TUMEFACTIVE MULTIPLE SCLEROSIS
It is a type of multiple sclerosis that can occur at any age,
most often between 20 and 30 years. Its etiology is unknown.
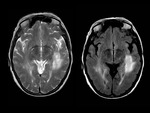
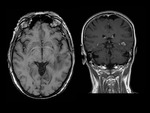
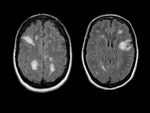
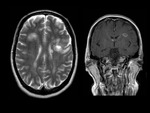
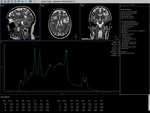
They are pseudotumoral lesions that present as a large intraparenchymal lesion (> 2 cm) with mass effect less than expected for their size.
They can simulate a glioma of low to high grade,
lymphoma,
stroke,
infections and abscesses.
CT is useful in the differential diagnosis with gliomas when it is correlated with MRI,
since the ring seen in the T1 sequence contrasted is marked isodense,
different from that of CT in demyelinating lesions,
which shows a hypodense ring and sometimes not discernible compared to that observed in MRI in contrasting T1 and T2 sequences.
The contrasted CT can,
on occasions,
show an incomplete ring lesion similar to that observed in MRI.
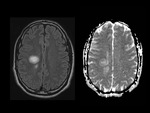
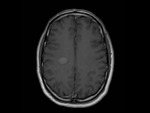
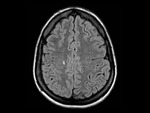
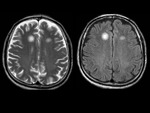
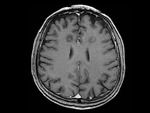
MRI shows large single or multifocal lesions that usually show no mass effect,
there is no cortical involvement and they have scant edema; the latter,
added to incomplete ring uptake in the T1 sequences with gadolinium (open ring sign); the area of enhancement indicates the area of active demyelination and targets the white matter,
different from what occurs in tumor lesions or abscesses,
where the ring is generally complete.
It may be accompanied by other demyelinating lesions in the brain or cervical spinal cord typical of MS.
Another technique described is the dynamic echo gradient sequence (T2 * -w) obtained during the IV administration of the contrast and where structures resembling blood vessels can be observed,
which emerge from the center of the lesion towards a subependymal vein.
which is usually dilated.
Fig.
1,
Fig.
2,
Fig.
3 and Fig.
4.
The sensitivity of the TAC added to the MRI is 97 vs 73.0% for MRI alone.
In MR spectroscopy,
a decrease in N-acetyl aspartate (NAA) peak is observed,
which reflects neuronal loss,
increased resonance intensity of choline peak (CHO) and lipids (LIP),
consistent with membrane breakdown cellular and lactate increase (LAC),
probably due to ischemia secondary to the acute inflammatory process or produced by activated macrophages.
However,
these findings are highly nonspecific,
which is why they lose their validity and has led some authors to conclude that it is not possible to differentiate between tumor and demyelinating lesions by means of spectroscopy; However,
once the demyelinating process becomes chronic,
the peaks of CHO,
LIP,
LAC normalize and the NAA peak persistently remains low,
contrary to what happens in tumor lesions,
where all metabolites continue to be altered,
recommending perform anti-inflammatory treatment and control spectroscopy to discern between both processes.
Fig.
5
Perfusion by MRI also helps to differentiate between neoplastic and demyelinating lesions.
In CNS gliomas and lymphomas,
the regional cerebral blood volume will be markedly increased and the average transit time will be reduced due to the process of angiogenesis,
contrary to that observed in the demyelinating lesions,
where the rCBV is not increased,
or it may even be diminished,
and the average transit time is increased.
ACUTE MULTIPLE SCLEROSIS (MARBURG)
Marburg's disease is an acute,
fulminating,
monophasic and rare variant of multiple sclerosis,
characterized by a rapid and continuous onset of progressive demyelination to death in a period of months after diagnosis.
Unlike the classic form of multiple sclerosis and its variants,
the lesions are confluent,
with a high degree of cell destruction and patches of demyelination.
The clinical course is characterized by a short duration (months),
with a very varied neurological commitment such as: hemiplegia,
aphasia,
spasticity,
deterioration of the state of consciousness and hemianopsia (among other visual alterations).
It has a mortality of less than 4% of all cases of multiple sclerosis.
The severe clinical course of this entity could be explained by the location of the demyelinating plaques in the brainstem or by an aggressive immunological process that has been described in its pathophysiology.
Demyelinating lesions can present clinically as a surgical emergency,
if the lesion acts as a mass on the brainstem causing obstructive hydrocephalus.
Another surgical aspect occurs when there is a single lesion that simulates a primary lymphoma.
MRI shows extensive confluent areas of tumefactive demyelination,
predominantly in the stem and white matter of the hemispheres; with progression of the lesions in the control MRI.
They present perilesional edema with mass effect and defined rings that enhance incompletely.
There are no pathognomonic images of this entity.
DIFFUSE MYELINOCLASTIC SCLEROSIS (SCHILDER)
It is a rare form of demyelinating disease,
also known as diffuse cerebral sclerosis or Schilder's disease.
