Type:
Educational Exhibit
Keywords:
Neoplasia, Inflammation, Infection, Education, Ultrasound, MR, CT, Soft tissues / Skin, Paediatric, Neuroradiology brain
Authors:
A. Chattopadhyay, D. J. Warren, I. Craven, M. S. Igra; Leeds/UK
DOI:
10.1594/ecr2018/C-3191
Findings and procedure details
The characteristic imaging features of a wide range of scalp and skull lesions are illustrated across a range of imaging modalities.
Parietal Foramina
Background:
- Congenital calvarial defects which are a result of delayed/incomplete ossification of the parietal bones,
specifically around the parietal notch
- Typically,
they appear as a pair of lucencies within the parietal bone,
close to the intersection of the sagittal and lambdoid sutures.
- Occasionally,
there can be associated meningeal,
cortical or vascular malformations which can act as an epileptogenic focus.
Imaging:
- US- defects within the parietal bone.
-
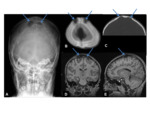
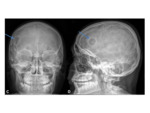
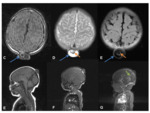
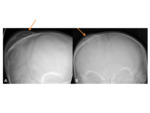
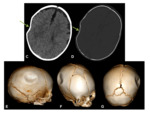
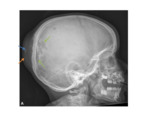
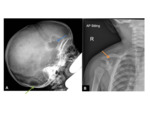
XR and CT- symmetrical radiolucencies either side of the sagittal suture- best appreciated on frontal views.
Radiographic appearances are often likened to a “pair of spectacles”.
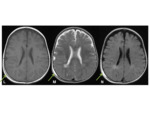
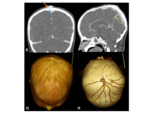
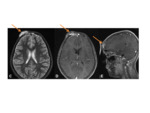
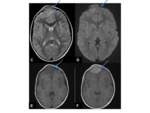
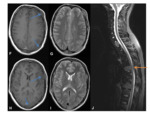
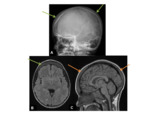
Fig. 1 Occasionally,
the defects may join,
and appear as a single midline lucency.
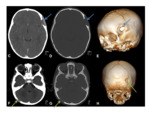
CT can provide useful 3D reformats.
Fig. 1
-
MR- bony defects as above.
MRI provides superior soft-tissue delineation compared to CT,
and will identify any associated cortical,
vascular or meningeal anomalies Fig. 1
Dermoid Cyst
Background:
-
Benign lesions,
thought to arise from inclusion of ectodermal components at sites of suture and neural tube closure.
Common locations are along the planes of embryonic closure- the anterior fontanelle Fig. 2 ,
glabella Fig. 3 Fig. 4 ,
nasion,
vertex and occiput,
as well as along the coronal and lambdoid sutures Fig. 5 Fig. 6 Fig. 7 .
-
Histologically,
they are lined by squamous epithelium,
and contain dermal elements,
such as hair,
sebaceous and sweat glands,
keratin,
smooth muscle and lipid debris.
- Can be associated with bony invasion,
sinus tracts and intracranial extension.
-
Treatment is with surgical removal or curettage.
Resection is indicated to prevent further growth and minimise potential infection risks,
as well as for cosmetic reasons.
Imaging:
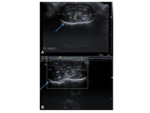
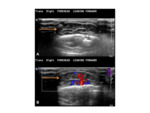
- US- encapsulated,
unilocular cystic lesion which appear heterogeneous,
with internal echoes.
Fig. 5
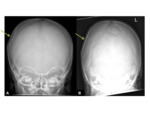
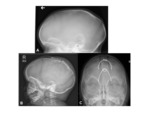
- XR- well-demarcated,
lytic lesion,
with sclerotic borders.
Fig. 6
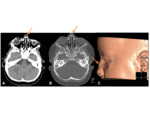
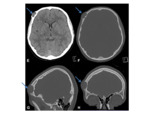
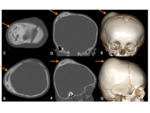
- CT- expansile,
osteolytic midline lesions,
with a sclerotic border. The soft-tissue component extends beyond the confines of the cranium.
Fig. 7 Most dermoid cysts have the attenuation and signal intensity of lipid material due to sebaceous contents.
