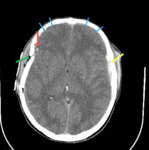
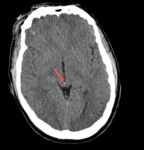
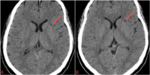
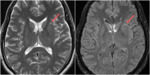
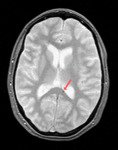
On neuroimaging,
axonal injury is seen as small focal white-matter lesions measuring from 1 to 15 mm in size (Fig.1,
Fig.2,
Fig.3).
Traumatic microbleeds are considered to be important imaging marker for DAI. They are seen as punctate lesions at corticomedullary junction,
corpus callosum,
deep grey matter and brainstem.
DAI is much more visible through MR (magnetic resonance) than CT (computed tomography).
It is estimated that 50-80% of DAI patients have normal CT scan reading upon presentation.
Therefore,
brain magnetic resonance is the best imaging tool for DAI.
CT
Since the diagnosis of DAI in acute patient who suffered a significant head trauma is difficult to obtain clinically,
using CT in the emergency settings is helpful in the identification of injuries and diagnosis.
Initial CT scan can show no abnormalities or it can be positive for DAI and show small petechial hemorrhages located at the grey-white matter junction as well as in the corpus callosum and brainstem (Fig.1,
Fig.2,
Fig.3).
Delayed brain CT usually demonstrates edema,
which is a later finding associated with DAI (Fig.4).
CT is particularly insensitive to non-hemorrhagic lesions which are rarely detected on CT scans (Fig.5,
Fig.6).
The larger and more hemorrhagic the lesion is,
the easier it is to notice on the CT scan.
Possible findings and lesion characteristics on non-contrasted brain CT in DAI are:
- Often normal (50-80%)
- Hemorrhagic lesions are hyperdense
- Non-hemorrhagic lesions are hypodense
- The lesions typically become more evident over the first few days as edema develops around them
Although MR is more sensitive in the detection of subtle soft-tissue abnormalities,
CT scanning is more available,
and is therefore,
usually performed as a primary,
emergency neuroimaging tool in head trauma patients.
Short examination time and its compatibility with life-supporting devices have made it a method of choice to evaluate head trauma patients.
MR
Even though MR requires a longer image acquisition time and is not compatible with instruments having magnetic components,
its ability to show small abnormalities in brain parenchyma has made it the best imaging tool for DAI.
It is useful for assessing suspected diffuse axonal injury even in patients with entirely normal CT of the brain.
Possible findings and lesion characteristics on brain MR are:
- Microbleeds
- Punctate lesions at corticomedullary junction,
corpus callosum,
deep gray matter, brainstem
- Size of lesions: up to 15 mm
- Morphology of lesions: punctate,
round,
ovoid foci; often hemorrhagic,
nearly always multiple and bilateral
Most common location of lesions is gray-white matter interface (67%),
especially frontotemporal lobes,
corpus callosum (20%) with common involvement of splenium and posterior body,
brainstem,
especially dorsolateral midbrain and upper pons.
Involvement of corpus callosum,
and particularly of the brain stem is related to poorer outcome.
Less common locations of lesions are deep grey matter,
internal/external capsule,
tegmentum,
fornix,
corona radiata and cerebellar peduncles.
Useful MR sequences for nonhemorrhagic lesions are FLAIR (fluid-attenuated inversion recovery) and DWI (diffusion-weighted images),
and for hemorrhagic lesions SWI (susceptibility-weighted imaging) or T2* GRE (gradient echo).
Nonhemorrhagic DAI lesions appear as small foci of increased signal on T2- weighted images (T2WI) and FLAIR within the white matter (Fig.6).
On T1-weighted images (T1WI) they appear as subtle areas of decreased intensity.
The lesions tend to be multiple and bilateral,
especially in patients with severe head injury.
Hemorrhagic lesions are best seen on SWI and T2* GRE imaging.
On these sequences they appear as hypointense focal lesions as a result of susceptibility from blood products (Fig.7). Hemorrhagic lesions appear hyperintense on T1WI.
The abnormal signal on gradient-echo images can persist for many years after the injury.
That abnormal,
low signal,
represents hemosiderin-laden macrophages that occur adjacent to small vessels and are indicative of previous extravasation of blood.
Sometimes DAI lesions can show restricted diffusion with high signal intensity on DWI sequences and hypointense signal intensity on ADC map.
Cytotoxic edema may be a cause of those findings,
but it is believed there are other possible mechanism and causes which are contributing to increased restricted diffusion in DAI
The neuroimaging can also play a significant role in determining the outcome of patients after DAI.
Some studies show that the greater the number of lesions observed early after trauma,
the greater the impairment of functionality after 12 months.
Besides the number of lesions,
the location of lesions is also a very important factor which is related to severity of patient`s symptoms and severity of trauma.
Patients with the mildest forms of injury have lesions in frontal and temporal white matter,
near the gray–white junction.
The lesions typically involve the parasagittal regions of the frontal lobes and periventricular regions of the temporal lobes.
Patients with more severe trauma have DAI in deeper white matter as well as in the corpus callosum,
especially the posterior body and splenium.
Patients with brain stem injuries have poor outcome,
sometimes leading to death.