IMAGING FEATURES IN IDIOPATHIC INTRACRANIAL HYPERTENSION
Neuroimaging in IIH has traditionally performed to exclude other causes of elevated ICP,
such as space-occupying mass lesion and venous sinus thrombosis.
However,
it has become clear that a variety of imaging findings involving the orbit,
skull base,
brain and transverse sinuses are commonly found in patients with IIH.
Hence,
latest diagnostic scheme for IIH incorporates imaging findings as criteria for a diagnosis of "possible IIH" when papilledema is absent.
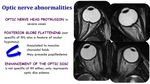
Optic nerve abnormalities
- Optic nerve head protrusion in severe cases
- Posterior globe flattening (not specific of IIH; also a feature of ocular hypotony.
Associated to macular choroidal folds.
May precede papilledema.
- Enhancement of the optic disc is not specific of IIH either; only represents optic dis edema.
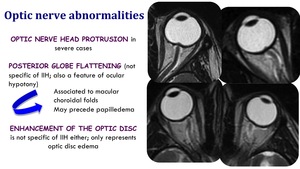
Fig. 10: Optic nerve abnormalities in IIH
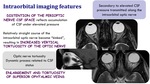
Intraorbital imaging features
- Distention of the perioptic nerve CSF space reflects accumulation of CSF under elevated pressure.
Secondary to elevated CSF pressure transitted along the intraorbital optic nerve.
- Relatively straight couse of the intraorbital optic nerve become "kinked",
resulting in increased vertical tortuosity of the optic nerve. Optic nerve tortuosity is a dynamic process related to CSF status.
- Enlargement and tortuosity of superior ophtalmic veins.
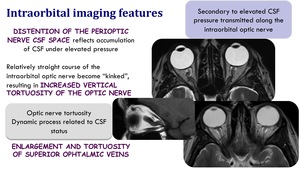
Fig. 11: Intraorbital imaging features in IIH
Osseous erosions and remodelling at skull base
- Remodeling from the chronic IIH cause widening of the bony canal of the skull base.
- Increase the size of the bony pituitary fossa with minimal effect on the pituitary size leading to partial empty sella turcica.
This causes an herniation of the subarachnoid space to the anterior sella turcica diaphragm.
- Enlargement of foramen ovale,
jugular foramen and hypoglossal canal.
- Widening of the optical canal; associated with the severity of papilledema and poor visual function.
Each milimeter increase in bony optic canal size associated with a 0.50 dB decrease in Humphrey visual field mean deviationm and with grade 4-5 papilledema or optic atrophy.
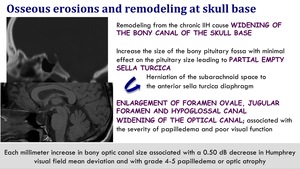
Fig. 12: Osseous erosions and remodelling at skull base in IIH
Enlargement of CSF spaces
- Skull base meningoceles and encephaloceles. Meningoceles surrounding cranial nerve III in the cavernous sinus,
along hypoglossal canal and involving the geniculate fossa.
- Enlargement of the Meckel cave as frank meningoceles in 10% of IIH patients.
- Scalloping of the intracranial surface of the bony skull (osteodural defects); ocassionally can transmit frank meningoceles or encephaloceles protrudings into sinonasal cavities or mastoid temporal bone that results in CSF leaks.
Pachymeningeal enhancement and sagging of the brain is uncommon.
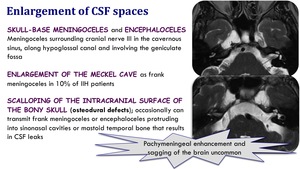
Fig. 13: Enlargement of CSF spaces in IIH
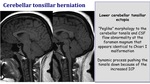
Cerebellar tonsillar herniation
Lower cerebellar tonsilar ectopia.
"Peglike" morphology to the cerebellar tonsils and CSF flow abnormality at the foramen magnum that appears identical to Chiari I malformation.
It is a dynamic process pushing the tonsils down because of the increased ICP.
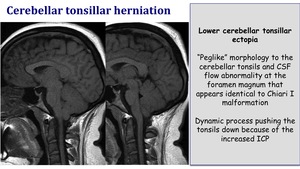
Fig. 14: Cerebellar tonsillar herniation in IIH
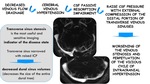
Transverse sinus stenosis
Most patients with IIH have anatomical abnormalities of the cerebral venous system.
Stenosis of the dominant or both transverse sinuses that affects the lateral margins of the sinuses:
- Extrinsic stenosis: smooth gradually narrowing tapered stenosis
- Intrinsic type: stenosis due to arachnoid granulations or fibrous septae.
Degree of stenosis does not correlate with ICP or visual loss.
Elevated venous sinus pressure in the setting of stenosis may impair CSF drainage at the arachnoid granulation tissue exacerbating a cycle of intracranial hypertension.

