The study enrolled 128 patients with chronic shoulder pain (61 male and 67 female),
with a mean age of 57 years (from 18 to 83 years)
and 35 asymptomatic patients with a mean age of 56 years (from 45 to 87 years).
All patients were examined by traumatologist and underwent complex examination using the following methods: conventional shoulder radiography,
ultrasound examination,
MRI,
MDCT, MR-arthrography,
followed by arthroscopy.
To establish bone-cartilaginous element’s condition and the type of tendon/ligament changes MDCT and MR-arthography and arthroscopy were performed.
Clinical examinations included specific tests for SIS carried out by orthopedist/traumatologist.
ASES shoulder score was used to assess the pain and disability level.
The signs of SIS were identified with conventional shoulder X-ray,
with further MDCT measurements.
Special angles were used to evaluate scapulohumeral topology (Acromial inferior protrusion related angles Fig.
1 , distance indicative of Humeral head superior migration and and Angles defining Lateral extension of the acromion Fig. 2 , Angles defining acromion type Fig. 3 ).
Examination took place between 06.2015 and 04.2018.
Control group consisted of 35 patients examined using identical scheme with identified shoulder osteoarthritis and no pain present.
Special angles and distances were estimated on a work station independently by 2 radiologists with experiences ranging from 4 to 38 years.
Final values determined in consensus.
Repeated measurements were taken in 1 week interval by one of the radiologists.
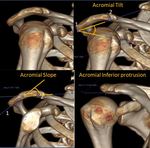
Acromial inferior protrusion related angles.
1) Acromial Tilt (AT). First line was drawn across the inferior part of the acromion from its most posterior to the most anterior points.
Second line connected inferior tip of the coracoid process and the most posterior point of the inferior acromion.
The angle between the lines measured the acromial tilt (AT) (fig.1).
2) Acromial slope (AS).
First line was drawn from the most anterior point of the inferior acromion passing though the midpoint of the anterior acromion.
Second line was drawn from the most posterior point of the inferior acromion through the same midpoint of the inferior acromion.
The angle at the intersection of these lines measured the acromial slope (AS) (fig.
1).
3) Acromial inferior protrusion (AIP).
It represents the distance from the most inferior point of the anterior acromion to the line coincident to the inferior aspect of the distal clavicle.
(fig.
1)
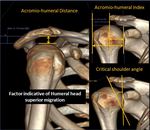
Factors indicative of Humeral head superior migration
4) Acromio-humeral distance (AHD).
AHD is defined as the distance between the most inferior aspect of the acromion and the most superior point of the humeral head (fig.
2).
Angles defining Lateral extension of the acromion
5) Acromiohumeral index (AI).
It measures the ratio of the distance form the glenoid plane to the lateral border of the acromion and the distance from same glenoid plane to the most lateral part of the proximal part of the humerus (fig.2).
6) Critical shoulder angle (CSA). First line was drawn from the most superior to the most inferior points of the gleniod cavity.
The second line from the most inferior points of the gleniod cavity to the lateral edge of the acromion.
The angle between the lines measured the critical shoulder angle.
(CSA) (fig.
2).
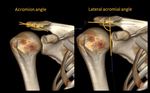
Angles defining acromion type
7) Acromion angle (AN).
First line was drawn across the midpoint of the posterior acromial slope,
another line was drawn across the midpoint of the anteiror acromial slope. The AN was measured as the angle formed by these two lines (fig.
3).
AN up to 15 degrees corresponded to type 1 acromion.
AN of 16 to 30 degrees to type 2 acromion,
whereas AN of more than 30 degrees was a type 3 acromion.
8) Lateral acromial angle (LAA).
First line was drawn along the most superior to the most inferior points of the gleniod cavity,
second line was drawn parallel to the acromion undersurface.
The angle between these lines represented lateral acromial angle.
Normal readings for this angle were within 64 and 99 degrees,
mean value was 78 degrees (fig.
3).
Rotator cuff tear verification methods were: MRT (43 patients) MR-arthography (8) or diagnostic arthroscopy (11).
Statistics were carried out using MedCalc Software (M.Tschopp&P.Pfiffner).
Descriptive statistics (mean value and standard deviation) were used for quantitative values.
Differences of the resultant radiography parametric values for the SIS patients and the control group,
as well RCT patients were evaluated using Student’s t-test.
Significance of the mean difference between the SIS and control groups was examined.
Significance level of p<0.05 was assumed to be significantly important.
Reproducibility of each parametric value was evaluated using intraclass correlation coefficient (ICC) with Cohen's Kappa statistics.