Unlike epidermoid cysts,
dermoids can have a thick wall that enhances following contrast.
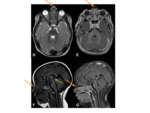
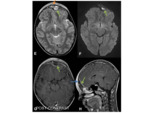
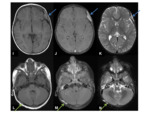
- MR- superior to CT in assessing for potential intracranial extension. The lesions tend to be T1- iso-hypodense,
T2-iso-hyperdense and can show rim enhancement following gadolinium.
Fig. 4
Encephalocele
Background:
-
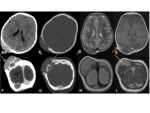
Extracranial herniation of intracranial structures through a bony defect.
Fig. 8
-
Often associated with other intracranial pathologies or congenital abnormalities.
-
Surgery is the gold-standard treatment.
Imaging:
- US- fluid-filled herniation,
with an underlying bony defect.
-
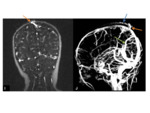
CT- a useful pre-operative tool-used to evaluate the size and boundaries of the osseous defect.
Fig. 8
-
MRI- best imaging modality to evaluate the contents within the encephalocele prior to surgery,
as well as allowing for prognostication.
Encephaloceles may involve the dural venous sinuses,
and MR venogram can be performed to clarify.
Fig. 8
Atretic Cephalocele
Background:
-
Focal,
often midline, extracranial herniation covered by skin.
Usually contains dura,
fibrous tissues and degenerated brain tissues.
There is a connection to the underlying dura via a fibrous stalk.
-
Can be associated with a vertically positioned straight sinus,
anomalies of the tentorial incisura,
persistent falcine sinus, and superior sagittal sinus abnormalities.
Often associated with other intracranial abnormalities
Imaging:
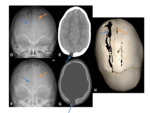
-
US- complex midline lesion, immediately underlying the skin,
with an associated bony defect.
Fig. 9
-
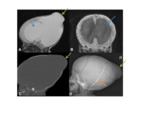
CT- midline lesion,
which is complex/heterogeneous in nature.
CT is used to provide superior bony detail with regards to the bony anatomy.
- MRI- gold standard for delineating the contents.
Cephaloceles are complex in nature,
with CSF signal contents outlining the mixed remnant tissues.
MRV may show an incidental persisting primitive falcine vein,
as well as other anomalies of the venous sinuses.
Fig. 10
Cephalhaematoma
Background:
-
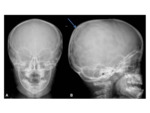
Traumatic subperiosteal accumulation of blood Fig. 11
-
Characteristically,
confined by the cranial sutures Fig. 12 (unlike caput succedaneum and subgaleal haematomas)
-
Often related to birth trauma and is more commonly seen in assisted deliveries- either forceps or vacuum.
-
Majority resorb spontaneously within the first month of life.
-
May become infected,
requiring appropriate antimicrobial therapy,
or even drainage.
-
Rarely,
the haematomas will fail to resorb,
and undergo progressive subpericranial osteogenesis,
resulting in a calcified cephalhaematoma.
These feel solid on examination.
Fig. 15 Fig. 16
Imaging:
-
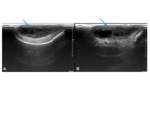
US- anechoeic fluid collection,
confined by the cranial sutures Fig. 12.
Only of use in the non-ossified cephalhaematomas.
-
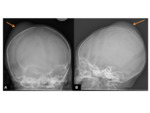
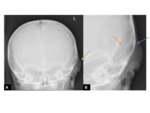
XR- focal soft-tissue collection overlying the bones.
No fracture is usually demonstrated in simple cases Fig. 11 vs Fig. 13 In cases of progressive calcification,
both peripheral,
as well as intralesional calcification can be demonstrated.
Fig. 15
-
CT- crescent-shaped fluid collection adjacent to the outer table of the skull.
The diploic space and innter table remain intact. CT is the gold standard when assessing for ossified cephalhaematomas,
as it nicely demonstrates the hypodense,
non-enhancing core, encased by bone which is continuous with the periosteum.
Fig. 16
-
MRI- can aid in delineating the exact space that the fluid is contained in.
Different signal characteristics can be used to try and age the injury.