Fig. 15: Transverse sinus stenosis in IIH
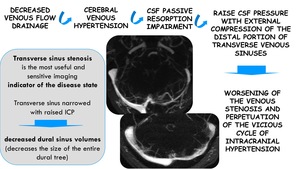
Fig. 16: Physiopathology of IIH and transverse sinus stenosis
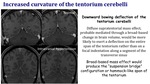
Increased curvature of the tentorium cerebelli
Downward bowing deflection of the tentorium cerebelli.
Diffuse supratentorial mass effect,
probably mediated through a broad-based change in brain volume,
would be more likely to exert a deflection on the entire span of the tentorium rather than on a focal identation along a segment of the transverse sinus.
Broad-based mass effect would produce the "suspension bridge" configuration or hammock-like span of the tentorium.
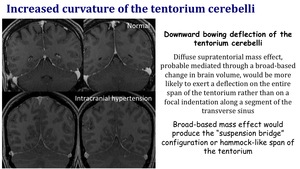
Fig. 17: Increased curvature of the tentorium cerebelli in IIH
Significance of arachnoid granulations
There is a relationship between presence of arachnoid granulations and IIH.
Arachnoid granulations seem to act in a compensatory mechanism in patients with IIH.
Patients with IIH have more arachnoid granulations than general population.
They are inversely associated with imaging findings of IIH and play a role in homeostasis and hence in the pathogenesis of IIH.
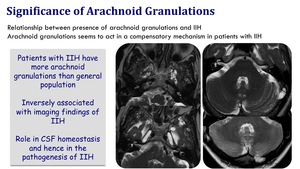
Fig. 18: Significance of arachnoid granulations in IIH
IMAGING FINDINGS IN SPONTANEOUS INTRACRANIAL HYPOTENSION
Brain MRI may be normal in 20% of patients with SIH.
CRANIAL SIGNS:
- Subdural fluid collections (hygromas,
hematomas)
- Enhancement of the pachymeninges (diffuse,
smooth,
uniform)
- Engorgement of venous structures
- Pituitary hyperermia
- Sagging of the brain (flattening of pons,
effacement of basal cisterns,
bowing of optic chiasm,
descent of cerebellar tonsils)
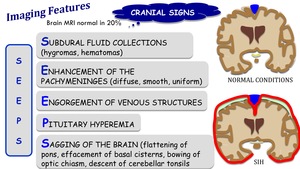
Fig. 19: Imaging features of spontaneous intracranial hypotension
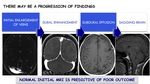
There may be a progression of findings:
Initial enlargement of veins ⇒ dural enhancement ⇒ subdural effusion ⇒ sagging brain
Normal initial brain MRI is predictive of poor outcome.
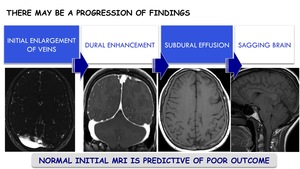
Fig. 20: Progression of brain MRI findings in SIH
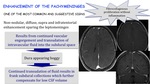
Enhancement of the pachymeninges:
It is one of the most common and suggestive signs.
Typically non-nodular,
diffuse,
supra and infratentorial enhancement sparing the leptomeninges.
Results from continued vascular engorgement and transudation of intravascular fluid into the subdural space.
⇓
Dura appears boggy
⇓
Continued transudation of fluid results in frank subdural collections which further componsate for low CSF volume.
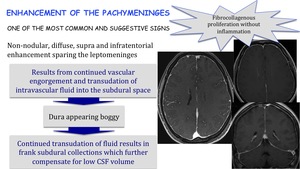
Fig. 21: Enhancement of the pachymeninges in SIH
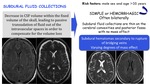
Subdural fluid collections:
Risk factors: male sex and age >35 years.
May be simple or hemorrhagic,
often bilaterally.
Subdural fluid collections are thin on the cerebral convexities and posterior fossa with no mass effect.
Subdural hematomas are secondary to rupture of bridging veins and have varying degress of mass effect.
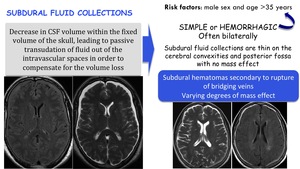
Fig. 22: Subdural fluid collections in SIH
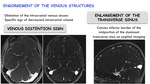
Engorgement of the venous structures:
Venous distention sign: produced by dilatation of the intracranial venous sinuses.
It is a specific sign of decreased intracranial volume.
Enlargement of the transverse sinus: convex inferior border of the midportion of the dominant transverse sinus on sagittal imaging.
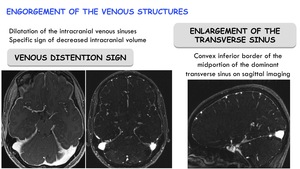
Fig. 23: Engorgement of the venous structures in SIH
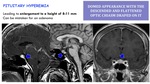
Pituitary hyperemia:
Leading to enlargement to a height of 8-11 mm.
