Keywords:
Oncology, Interventional non-vascular, Musculoskeletal bone, Percutaneous, CT, Ablation procedures
Authors:
I. A. Burovik, G. Prokhorov, A. V. Mishchenko; Saint Petersburg/RU
DOI:
10.26044/ecr2019/C-0408
Results
•Duration of hospitalization: 1 day
•Decrease in the index of the pain syndrome according to the McGill scale from the first day after the procedure (11 patients - partial pain relief, 6 patients - complete pain relief)
•Complications:
–slight disruption of sensation and a decrease in muscle strength in the peripheral regions in patient with tumor involving the sacral plexus
•0,5-1-year monitoring:
–10 patients- no local progression
–7 patient - local progression -> second procedure
Case 1.
•♀,
63 y.o.
•Ovarian cancer T3N0M1 (oss)
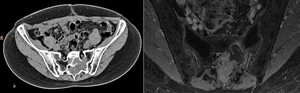
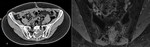
Fig. 3: Metastasis in sacrum of ovarian cancer
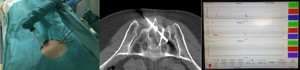
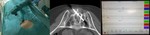
Fig. 4: Procedure of cryoablation. Two cryoprobes and one needle microthermocouple. Temperature control on the screen of cryotherapy system
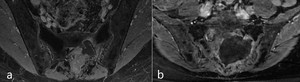
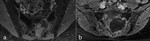
Fig. 5: MRI scans before (a) and in 6 months after cryoablation (b). On postoperative study (b) cystic cavity in the zone of the lesion with slight enhancement of the walls can be seen
While control biopsy in 6 months after procedure tumor cells were not detected.
Case 2.
• ♂,
62 y.o.
• Lung cancer T2N1M1 (oss)
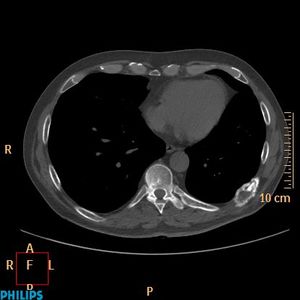
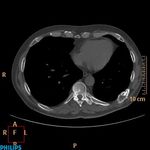
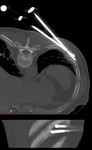
Fig. 6: Metastasis in the rib of lung cancer
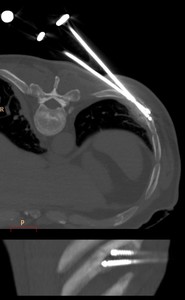
Fig. 7: Probe positioning while cryoablation
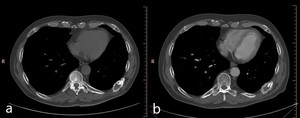
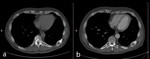
Fig. 8: Matastasis in the rib of lung cancer: before treatment (a) and in 8 months after cryoablation (b)
In 8 months after cryoablation no local progression was determined.