MATERIALS
Our collection of artefacts in prostatic elastography was carried out using various systems equipped with different elastography algorithms for SE (Resona 7, Mindray,
China; MyLab Twice HD and MyLab 8,
Esaote,
Italy; Hi-Vision EUB 8500 and Preirus,
Hitachi Medical System,
Japan; Logiq E9,
GE Healthcare,
USA).
For SWE only one system was available on the market until recently (Aixplorer,
SuperSonic Imagine,
France).
TRANSDUCER CHOICE
Although bi-convex and linear transducers are available,
the end-fire convex transducer is generally preferred for SE; prostatic SWE is currently supported by end-fire curved transducer only.
EXAMINATION TECHNIQUE
The examination technique varies between SE or SWE methods.
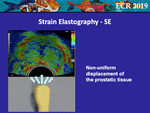
In SE,
a series of minimal compressions and decompressions induced with the transducer are necessary to obtain the right displacement of the prostatic tissue,
while the probe is maintained in a fixed position or moved along the prostate surface in transverse scan [12].
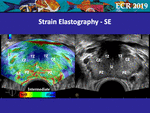
SE estimates the relative tissue stiffness of the prostate by visualising the differences in strain among adjacent regions.
To obtain a correct estimation,
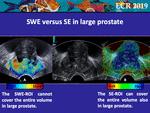
the elastography region of interest (ROI) should be wide and cover the prostate and the surrounding fatty tissue but,
when possible,
avoid the bladder which is a no strain zone [12,
13] (Fig.
1).
The SE-ROI size wideness is not limited in itself; however,
the tissue displacement far from the probe may be insufficient to be measured,
resulting in incorrect coding on the map.
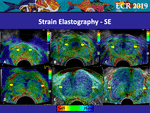
The regular SE pattern varies with age and the inner gland volume (Fig.
2).
In SWE,
data are acquired by examining the prostate in transverse scans,
slowly moving the transducer from base to apex,
while avoiding manual transducer pressure to minimise pre-compression artefacts.
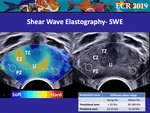
SWE distinguishes the prostatic zones that are characterised by different stiffness values (Fig.
3).
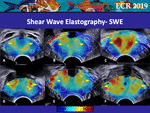
The regular SWE pattern varies with age and the inner gland volume (Fig.
4).
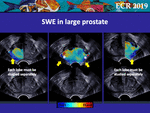
The SWE-ROI size is limited by physics of shear wave propagation and allows simultaneous visualisation of the two lobes only in small and medium volume prostates (Fig 5); to overcome this limitation,
in large prostate the peripheral zone of each lobe must be studied separately (Fig.
6).
With SWE the ROI size doesn’t affect the map representation of the absolute tissue stiffness.
TYPES OF ARTEFACTS
Both techniques are affected by multiple artefacts which should be known in detail.
In SE,
the map varies according to the type of tissue present within the ROI,
the ROI size and the distance from the probe.
However,
the manual compression and decompression are relatively uncontrolled elements,
with wide variability.
Thus,
images affected by artefacts have been found in up to 32% of cases [14].
Moreover,
some artefacts are related to the algorithm used by specific systems.
In SWE,
the map reflects the shear wave propagation,
which may be affected by different factors such as beam penetration,
tissue uniformity and tissue pre-compression.
With SWE,
it is critical to avoid any pressure on the prostate gland applied by the transducer [15].
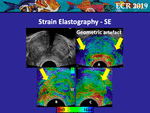
• Geometric Artefact
The prostate is studied for the characterisation of abnormal lesions and detection of stiff suspected areas.
Because of its geometric characteristics and a reduced contact surface,
the convex transducer produces a non-uniform distribution of the pressure during the SE acquisition (Fig.
7),
thus generating lateral artefacts [3].
Their presence becomes more evident in large prostates.
In some systems,
the algorithm assigns the stiff code to every not-displaced target,
independent from their real stiffness.
As a consequence of the reduced tissue displacement due to the transducer geometry,
the lateral sides of large glands are displayed as stiff (Fig 8A).
This common artefact can be overcome by tilting the probe laterally (Fig 8B).
The same artefact can be observed in the fatty tissue neighbouring to the lateral sides of the prostate,
which might be not-displaced in some condition (Fig 9A).
In some systems,
the algorithm assigns the soft code to the fatty tissue,
even when it is not adequately displaced by manual compressions (Fig.
9B).
Concerning the limited width of the SWE-ROI and in particular to the different physical principle on which the SWE technique is based,
the correspondent SWE map is not affected by geometric artefacts.
• Color Noise Artefacts
With SE,
the frequency of the micro-compression should remain constant,
allowing the scanner to assign the correct displacement average value for every pixel of the image.
It reduces background signals (“colored noise artefacts”) brief,
non-reproducible flashes of apparent stiff pixels that affect the image quality [12].
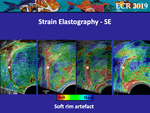
• Soft Rim Artefact
At SE a thin periprostatic border,
known as the “soft rim artefact,” can be seen and suggests that the prostate is freely movable within the periprostatic tissues.
These areas will be depicted as soft,
meaning that large displacements are seen from one frame to the next [16].