It is a chronic inflammatory myelinoclastic process with formation of large plaques (extensive demyelination),
diffusely,
in the white matter of both cerebral hemispheres,
often cavitated and with areas of necrosis that show mass effect.
The most frequent age of onset is the pediatric one,
with symptoms that differ according to the location of the main lesions.
Symptoms include intracranial hypertension,
headache,
nausea,
vomiting and decreased level of consciousness.
Within the diagnostic criteria proposed by Posner in 1985 include: 1-2 large plates (lesions more than 2 cm in 2 dimensions) in each cerebral hemisphere (predominantly in semioval centers),
no additional lesions are identified,
no abnormality of the peripheral nervous system,
normal adrenal function,
long-chain fatty acids of normal serum and pathological / histological changes consistent with diffuse subacute / chronic myelinoclastic sclerosis.
MRI shows large demyelinating lesions,
hyperintense in T2-weighted sequences and hypointense lesions in T1-weighted sequences that may have peripheral contrast enhancement.
It predominantly affects the posterior white matter of both cerebral hemispheres,
with a sometimes relatively symmetrical distribution.
The differential diagnosis must be made with pathologies such as progressive multifocal leukoencephalopathy,
acute disseminated encephalitis or adrenoleukodystrophy (with the latter being differentiated because adrenal function and very long chain fatty acid levels are normal in Schilder's disease).
As in all forms of aggressive MS,
it is also necessary to differentiate them from tumor or infectious lesions.
The definitive diagnosis is given by the brain biopsy.
The majority of patients present a fatal course,
although there are cases with a better prognosis.
The treatment used is similar to other demyelinating pathologies: corticosteroids and immunosuppressants.
Corticosteroid therapy seems to be effective in the radiological improvement of the lesions.
CONCENTRIC SCLEROSIS (BALÓ)
Baló's concentric sclerosis is a rare variant of MS that is pathologically characterized by the presence of lesions with alternating bands of demyelinated and normally myelinated white matter,
which give the lesion a configuration in concentric bands or with a mosaic pattern.
This rare variant of MS appears more frequently in young subjects of Asian origin,
presenting an acute monophasic course.
In the cases described,
it can occur fatally,
with the death of the subject in a few weeks after the onset of symptoms.
MRI shows areas of concentric demyelination between myelinated areas of white matter in the form of hyperintense / hypointense rings in T2-weighted sequences.
Contrast uptake can be observed,
especially at the periphery of the lesion,
in T1 sequences.
It has been argued that the conserved concentric areas are actually different stages of the demyelinating lesion,
since they show a decrease in glial cells and myelin,
but in a milder form than in the demyelinated areas.
Fig.
6 and Fig.
7.
The course of the disease,
sometimes fatal,
requires establishing a diagnosis as soon as possible and initiate treatment of the EM outbreak,
that is,
high-dose steroids.
The use of immunosuppressants seems to be indicated by the associated poor prognosis.
NEUROMYELITIS OPTICA (NMO)
Classically it has been considered as a variant of MS,
although currently it is known that it belongs to another group of pathologies; however,
we are going to mention it as a differential diagnosis of all those previously seen.
Also called Devic's syndrome,
it is a demyelinating disease that affects almost exclusively the optic nerve and the spinal cord,
and consists of a combination of bilateral optic neuropathy and cervical myelopathy.
There is no or very little demyelinating affectation of other territories,
at least in the typical form of this entity.
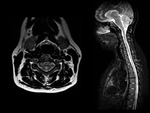
Think of the NMO when there are extensive spinal cord injuries (more than 3 vertebral segments).
Injuries often involve most of the medullary cord unlike MS where the lesions are smaller and peripheral.
In its etipatogenia,
autoantibodies to the water channel of aquaporin-4 have been seen.
The findings of the optic nerve in MRI are: signal hyperintensity in T2-weighted sequences and enhancement of the optic nerve,
by disruption of the blood-brain barrier,
(BBB) after the administration of gadolinium.
These alterations can extend to the optic chiasm.
The STIR sequence facilitates the assessment of the optic nerve.
The spinal lesions are extensive,
symmetrical and central,
covering 3 or more vertebral segments.
It is the most characteristic radiological finding (unlike MS) (generally <2 vertebral segments,
incomplete,
not central).
They are located mainly in the cervical and thoracic regions,
with spinal cord edema observed,
with hyperintensity in T2-weighted and hypointensed sequences in T1.
There may be enhancement after gadolinium administration until months after the episode of acute myelitis.
In more advanced stages of the disease or in more severe forms,
atrophy and cavitations may be observed.
Fig.
8 and Fig.
9.
Generally no alterations are observed in the cerebral parenchyma,
although non-specific lesions may appear in the brainstem,
hypothalamus and ependyma.
Acute Disseminated Encephalomyelitis (ADEM) is an important differential diagnosis of MS.
This is a monophasic,
immune-mediated demyelinating disease which often presents in children following an infection or vaccination.
On MRI there are often diffuse and relatively symmetrical lesions in the supra-and infratentorial white matter which may enhance simultaneously.
Fig.
10 and Fig.
11.
There almost always is preferential involvement of the cortical gray matter and the deep gray matter of the basal ganglia and thalami.