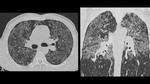
Radiological findings in patients with the chronic form of paracoccidioidomycosis are very diverse and there is frequently a combination of patterns such as reticular and nodular opacities,
airspace consolidation,
cavities and fibrotic lesions showing a tendency for bilateral and symmetrical distribution [6] and usually involving more than one third of the lungs (Fig.
2); however,
pleural effusion and pulmonary calcifications are seldom observed.
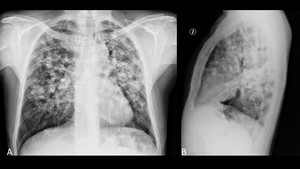
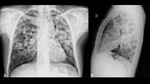
Fig. 2: Chest plain radiograph.Frontal (A) and lateral (B) views. Bilateral ill-defined nodules along with reticular opacities predominantly in middle and upper lung zones.
References: Department of Radiology, Clínica Universitaria Bolivariana / Medellín 2017
A discrete predominance in the middle lung zones has been reported and its association with lower lobe emphysema could suggest the diagnosis when found in patients living in endemic areas.
Nevertheless,
the myriad of imaging patterns previously described makes differential diagnosis with other pathologies imperative,
especially pulmonary tuberculosis which can coexist in 10% of patients with paracoccidioidomycosis [2].
Interestingly,
up to 35% of patients with radiographic abnormalities can be completely asymptomatic,
reflecting a clinical-radiological dissociation (7).
High resolution CT (HRCT) demonstrates lung disease in 93% of patients [8].
Ground glass opacities are noted in around 58% and represent the most common abnormality in those individuals who have not received treatment [9].
Centrilobular nodules,
parenchymal bands,
interlobular septal thickening,
areas of cicatricial emphysema,
consolidations,
traction bronchiectasis,
cavitations and architectural distortion are regularly seen [10].
Next,
we describe a series of 7 adult patients with pathology confirmed pulmonary paracoccidioidomycosis and relate their radiologic findings to some of the main imaging characteristics of this clinical entity.
All of them were rural workers,
including a female.
Either HRCT or contrast enhanced CT of the thorax were performed using 16 and 64 MDCT scanners and images were reviewed using both lung and soft tissue windows with multiplanar reformations.
Additionally,
images of extrapulmonary disease are included to illustrate its polymorphic presentation and emphasize the importance of differential diagnosis.
- Consolidations: they generally have a patchy appearance and correspond to areas of acute alveolitis with an inflammatory exudate (Fig.
3).
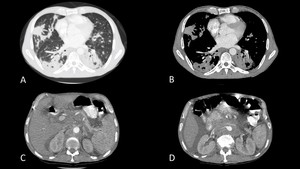
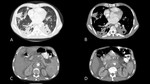
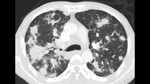
Fig. 3: Chronic paracoccidioidomycosis in a 42-year-old male. Contrast enhanced CT of the thorax in lung (A) and soft tissue windows (B) depicting irregular airspace consolidations involving both lungs. Contrast enhanced CT of the abdomen in the same patient (C and D) demonstrating spleen infiltration as well as retroperitoneal lymph node enlargement.
References: Department of Radiology, Hospital Universitario San Vicente Fundación / Medellín 2017
- Ground glass opacities: usually result from inflammatory alveolar wall thickening or fibrosis that may be accompanied of partial airspace filling (Fig.
4).
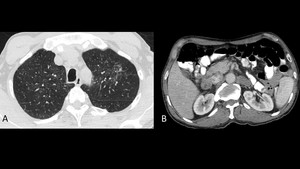
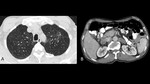
Fig. 4: 63-year-old male with Addison’s disease secondary to chronic paracoccidioidomycosis. High resolution CT (A) showing subtle ground glass opacities in both upper lobes. Contrast enhanced CT of the abdomen (B) with evidence of a 26mm mass in the right adrenal gland and a 33mm mass in the contralateral gland.
References: Department of Radiology, Hospital Universitario San Vicente Fundación / Medellín 2017
- Nodular pattern: it can either present as random micronodules (Fig.
5 and 6) or irregular macronodules (Fig.
7).
The former nodules have been demonstrated to correlate with interstitial epithelioid granulomas and have more irregular shapes than those found in miliary tuberculosis [11],
although this can be difficult to differentiate in clinical practice and can also be found in other systemic mycosis like histoplasmosis.
On the other hand,
macronodules can resemble those of other infectious diseases,
neoplastic processes [12] and even rheumatologic conditions such as granulomatosis with polyangiitis.