Fig. 14
Ping-Pong Fracture
Background:
Imaging:
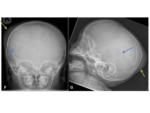
-
XR-depressed skull fracture,
presenting as a smooth inward indentation of the calvarium Fig. 17
-
CT-inner buckling of the calvarium,
but no discrete fracture line is demonstrated. Fig. 18
Growing Fracture
Background:
-
Also known as a leptomeningeal cyst
-
Associated with 1% of skull fractures,
or,
as in this case,
following iatrogenic osteotomies Fig. 19 Fig. 20
-
Occurs when the dura mater is torn.
The inner table of the fracture is exposed to CSF and arachnoid pulsations,
which inhibits healing of the fracture.
Pressure from the pulsations causes bone erosion,
and subsequent widening of the fracture.
-
The orientation of the bony defect is parallel to the original injury,
with the bony defect and resultant cyst elongated in morphology.
Imaging:
-
US- a fluid-filled bony defect.
-
XR- a wide bony defect,
elongated along the length of the fracture.
Interval radiographs will show this to widen in diameter if left untreated.
Fig. 19 Fig. 20
-
CT- as on the radiographs,
a widening fracture over serial studies Fig. 20
-
MR- bony defect,
filled with a cystic lesion.
The contents of the cyst is isointense to the surrounding CSF on all sequences,
and shows communication with the subarachnoid space.
This can form an acquired internal cephalocele,
with mild herniation of meninges and brain tissue.
Lymphovascular Lesions
-
Includes haemangiomas (described below) and other vascular malformations,
including lymphatic malformation,
arteriovenous malformations and venous malformations (described below).
-
Imaging may be necessary if a lesion is clinically significant (ie) affecting the airway,
occluding vision,
show causing overlying ulceration or associated with other anomalies.
Venous Anomaly
Background:
-
Venous malformations are soft,
non-pulsatile,
and of a bluish colour.
-
Low-flow malformations.
- Unlike haemangiomas,
show progressive growth as the child grows.
-
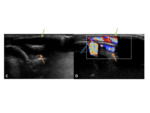
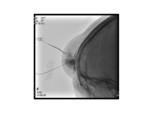
Treatment is a combination of sclerotherapy Fig. 27 and surgical resection.
Imaging:
-
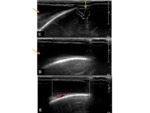
US- is useful as the lesions are superficial.
Ultrasound shows tubular structures,
which will show a venous trace on Doppler evaluation.
Fig. 25
-
CT- a cluster of vessels demonstrated superficially,
which will show variable venous enhancement.
-
MR- T2-weighted images show a high signal lesion,
with areas of septation.
Venogram images show contrast within the lesion.
There are no flow voids,
unlike the more arterialised lesions.
Fig. 26
Sinus Pericranii
Background:
-
Venous abnormality- connection between the intracranial deep venous sinuses and the superficial extra-cranial venous system via a small ostium.
-
Treatment is with ligation of the communicating veins and surgical removal of the sinus.
Imaging:
-
US- venous structure,
with low flow/venous flow on Doppler interrogation.
Valsalva manoeuvres cause increased pressure in the lesion,
and can help confirm the diagnosis.
Fig. 22
-
XR- may show a small osseous defect through which the transcalvarial vein traverses Fig. 21
-
CT- due to the venous nature of the lesion,
CT venography is the most suitable means of assessing the anomalous venous anatomy.
This is demonstrated as dilated venous structures overlying the cranium.
CT also delineates the osseous defect clearly.
Fig. 23
-
MR- as with CTV,
MRV is used to assess for patency of the deep venous structures,
as well as to delineat the abnormal anatomy Fig. 24
PHACES
Background:
-
Suspected if the child presents with a large segmental or plaque-like vascular haemangioma on their face
-
It is an acronym for a spectrum of conditions: Posterior fossa malformations (eg Dandy-Walker malformation).
Haemangiomas.
Arterial anomalies (intracranial).
Coarctation of the aorta.
Eye abnormalities.
Sternal clefting +/- supraumbilical raphe.
-
Not all of the above abnormalities are necessarily demonstrated.
Imaging:
-
Superficial haemangioma- benign endothelial tumour which slowly becomes apparent over the first few weeks of life,
enlarge over the first year of life,
and subsequently undergo clinical involution.
-
The child may undergo further imaging of their aorta and abdomen.
Fig. 28
Neoplastic Lesions
- Important lesions to identify and correctly characterise.
Allows appropriate staging, management,
follow-up and prognostication.
- It can be difficult to differentiate an aggressive from a non-aggresive lesion,
and biopsy is often the gold-standard.
