Evaluation of tumor staging according to MRI data in comparison with histopathological data
The results of preoperative MRI staging and postoperative pathology T-staging are presented in Table 1.
The discrepancy between the MR and pathological staging was noted by us in 16 cases out of 86.
An analysis of the discrepancy between the results is shown in Table 2.
There were following cases of overdiagnosis (reassessment of the stage) of the process according to MRI (see table 2):
· In one case,
on the pathomorphological data,
the Tis stage was registered – villus adenoma with intramucosal foci of adenocarcinoma; on MRI there were diagnosed polypoid lession of the lower ampullar rectus,
T2 st.
This case can be considered as a casuistry,
rarely observed in everyday practice; the recognition of the Tis stage lies outside the diagnostic capabilities of the MRI.
In its turn,
when visualizing polypoid lesion,
it is difficult to judge only on the basis of MRI data about the benign or malignant nature of a tumor.
Rather,
this case illustrates that the polypoid and infiltrative tumors of the rectum should be considered as stages of one process,
and preferably all polypoid formations are considered as potentially malignant.
· In five cases,
MRI overestimated the involvement of adjacent pelvic organs with fibrosis after neoadjuvant therapy,
pathomorphology excluded the invasion of adjacent organs (T4 stage lowered to T3).
This problem is often mentioned in similar studies and is mentioned in all similar studies we examined [5,6,
19-20].
Post-radiation fibrosis,
as a rule,
is present in patients with a primary verified T3 stage,
makes it difficult to determine the exact boundaries of the tumor process and pre-operative re-staging. A possible solution to this problem is the use of DWI with a sufficiently high b-factor [21,
22],
application of additional contrast series [4,
11],
as well as the use of additional to the standard protocol thin-cutting (1-2 mm) 3D T2-series [20].
Underestimation (hypodiagnosis) of the tumor stage:
· According to the MRI data,
we concluded T1 stage,
while pathomorphology revealed the focus of invasion in the muscle layer and T2 stage has been verified - 2 cases;
· The cT2 stage is verified as pT3a (pathologically verified spread beyond the intestinal wall by 1-2 mm) - 3 cases;
· The cT3 stage was considered in pathomorphology as pT4 (4 cases) - in patients after neoadjuvant CRT.
Difficulties in recognizing the T1-T2 stage are often mentioned in the literature,
especially in early studies based on 1.5 T MRT data [10,11].
Although most researchers do not notice significant differences in the sensitivity and specificity of the 1.5T and 3T MRI in the staging of rectal cancer,
for 3T MRI,
a higher sensitivity in the differentiation of the submucosal layer and the muscular wall was established,
and consequently,
recognition of the T1 and T2 stages of the process [20,
23,
24]. In our study,
for T1 and T2 stages,
sensitivity and specificity for the T1 stage,
100% and 97.5%,
respectively (table 3).
Sensitivity,
specificity and diagnostic accuracy [17,
18],
3T MRI for different T-stages of colorectal cancer obtained in our work are presented in Table 3.
Mistakes in the separation of T2 and T3a stages (limited spread beyond the limits of muscularis propria plate to mesorectal tissue) due to desmoplastic reaction and postradiation fibrosis,
are also often mentioned in publications,
constituting one of the main reasons for the decrease in the sensitivity and specificity of MRI for these stages of the process [4,6,
8,
11,
20].
In this case,
the sensitivity for the T3 stage in these sources varies from 71 to 83%,
and the specificity is 20-76%.
In our study,
the sensitivity and specificity for T3 was 87.1% and 92.1%,
respectively,
for the T2 stage – 81.3% and 94.5% (table 3).
Despite the generally recognized limitations of MRI in the separation of T2 and T3a,
a small clinical significance of this fact is noted,
due to the of the same therapeutic approach to these patients adopted in the most countries (a short neoadjuvant dose of radiotherapy and surgical intervention,
the type of which is determined by the tumor localization).
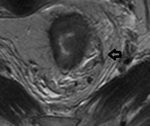
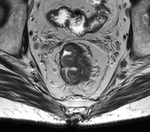
Extramural vascular invasion (EMVI)
EMVI was identified in 14 patients (16.2%) out of 86,
Fig.
1-2.
Estimated diagnostic accuracy for EMVI as compared with tumor endovascular emboli evidence on pathology was 93%.
8 (57%) of patients with pathology verified EMVI were diagnosed local T3 stage by MRI (with or without mesorectal fascia involvement).
5 (35,7%) were proved to have T4 stage.
Only one (7,3 %) – had no evidence of perirectal fat involvement.
Thus,
according to our data,
EMVI was diagnosed in 20,5% cases of MRI- evidence of local T3 stage (8 out of 39 cases).
During further short time follow –up (within two weeks after primary MRI),
distant liver metastases were detected in 6 out of 8 patients with EMVI and local T3 stage on MRI (75%).
To compare,
among the rest 31 patients with MRI proved local T3 without evidence of EMVI only 4 had distant metastases (12,9%).
Previously,
extramural vascular invasion was assessed only with a pathomorphological study [12].
Currently,
MRI makes it possible to clearly differentiate EMVI as a proven important risk factor for early recurrence,
tumor aggressiveness,
its sensitivity to neoadjuvant chemoradiotherapy [12,
13].
EMVI is associated with poor prognosis of the course of the disease and as a result - low overall survival of patients [12,
15- 16].
The sensitivity and specificity of MRI detection of EMVI reported by  Smith NJ et al.
in 94 patients undergoing primary surgery were 62 and 88 per cent respectively [12].
Thus,
MR-EMVI can be used as a potential biomarker that facilitates the choice of a method of treatment [12,13].
Sohn B et al.
showed that EMVI detected by MRI serves as an independent risk factor for the detection of distant synchronous metastases in a primary examination of the patients,
therewith the involvement of large vessels (more than 3 mm) is associated with a higher risk in comparison with small vessels (less than 3 mm in diameter) [13].
Similarly,
Barbaro B et al.
showed the relationship of EMVI and risk of synchronous metastases in patients with a non-mucinous form of adenocarcinoma [15].
Smith NJ et al.
in 94 patients undergoing primary surgery were 62 and 88 per cent respectively [12].
Thus,
MR-EMVI can be used as a potential biomarker that facilitates the choice of a method of treatment [12,13].
Sohn B et al.
showed that EMVI detected by MRI serves as an independent risk factor for the detection of distant synchronous metastases in a primary examination of the patients,
therewith the involvement of large vessels (more than 3 mm) is associated with a higher risk in comparison with small vessels (less than 3 mm in diameter) [13].
Similarly,
Barbaro B et al.
showed the relationship of EMVI and risk of synchronous metastases in patients with a non-mucinous form of adenocarcinoma [15].