Can be mistaken for an adenoma.
It has a domed appearance with the descended and flattened optic chiasm draped on it.
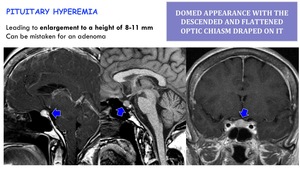
Fig. 24: Pituitary hypermia in SIH
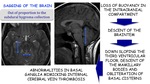
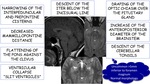
Sagging of the brain:
Out of proportion to the subdural hygroma collection.
Loss of buoyancy in the intracranial compartment
⇓⇓
Descent of the brainstem
⇓⇓
Down sloping the third ventricular floor,
descent of the mamillary bodies and obliteration of basal cisterns
⇓⇓
Abnormalities in basal ganglia mimicking internal cerebral vein thrombosis.
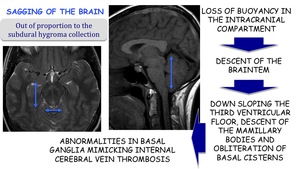
Fig. 25: Sagging of the brain in SIH
Other imaging findings related to sagging brain:
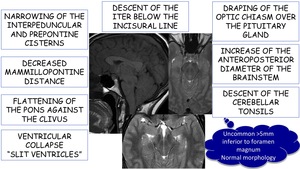
Fig. 26: Other imaging findings related to sagging brain in SIH
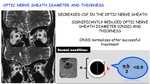
Optic nerve seath diameter and thickness:
Decreased CSF in the optic nerve sheath
⇓⇓⇓
Significantly reduced optic nerve sheath diameter (ONSD) and thickness
ONSD normalizes after successful treatment
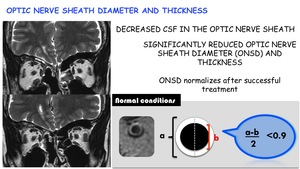
Fig. 27: Optic nerve sheath diameter and thickness in SIH
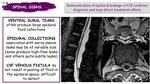
SPINAL SIGNS:
Ventral dural tears often produce large epidural fluid collections.
Epidural collections associated with nerve sleeve leaks may be of variable size (some produce high-flow leaks and others quite subtle leaks).
CSF venous fistula do not result in pooling of fluid in the epidural space; difficult to detect.
Demonstration of epidural leakage of CSF confirms diagnosis and may direct treatment efforts.
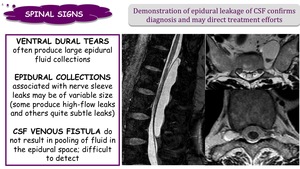
Fig. 28: Spinal signs in SIH
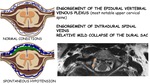
Engorgement of the epidural vertebral venous plexus (most notable upper cervical spine)
Engorgement of intradural spinal veins
Relative mild collapse of the dural sac
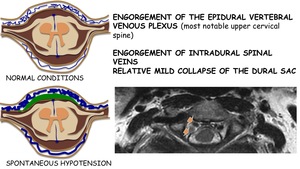
Fig. 29: Spinal venous engorgement in SIH
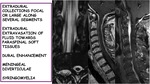
Extradural collections focal or large along several segments
Extradural extravasation of fluid towards paraspinal soft tissues
Dural enhancement
Meningeal diverticulae
Syringomielia
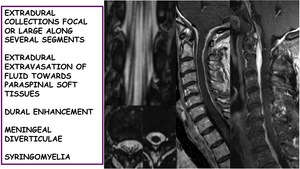
Fig. 30: Other spinal findings in SIH
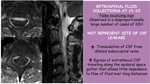
Retrospinal fluid collections at C1-C2
They are a false-localizing sign observed in a large number of cases of SIH.
Not represent site of CSF leakage and reveals:
- Transudation of CSF from dilated suboccipital veins
- Egress of extrathecal CSF traveling along the epidural space gutter that allows little impedance to flow of fluis over long distances
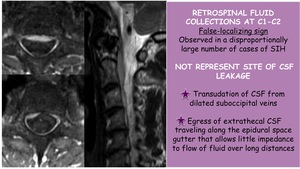
Fig. 31: Retrospinal fluid collections at C1-C2 in SIH
Looking for the CSF leak....
Both CT myelography and MRI (conventional and heavily T2WI) are capable of identifying large leaks when epidural fluid is abundant.
CT myelography:
- Superior at demonstrating slow-flow leaks
- Superior anatomic detail (calcified disk herniations)
- Detect CSF-venous fistulas (not visible on MRI)
- Best choice for many authors for the initial evaluation of SIH
- Disadvantage: invasive (lumbar puncture) and ionizing radiation
MRI:
- Widely available and noninvasive
- Initial screening study at some centers.
Negative MRI ⇒⇒ CT myelography
- MR Myelography using intrathecal gadolinium may identify some leaks not seen at CT; off-label use and reserved for selected cases.