerhans Cell Histiocytosis
Langerhans cell histiocytosis (LCH) is the most common disorder in the dendritic cell group.
However,
it is still a rare disease and it is characterized by proliferation and infiltration of Langerhans cells in one or more organs,
such as flat or long bones,
liver,
lymph nodes,
central nervous system and lungs.
There are three known presentations of LCH,
divided accordingly to the number of lesions and systems involved,
each with its own particular prognosis.
The unifocal type (70% of cases) presents between 5 and 15 years of age,
in a single or a few bones,
and may sometimes involve the lungs.
The multifocal unisystem (20% of cases) presents in children 1 - 5 years old,
involving multiple bones and the reticuloendothelial system,
sometimes presenting with diabetes insipidus,
when there is pituitary involvement.
The multifocal multisystem form (10% of cases) presents in the first 2 years of life and is also known as the fulminant type,
being often fatal.
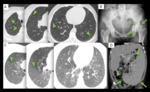
Some examples of systemic findings are shown in the images below.
Pulmonary Langerhans cell histiocytosis (PLCH) occurs only in approximately 10% of LCH cases and can present as the only affected organ or as part of a systemic disease.
It has no predilection for sex and can affect individuals of any age,
but almost exclusively affects young adults.
Patients with PLCH are at higher-risk for malignancies,
such as lymphoma and bronchogenic carcinoma,
probably due to their dysfunctional immune system and the fact that this condition is almost always associated with smoking.
The prognosis is overall good,
with smoking cessation being imperative for such an outcome.
Patients can be asymptomatic or have systemic manifestations along with the pulmonary symptoms.
In the pediatric population,
the pulmonary involvement is rare and is usually part of a multifocal multisystem disease,
that is more aggressive and often fatal.
Histologically,
PLCH findings can be summarized as cellular lesions in the early-stage and,
as the disease progresses,
fibrotic lesions and cysts become dominant.
In the beginning,
the proliferation of Langerhans cells is in the bronchiolar and bronchial epithelium,
forming granulomas that appear as centrilobular micronodules.
Cysts are formed through cavitating nodules or as a result of traction on the central bronchiole with destruction of bronchiolar walls by peripheral fibrosis.
Non-enhanced computed tomography (NECT) is the best method to diagnose PLCH even though it has variable appearance depending on the stage of disease,
ranging from small peribronchiolar nodular opacities to multiple irregularly-shaped cysts.
Nodules are the main findings at the early stage of the disease.
They can vary in size,
measuring usually less than 10 mm,
ranging from a few to numerous,
with irregular margins and centrilobular distribution.
The cysts are more pronounced later in the disease,
can measure up to 20-30 mm but are usually less than 10 mm,
with mostly thin walls that can also be a few millimeters thick.
The involvement of the lungs tend to be bilateral,
symmetric,
with an upper and mid lung distribution.
Overall,
the prognosis is good,
being smoking cessation imperative.
In persistent or progressive cases,
chemotherapy and steroids may be necessary for treatment.
As a general rule,
the higher the number of lesions and systems involved,
the younger the patients and the worst the outcomes.
1.2 Non-Langerhans Cell Histiocytosis:
Rosai-Dorfman
Rosai-Dorfman disease (RDD),
also known as sinus histiocytosis with massive lymphadenopathy, is a rare non-neoplastic histiocytic disorder characterized by macrophage proliferation.
Some immune regulation disorders and viral infections are thought to be involved.
This condition has a slight male predominance,
with predilection for children and young adults,
most common in people from African and west Indian descent.
It has a good prognosis even when no treatment is administered. Surgical resection can be useful if there is vital organ involvement or complications.
Extranodal lesions,
associated with worse prognosis,
are present in nearly half of the patients and frequently occur in the head and neck.
More rarely,
it can also affect other organs such as the CNS,
breasts,
lungs,
gastrointestinal,
bones and subcutaneous tissue.
Therefore,
if diagnosed in one site,
screening and follow-up in other body parts are mandatory.
Epidural or subdural lesions are the main CNS manifestations and can be confused with meningiomas at imaging.
These patients aren’t usually associated with lymphadenopathy.
Bone involvement is more common in the skull,
tibia and femur and typically presents as multicentric lytic lesions with variable presence of sclerotic margins and can be easily confused with LCH lesions.
Thoracic RDD is very rare and involves the trachea,
bronchi and associated lymph nodes and,
less commonly,
may manifest as a lung nodule or interstitial involvement.
CT findings include solitary or multiple polypoid masses in the airways.
Pleural involvement is associated with extensive lung disease but can be an isolated thoracic finding.
Erdheim-Chester
Erdheim-Chester disease (ECD) is a rare non-LCH dendritic cell disorder that affects middle-aged and older adults,
with a slight male predominance.
It is considered to be non-genetic and not associated with infectious agents.
Presentation of ECD may vary from an indolent focal disease to a life-threatening organ failure and the diagnosis is based on histological and radiological findings.
Bone involvement is practically universal in ECD,
leading to diagnosis as patients tend to present bone pain as a first complaint.