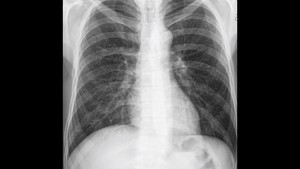
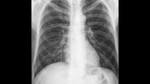
Fig. 5: 53-year-old patient who had previously worked in a cotton plantation. Chest radiograph demonstrates multiple micronodules in both lungs
References: Department of Radiology, Hospital Universitario San Vicente Fundación / Medellín 2017
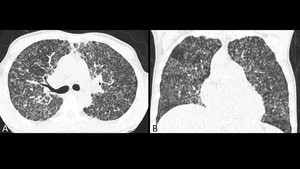
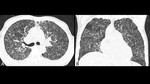
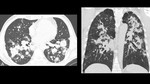
Fig. 6: Same patient as in figure 5. High resolution CT in axial (A) and coronal (B) planes confirming the presence of miliary nodules resembling tuberculosis.
References: Department of Radiology, Hospital Universitario San Vicente Fundación / Medellín 2017
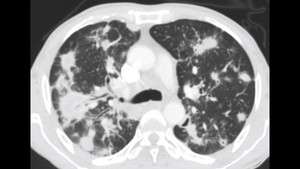
Fig. 7: Male rural worker with chronic paraccocidioidomycosis. Contrast enhanced CT in axial plane revealing multiple nodules with irregular contours, some of them surrounded by a subtle ground glass halo.
References: Department of Radiology, Hospital Universitario San Vicente Fundación / Medellín 2017
- Cavitations: commonly arise from nodules,
consolidations or masses that later undergo necrosis.
Again,
one of the main considerations to keep in mind is the differential diagnosis with tuberculosis as well as cavitating pulmonary metastases (squamous cell carcinomas account for 70% of these lesions) and septic emboli (Fig.
8).
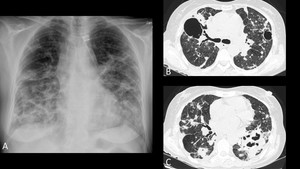
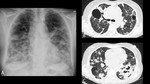
Fig. 8: 49-year-old female with 10 months of cough, occasional hemoptysis, weight loss and intermittent fever. Chest radiography (A) depicts bilateral areas of airspace consolidation, fibrotic changes and some cavitations. High resolution CT (B and C) better illustrates the architectural distorsion and cavitations associated to chronic paracoccidioidomycosis.
References: Department of Radiology, Hospital Universitario San Vicente Fundación / Medellín 2016
As mentioned earlier,
extrapulmonary lesions can be the first presentation of chronic paracoccidioidomycosis and this can eventually lead to delays in diagnosis,
so a high index of suspicion is needed in patients with epidemiological risk factors so prompt treatment can be initiated (Fig.
9 to 12).
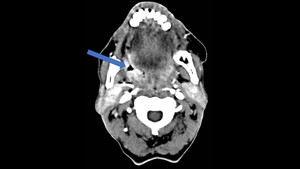
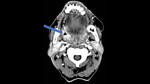
Fig. 9: 45-year-old rural worker with an ulcer in the oropharynx. A previous biopsy had been performed suggesting a malignant lesion. Contrast enhanced CT reveals thickening, irregularity and increased enhancement of the oropharyngeal mucosa along with some air at the site of the biopsy (arrow)
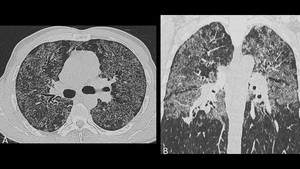
Fig. 10: Same patient as in figure 9. High resolution CT in axial (A) and coronal (B) planes demonstrating multiple random and confluent micronodules in both lungs. The patient was initially misdiagnosed as having an oropharyngeal cancer with pulmonary dissemination and posteriorly went into surgery. The histopathological analysis of the surgical specimen ruled out malignancy and confirmed paracoccidioidomycosis.
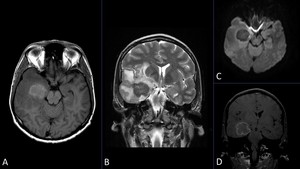
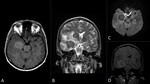
Fig. 11: 51-year-old male with headache and dizziness in the last year. MR images show a nodular lesion in the right temporal lobe which is hyperintense in T1 WI(A) and markedly hypointense in T2 WI (B);it presents peripheral enhancement after the injection of contrast agent (C) but there is no diffusion restriction (D). Note the midline deviation and uncal herniation.
References: CediMed / Medellín 2017
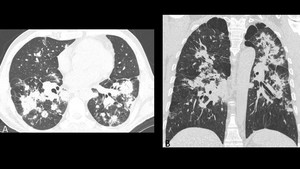
Fig. 12: Chest CT corresponding to the same patient in figure 11. Axial (A) and coronal (B) images. Multiple coalescing nodules with random distribution are visualized in both lungs; some of these nodules present spiculated borders and ground glass halo and are accompanied of interlobular septal thickening as well as paraseptal emphysema.