Aggressive Lesions
Background:
Ewing's Sarcoma Imaging:
-
XR- can present in a number of ways,
and can have variable appearances.
Typically,
will have a permeative bone lesion,
with associated lamellated “onion-skin” periosteal reaction.
-
CT- will mimic appearances demonstrated on the plain film.
Often demonstrated as a permeative,
destructive bone lesion,
with extension into the surrounding soft-tissues,
and an aggresive periosteal reaction.
Fig.
29
-
MR- avidly enhancing soft-tissue component.
T1 weighted images may show bony infiltration as low T1 signal. Fig.
30
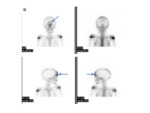
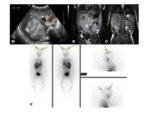
- Nuclear medicine- scintigraphy can demonstrated increased tracer uptake at the site of the primary bone lesion.
Fig.
31
Acute Lymphoblastic Leukaemia Imaging:
-
XR- can present with areas of sclerosis,
permeative destruction,
diffuse osteopenia,
periosteal new bone formation or geographic areas of lysis. Fig.
37
-
CT- bony destruction with enhancing soft-tissue components,
which have both extracranial and extradural components can be seen.
Fig.
37
-
MRI- diffusely abnormal bone marrow signal is best appreciated on T1 weighted images.
Fig.
38
Neuroblastoma Metastases
Background:
-
Bony metastases to the skull can be found in 25% of patients,
with the posterolateral part of the orbit a common location for bony involvement.
-
Clinically,
metastases to the lateral orbital wall can present as “racoon eyes”- periorbital bruising.
Skull lesions can also present as palpable lumps,
proptosis or be found incidentally.
Imaging:
-
XR- can present as a range of radiographic findings.
This includes bony thickening,
“hair-on-end” periosteal reaction,
lytic lesions and irregular separation of sutures.
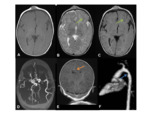
-
CT- cross-sectional imaging is required to demonstrate any epidural deposits.
Bone-windows will also allow evaluation of the hair-on-end periosteal reaction,
as well as the ill-defined sutural margins.
Fig.
39
-
MR- the lesions appear as T2 high signal,
with enhancement following gadolinium.
Fig.
39
- Nuclear medicine studies (MIBG) can help identify distant metastatic disease,
even before the patient presents with the palpable lesion.
Fig.
40
Non-Aggressive Lesions
Myofibroma
Background:
-
Rare tumour- can be solitary or multiple
-
Proliferative disorder,
characterised by the development of firm,
discrete nodules within the dermis and subcutis,
but may also form in the muscle,
bone and viscera.
-
Can resemble a malignant process,
despite being a benign entity.
Imaging:
-
XR- rounded lytic lesions,
with a sclerotic rim.
Can show aggressive periosteal reaction.
Fig. 32
-
CT-well-delineated soft-tissue components,
which are avidly enhancing.
Fig. 33
-
MR- heterogeneous lesions,
depending upon the amount fibrous and collageneous content.
Again,
like on CT,
there is avid enhancement post contrast.
Benign Fibrous Histiocytic Tumour
Background:
Imaging:
-
XR- lobulated,
lytic lesion,
with a very narrow zone of transition,
and a sclerotic rim.
Fig. 34
-
CT- large,
lobulated lesion,
with destruction of the bone.
Soft-tissue component,
with variable enhancement Fig. 35
-
MR- lobulated soft-tissue component,
with patchy,
peripheral areas of enhancement. Fig. 35
Plexiform Neurofibroma
Background:
-
WHO grade 1 tumour of the peripheral nerves.
Uncommon form of neurofibroma,
pathognomonic for neurofibromatosis type 1.
-
Clinically presents as a subcutaneous mass,
which feels like a “bag of worms”
Imaging:
-
CT- non-specific,
subcutaneous lesion
-
MRI- T1 low signal,
T2 high signal,
with mild enhancement.
Fig. 36 There may be other features of NF1.
Pott's Puffy Tumour
Background:
-
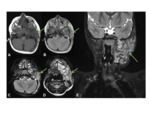
Subperiosteal abscess of the frontal bone secondary to frontal bone osteomyelitis presenting as a subgaleal collection.
This is commonly caused by sinusitis of the frontal sinuses,
with infection spreading to the bone directly,
or via a small network of valveless emissary veins.
-
Treatment includes extensive antibiotic therapy and occasionally surgical draining and wash-out.