It is usually seen in long bones as bilateral and symmetrical osteosclerosis.
Almost half of the patients have extraskeletal manifestations upon diagnosis,
which are associated with a worse prognosis.
The possible sites of involvement include retroperitoneum,
kidney,
CNS,
orbit,
skin,
breast,
sinonasal mucosa and skeletal muscle.
The treatment has limited alternatives and interferon therapy serves as the first-line choice.
Surgical percutaneous intervention is an option for symptomatic local disease and helps alleviate mass effect on vital structures.
The most common causes of death are pulmonary fibrosis and cardiac failure.
The spectrum of CECT findings of the chest in patients with ECD is rather vast and includes smooth pleural and septal thickening,
effusions,
ground-glass opacities,
consolidations,
centrilobular micronodular opacities and thin-walled cysts. Cardiovascular structures such as the pericardium,
the cardiac muscles and the great vessels (coated aorta) can also be infiltrated.
Sclerosis of the ribs,
clavicles,
sternum,
and spine can also be detected.
Renal encasement by homogeneous soft tissue can be partially seen when the chest CT reaches the upper abdomen.
Hemophagocytic Lymphohistiocitosis Syndrome
Hemophagocytic lymphohistiocytosis (HLH) is a nonmalignant rare multisystem disorder of immune regulation,
characterized by excess of lymphocytes and activated macrophages,
typically with hemophagocytosis,
in the bone marrow,
spleen,
liver,
and lymph nodes.
It has a poor outcome and,
if left untreated,
can be fatal.
HLH can be primary (with an autosomal recessive inheritance pattern,
seen in young children) or secondary, associated with infections (such as EBV,
CMV,
leishmaniasis),
autoimmune conditions or prolonged immunosuppression,
usually occurring in older infants and adults.
The diagnosis is often delayed because of its non-specific symptoms and requires the presence of a specific set of diagnostic criteria.
CNS involvement mimics encephalitis and is quite frequent,
with a poor prognosis.
Abdominal abnormalities can include organomegaly (liver,
spleen and/or kidney),
ascites,
lymphadenopathy and periportal echogenicity.
Regarding the chest,
alveolar-interstitial opacities with or without pleural effusion may be seen in radiographs,
often with rapid evolution.
2.
Secondary Histiocytosis
2.1 Histiocytic reaction as a major component - Storage diseases
Gaucher Disease
Gaucher disease (GD) is the most common lysosomal storage disease,
usually diagnosed during childhood,
with no predilection for gender.
It is an autosomal recessive,
multisystem disorder caused by deficiency of glucocerebrosidase or beta-glucosidase activity,
resulting in accumulation of a glycolipid (glucocerebroside) within the lysosomes of macrophages (Gaucher cells),
particularly in the bone marrow,
liver and spleen.
There are three clinical subtypes based on the presence (type 2 and 3) or absence (type 1) of neurologic manifestations.
Clinical manifestations can be severe,
and lead to death from hepatic,
pulmonary or cardiac failure.
The accumulation of Gaucher cells leads to organomegaly and hematologic dysfunction.
Skeletal infiltration results in abnormal bone remodeling with vertebral endplate collapse (seen as "ballooning" of intervertebral disc) and femoral Erlenmeyer flask deformity; it can also manifest simply as osteopenia,
osteonecrosis or fractures.
Extraosseous deposits of Gaucher cells are a rare complication of GD and should be considered when patients with known Gaucher disease present with soft tissue masses.
Exclusion of malignancy is mandatory since these patients are at increased risk for such complications.
Liver disease can amount to hepatopulmonary syndrome (dilated lung capillaries,
arteriovenous shunting,
and hypoxemia),
associated with a worse prognosis.
Lung involvement is uncommon and is usually present only in severe systemic disease.
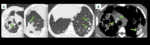
Infiltration of alveoli and alveolar walls are the main involvement and appear on CT as interlobular septal thickening and ground-glass opacity.
If occluded, the alveolar septal capillaries can lead to pulmonary hypertension.
Alveolar filling by these typical cells can mimic desquamative interstitial pneumonia (DIP).
Niemann-Pick Disease
Niemann-Pick Disease (NPD) is an autosomal recessive lysosomal storage disease with three subtypes.
Types A and B are caused by absence or deficiency of acid sphingomyelinase enzyme,
with pathologic accumulation of sphingomyelin and other lipids in macrophages (Niemann-Pick cells).
Both types present with hepatosplenomegaly and CNS involvement.
Type A has an earlier onset and worse prognosis whereas type B is associated with survival into adulthood and a variable age of onset and prognosis.
Type C is due to mutations in cholesterol-binding genes affecting intracellular cholesterol metabolism,
with pronounced CNS involvement but mild hepatosplenomegaly.
Pulmonary involvement occurs in all three types but is more frequent in type B.
The alveolar filling by Niemann-Pick cells causes a type of endogenous lipoid pneumonia,
which also infiltrates the interstitium,
preserving the lung's architecture.
CT findings include ground-glass opacities,
occasionally with interlobular septal thickening and / or crazy-paving pattern.