Its presence also reflects the difference in relative elasticity between the prostate and the adjacent tissue,
which contains the periprostatic venous plexus [12].
The “soft rim” visualisation and its thickness may depend on the axial resolution and sensitivity of the scanner or the dynamic range setting (Fig.
10).
Some authors have proposed this as a marker of capsule integrity in prostate cancer [17].
However,
this artefact is not always visualised even in normal prostate: in a study it was observed in only 73% of cases and its complete visualisation was possible on only 12% [12].
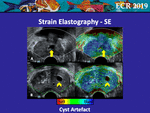
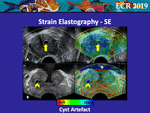
• Cyst Artefacts
In cyst,
when SE measures the tissue displacement between subsequent frames,
random noise is detected.
The noise may be displayed in different ways depending on the algorithm used by the system.
The two most commonly described artefacts are the “3-layer pattern” [18] (Fig 11A) and “bull’s eye artefact” (Fig 11B) [19].
These artefacts are considered useful since they highlight the cystic nature of the target,
even when internal echoes are present.
Frequently some small cysts may be coded as a target of an intermediate or absent displacement (Fig 12A and 12B),
thus creating problems of interpretation; in this condition,
the B-mode image represents the key to understanding.
SWE imaging usually shows the cyst as a blanked cavity because shear waves don’t propagate into the fluid.
However,
sometimes SWE shows the cyst in the map coded as tissue without any significant stiffness,
which represents an artefact.
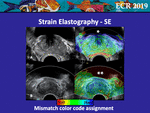
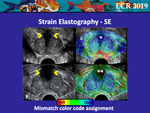
• Mismatch Color Code Assignment
In some systems,
during the SE processing,
an area of fluid collection (such as the bladder or a vessel) in which the transducer detects any radiofrequency variation of the signal is displayed as blanked in the color-coded map (Fig 13A),
thus clearly showing the absence of scattering inside the cited area.
In other systems a soft code (Fig 13B) or a hard code (Fig 12A) are assigned to these targets,
thus generating a mismatch in the color-code assignment.
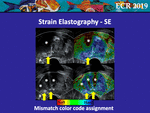
Sometimes a mismatch in the code assignment may also happen in areas of solid tissue where extremely low amplitude echoes,
related to the US beam attenuation,
are displayed in the B-mode image.
In this condition,
some systems may assign a soft code to anatomical structures by themselves stiff,
since they are misinterpreted as anechoic areas.
These artefacts can be observed for example in the peri-urethral tissue,
at the bladder neck,
which frequently appears hypoechoic (Fig.
14) or along the acoustic shadow of a calcification (Fig.
15).
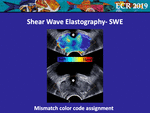
With SWE,
a mismatch in the color-code assignment may happen when the system cannot measure the shear waves propagation.
This phenomenon becomes evident in areas of highly stiff tissue such as cancer with significant shadowing or in case of marked shadowing behind calcifications [20].
It can also be seen at the level of the bladder neck; in these cases,
the stiff tissue is coded as a lack of shear wave signal (Fig.
16).
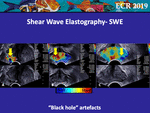
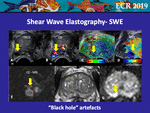
• Black Hole Artefacts
Another example of this lack with SWE can be seen in small prostatic cancers.
This artefact,
which was not explicitly described before in prostate elastography,
can be named “black hole sign”.
Usually,
only cysts are displayed as a blanked round cavity.
However,
signals also absent in small hypoechoic lesions may be suspicious.
This is because cancer stiffness is related to the amount of stromal matrix,
but also depends on the lesion shape and the tensile pressure inside the tumor,
which is dependent on the increased vascularization.
Consequently,
a small rounded lesion behaves with a shell that can refract the shear waves heating the rounded surface at the lesion boundary.
In these conditions,
the propagation velocity of the shear waves inside the lesion cannot be measured.
Thus,
the lesion is displayed as a “black hole”.
In contrast,
stiff signals,
a consequence of the lesion “shell”,
are shown in the surrounding (Fig.
17 and Fig.
18).
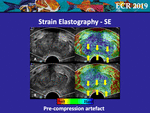
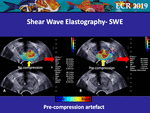
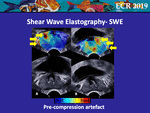
• Pre-compression Artefacts
Pre-compression of the prostatic tissue can affect the displayed map for both the SE and the SWE maps.
These artefacts can be generated by the external pressure exerted on the prostate with the endorectal probe,
or by the internal compression on the peripheral zone.
At SE,
the pre-compression of the peripheral zone affects the regular tissue displacement,
thus mimicking chronic disease or cancer lesions (Fig.
19).
At SWE,
it also influences the quantitative measurement of the tissue stiffness,
thus inducing a wrong finding (Fig.
20).
Another condition that may affect the SWE map is the decubitus which may generate an asymmetric pre-compression on the prostate.
In detail,
the patient usually is lying in the left lateral position,
and this might alter the compressibility of the right side of the prostate; the same artefact becomes evident on the left side of the prostate when the patient is lying in the right lateral position (Fig 21).
This artefact may result in a potential cause of misdiagnosis.