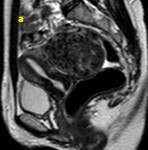
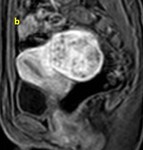
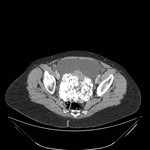
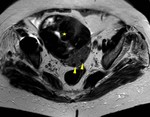
Magnetic resonance (MR) is the most accurate imaging technique for detection and localization of leiomyomas due to its excellent capability to demonstrate the uterine zonal anatomy that enables accurate classification of individual masses as submucosal,
intramural,
or subserosal.
The imaging is quite variable depending of the type of degeneration,
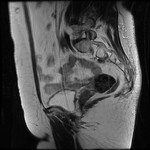
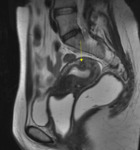
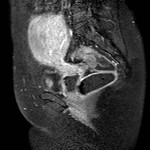
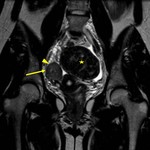
typically the leiomyomas demonstrate distinct low signal intensity relative to that of the myometrium on T2-weighted images,
an intermediate signal intensity on T1-weighted images and demonstrate enhancement on contrast–enhanced images.
These characteristic signal intensities are attributed to extensive hyalinization,
which occurs in more than 60% of uterine leiomyomas.
( Fig. 1 and Fig. 2 )
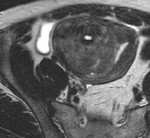
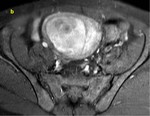
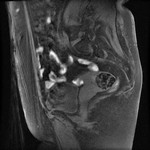
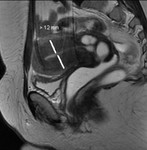
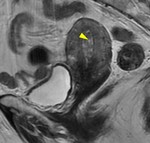
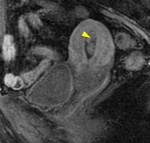
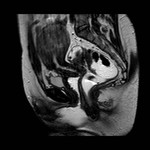
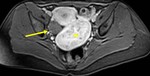
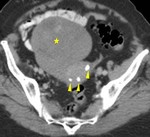
Cystic degeneration is observed in about 4% of leiomyomas that develop cystic spaces that appear as round,
well-demarcated areas that shows high signal intensity on T2-weighted images with no enhancement.
( Fig. 3 and Fig. 4 ).
Myxoid degeneration appears as cystic masses filled with gelatinous material and will demonstrate very high T2 signal intensity and minimal enhancement.
This type of degeneration is important because it may also be seen in leiomyosarcomas and other malignant tumors.
If an extensive myxoid change is seen,
it may be diagnosed as myxoid leiomyoma.
Red or carneous degeneration may exhibit peripheral or diffuse high signal intensity on T1-weighted images and variable signal intensity with or without a low-signal-intensity rim on T2-weighted images.
The entire lesion shows no enhancement,
which indicates complete interruption of blood flow.
Calcification is usually dense and amorphous.
This pattern of calcification at plain radiography almost exclusively indicates the diagnosis of leiomyoma and can be confirm in Computed Tomography ( Fig. 5 ). MRI shows low signal intensity on T2-weighted images,
and complete absence of enhancement in T1- weighted MR with contrast.
( Fig. 6 and Fig. 7 ).
DIFFERENTIAL DIAGNOSIS
The differential diagnosis includes non-myometrial lesions such as focal adenomyosis /adenomyoma and polyps.
Benign ovarian tumors such as fibroma/thecoma as well as malign tumors such us uterine leiomyosarcoma.
Its important to adequately characterize the lesion within the uterus,
to know the relationship of the lesion to the adjacent pelvic organs and structures,
to identify the ovaries and uterus,
and to evaluate the lesion in the patient's clinical context to avoid image pitfalls.
ADENOMYOSIS
- Characterized by the presence of ectopic endometrial glands and stroma within the myometrium,
which are associated with reactive hypertrophy of the surrounding myometrial smooth muscle.
- Commonly a diffuse abnormality,
at MR imaging,
appears as a thickened inner myometrium called as well as junctional zone( JZ ) on T2-weighted images.
( Fig. 8 ).
- But may also occur as a focal mass,
which is known as an adenomyoma.
The distinction from leiomyoma may be challenging; adenomyomas appears as an ill-defined,
poorly marginated area,
usually with low signal on T2 weighted images but may contain small foci of high signal intensity on T2 weighted images ( Fig. 9 ),
that could also presents as high signal intensity on T1-weighted images that would corresponds to hemorrhage.
ENDOMETRIAL POLYP
-
Endometrial polyps are benign localized overgrowths of the endometrium.
Most polyps are small and incidental.
-
On MRI,
polyps are generally well-circumscribed,
isointense on T1 signals and hypointense on T2 signals relative to normal endometrium.
-
Typically have rapid early and persistent enhancement or gradually increasing enhancement.
-
Differentiating between a submucosal leiomyoma and either an endometrial polyp or carcinoma can be achieved by demonstrating the endometrial origin on T2 weighted image of these endometrial pathologies.
( Fig. 10 and Fig. 11 )
UTERINE LEIOMYOSARCOMA
- Leiomyosarcoma may arise in a previously existing benign leiomyoma (sarcomatous transformation) or independently from the smooth muscle cells of the myometrium.
- Although it has been suggested that an irregular margin of a uterine leiomyoma at MR imaging is suggestive of sarcomatous transformation,
there are not specific imaging features stablished to predict accurately the presence of malignancy in a myometrial mass,
because of the imaging findings associated with degenerating leiomyomas can often overlap. ( Fig. 12 and Fig. 13.)
- The diagnosis diagnosis of leiomyosarcoma is established histologically by noting the presence of infiltrative margins,
nuclear atypia,
and increased mitotic figures.
SOLID ADNEXAL MASS
- Fibroma and thecoma are forms of a spectrum of benign tumors.
Lipid-rich thecoma can show estrogenic activity.
Fibroma is the most common sex cord tumor.
- They have a large fibrous component and similar signal intensity to that of a pedunculated leiomyoma.
- MR imaging allows detection and characterization of normal ovaries,
as well as it can demostraste adnexal masses,
ussually surrounded by ovarian stroma and follicles establishing the ovarian origin. ( Fig. 14 and Fig. 15 ).
- CT scan shows homogeneous solid tumor with delayed slight enhancement ( Fig. 16 ).
MRI shows low signal intensity on T1 and T2 weighted image (Fig. 17).
Observation of the interface vessels between the uterus and adnexal masses seems to be useful in differentiating leiomyoma from ovarian fibroma.