Fabry Disease
Fabry Disease (FD) is a multisystem lysosomal storage disorder that results from a X-linked inborn error of metabolism.
It's caused by α-galactosidase A deficiency,
resulting in abnormal accumulation of globotriaosylceramide in various organ systems. Endothelial accumulation of glycosphingolipids compromises vessel lumen size,
leading to vascular events.
Without treatment,
the condition is fatal in men within 50 years.
Heterozygous women,
even as carriers,
may also exhibit similar symptoms.
Lung-related symptoms include chronic obstructive airway disease,
such as dyspnea,
airway obstruction,
wheezing,
pneumothorax,
and hemoptysis.
CT findings include ground-glass opacities,
reflecting alveolar filling,
and mosaic attenuation,
indicating small-airway disease.
Cardiac involvement in FD is common and is the most frequent cause of death.
2.2 Histiocytic reaction as a minor component:
Pneumoconiosis
Pneumoconiosis are occupational lung diseases caused by inhalation of dust particles,
causing a of tissue reaction in the lungs.
These conditions may be clinically and pathologically classified as fibrotic or nonfibrotic,
being silicosis,
coal worker pneumoconiosis,
and asbestosis the three most common types.
The diagnosis of pneumoconiosis should be made by integrating a history of occupational exposure to inorganic dusts with certain imaging findings.
The pneumoconiosis associated with histiocytic disorders are silicosis,
anthracosis and hard-metal (especially cobalt) exposure.
Silicosis occurs in two clinical forms that are divided accordingly to the time of exposure to silica.
Acute silicosis manifests as alveolar silicoproteinosis and classic silicosis manifests as a chronic interstitial reticulonodular disease.
Histopathologically,
acute silicosis shows severe alveolitis with alveolar lipoproteinosis whereas the classic presents with silicotic nodules composed of mature collagen in the central portion and particle-laden macrophages in the peripheral zone.
Interstitial diseases
Respiratory bronchiolitis-associated interstitial lung disease (RB-ILD) is a rare smoking related disease that is closely associated to respiratory bronchiolitis (RB) but with more severe histologic,
imaging,
and clinical features.
This disorder is characterized by the accumulation of yellow-brown pigmented macrophages in airways and alveoli,
cellular or fibrotic inflammation with associated clinical features of interstitial infiltration.
Unlike simple RB,
mild to moderate chronic inflammation and fibrosis extend beyond the tissues immediately adjacent to respiratory bronchioles and into alveolar septa,
leading to architectural distortion,
as well as centrilobular emphysema (a RB-ILD progression to emphysema remains controversial).
Some patients have a good response to smoking cessation and/or corticosteroids,
but often the disease progresses despite any treatment.
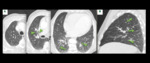
The main CT findings are central and peripheral bronchial wall thickening,
centrilobular micronodules (typically ground-glass attenuation but may be solid) and ground-glass opacities.
Both upper and lower zones are potentially affected,
with a modest upper zone predilection.
If advanced,
fibrosis may be evident affecting the subpleural regions.
The tree-in-bud pattern is a common manifestation of small-airway-disease but is rarely present in RB-ILD.
Patchy areas of hypoattenuation can be seen and have a slight lower lung predominance.
Desquamative interstitial pneumonia (DIP) is thought to represent the end-stage of RB-ILD and,
thus,
shares very similar CT findings with the latter. This disorder,
however,
has more pronounced alveoli pigment-laden macrophages than RB-ILD and can have other predisposing factors,
such as autoimmune disorders and infections,
which account for almost 10% of causes.
As previously mentioned,
interstitial infiltrates and ground-glass opacities are still the main findings,
though in a more diffuse distribution (less peribronchiolar),
notably basal and peripheral.

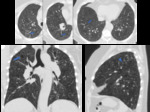
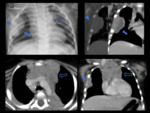
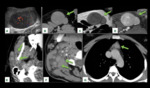
![Fig. 3: 9-month-old boy with Hemophagocytic lymphohistiocytosis. PA radiograph (A) and a lung windowing of an axial CT image (B) of the chest show interstitial opacities (arrows) in the lungs. A widened mediastinum is also noted on both A and B images, but better seen in the axial CT image with soft parts windowing (C). There are multiple enlarged lymph nodes (arrowheads) in the hilar regions and axillae. Erdheim-Chester disease manifestations in a 73-year-old man with chest CT showing wall infiltration of the thoracic aorta (coated aorta) seen in the sagital soft tissue windowiing image (D) and bilateral smooth thickening of the interlobular septa in the apices, seen in the axial lung windowing image (E) [These images are courtesy of Dr. Célia Antunes and were published on Insights Imaging (2014) 5:473–482]. The last image (F) is an axial chest CT with soft parts windowing showing a lymphadenopathy in the anterior mediastinum of a 25-year-old woman with Rosai-Dorfman disease.](https://epos.myesr.org/posterimage/esr/ecr2018/144239/media/775350?maxheight=150&maxwidth=150)