Imaging:
-
US- limited role,
could be used in assessing the superficial component.
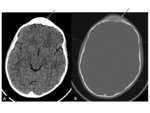
-
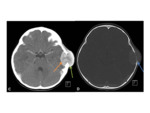
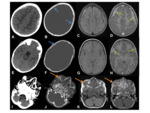
CT- useful in assessing both the bony structures and overlying soft-tissues,
as well as any potential intracranial abnormalities.
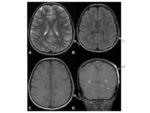
Fig. 41 Windowing the axial slices to bone-windows often reveals opacification of the frontal sinuses.
The overlying scalp can be thickened,
and may demonstrated ill-defined inflammatory change.
Careful interrogation of the bone-windows is necessary to assess for the integrity of the bones,
areas of lucency to suggest a bony defect,
and to look for periosteal reaction.
Contrast-enhanced studies are particularly useful in assessing for intracranial complications.
As in the case illustrated,
contrast-studies also add value in identifying and delineating fluid-collections within the scalp.
CT venogram is the gold standard for assessment of venous sinus thrombosis.
-
MR- more sensitive than CT at detecting subtle or early complications within the adjacent meninges or brain parenchyma.
Fig. 42
Fungal Kerion
Background:
-
An abscess caused by fungal infection- tinea capitis.
Associated with a large,
boggy mass of inflammatory tissue with pustules.
-
Is diagnosed clinically,
with microbioloical confirmation- the use of radiology is rare
-
Imaging plays a role where there is diagnostic ambiguity and atypical features- to both confirm the diagnosis and exclude more sinister differentials.
-
Treatment is with an aggressive course of systemic antifungals.
Imaging:
-
US- will provide a useful superficial examination.
Expected subcutaneous oedema,
and thickening of the scalp tissues.
-
XR and CT- given that the infection is superficial,
there is little role in these imaging modalities.
Changes that may be seen include a focal soft-tissue swelling.
-
MR- areas of inflammation,
presenting as superficial oedema will present as high T2/FLAIR signal,
and corresponding low T1 signal,
with avid enhancement following contrast.
Fig. 43 The excellent soft-tissue contrast resolution of MR will allow for assessment of the extent of infection.
Langerhan’s Cell Histiocytosis
Background:
-
Multisystemic disorder characterised by idiopathic proliferation of Langerhan’s Cells in various tissues
-
The cranium is the common site of osseous involvement
-
Clinically,
the patient presents with a rapidly growing,
tender lump.
Rarely,
patients may present with a pathological fracture through the lesion.
Imaging:
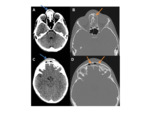
-
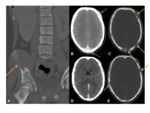
XR- intradiploic lytic lesion,
with non-sclerotic,
borders.
The lesions can either be well-defined- decribed as “punched-out”,
or poorly-defined.
Fig. 44 There is greater involvement of the outer table compared to the inner table- described as having a “bevelled edge”. Lesions can slowly coalesce,
and form geographic areas.
The rapid growth,
and the sometimes ill-defined nature of these lesions can cause diagnostic dilemmas,
raising the possibility of a more aggressive lesion.
When in remision,
the lesions become more sclerotic.
-
CT- characteristics as above. Useful in demonstrating the bevelled appearances of the lesions. Fig. 45 Occasionally a small,
central bony island is demonstrated- a “button sequestrum”.
-
MR- superior to CT in demonstrating the soft-tissue component.
This is T1 low-intermediate signal,
T2 high signal,
and demonstrate marked contrast enhancement.
Fig. 46 The soft-tissue component can have either extradural or extracranial extension.
MRI can be used to assess bone-marrow involvement.
Surrounding reactive change is also well-demonstrated,
and again,
can show enhancement.
Sickle Cell Anaemia
Background:
-
Number of bony manifestations of sickle cell,
much of which relates to marrow hyperplasia
-
Due to improvements in clinical management,
many of these signs are no longer seen radiologically.
Imaging:
-
XR and CT- presents as widening of the diploic space,
thinning of the outer table and a “hair-on-end”.
The end-stage of ongoing haematopoeic activity is expansion of the skull,
and subsequent frontal bossing.
Fig. 47
-
MRI- as above,
there is bony infiltration,
resulting in expansion of the skull bones.
On T1-weighted images,
this is demonstrated as diffuse T1 low signal throughout the bones.
Fig. 47