Patients and CTp protocol
This study involved 46 patients enrolled in one Centre of the PIXEL project,
one of the widest European study aiming at identifying perfusion parameters (with a special focus on HPI) able to predict the development of liver metastases at colorectal cancer diagnosis.
Six patients developed liver metastases within the subsequent three-years.
All patients underwent an axial liver CTp study during which they were asked to breath slowly in order to reduce motion artefacts.
Contemporaneously with the beginning of CTp acquisitions,
an intravascular bolus of Contrast Agent (CA) was administered at a speed of 5ml/s,
concentration of 350mgI/ml,
followed by a 20ml-bolus of physiological solution.
CTp acquisition lasts for 2 min,
yielding 480 images,
referred to 60 CT scans (every 1 s for the first 30 s and every 3 s after) of 8-slices each (5mm thickness).
Hepatic perfusion model
The CA kinetics throughout the liver is represented by means of a dual-input one compartmental model,
thus allowing describing the two vascular pathways mainly supplying the organ,
the hepatic artery and the portal vein.
These are related by HPI,
the percentage of the arterial inflow with respect to the whole input (i.e.,
the sum of arteria and portal contributions).
Moreover,
this single-compartmental model adopted by this work represents both the intra- and extra-vascular spaces for carrying out perfusion analyses in the first-pass phase of CA.
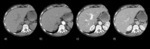
Fig.
1 shows the baseline,
arterial,
portal,
and delayed phases of CA kinetics,
respectively in a),
b),
c),
d),
captured by the CTp images.
Fig.
2 shows the dual-input one-compartmental model such as that used in this work.
By considering the model as a linear dynamic system,
inputs and output are related by means of the convolution of the inputs with the Impulse Residue Function (IRF) of the system,
representing the quantity of CA remaining into the tissue over time.
Data preparation and perfusion analyses
For each CTp examination a central slice is selected,
and two ROIs are first drawn on the aorta and tissue.
Then,
a ROI outlined the portal vein and was aligned over time in order to compensate for motion.
TCCs are recovered from the aorta and portal vein,
by averaging the contribution of all voxels,
while voxel-based TCCs are extracted from the tissue ROI.
An anisotropic edge-preserving spatial filter is exploited for noise reduction and an early non-parametric fitting is performed just to up-sample the TCCs and achieve a uniform frequency of 1Hz.
After baseline removal,
the corresponding Time Attenuation Curves (TACs) are pre-processed,
thus becoming ready for perfusion analyses.
As regards the vascular inputs,
Ca(t) and Cp(t) respectively,
the Lagged Normal function [8] is applied in order to fit the TACs and exclude the recirculation phase of CA.
Instead,
tissue TACs are fitted through the Gamma-Variate model [9].
Perfusion analyses were carried out by means of an in-house perfusion software implementing the deconvolution model,
thus recovering the IRF of the system and providing us with voxel-based estimates of the HPI.
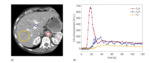
Fig.
3(a) reports all the ROIs outlined on a reference slice of the CTp study,
Fig.
3(b) shows the corresponding median TACs extracted from the ROIs.
Feature selection and discrimination process
Our perfusion software permits the computation of 6 hepatic perfusion parameters,
Blood Flow (BF),
Blood Volume (BV),
Mean Transit Time (MTT),
HPI,
Time to Peak (TTP),
Wash-in Time (WiT).
In the following,
these parameters are summarized,
with the help of a graphical representation shown in Fig.
6 to highlight the signals descriptors belonging to the IRF for the computation of BF,
BV,
and MTT and to the tissue TAC,
as regards TPP and WiT.
- BF,
measured in [ml/min/100g],
is the concentration of blood transported to a unit volume of tissue volume per unit of time.
- BV, measured in [ml/100g],
is the volume of blood flowing in the tissue.
- MTT, measured in [s],
is the average transit time of the blood throughout the tissue vascular network.
According to the Central Volume Theorem (CVT)[10],
MTT is related to BF and BV by means of the following Eq.
(1) in Fig.
4:
- HPI,
is a percentage weight of the arterial BF (ABF) over the total BF (the sum of both arterial and portal (PBF) contributions),
as expressed by Eq.
(2) in Fig.
5:
- TTP, expressed in [s] is the time instant when the maximum value of tissue TAC occurs
- WiT,
expressed in [s] is the time instant when the derivative of the tissue TAC reaches its maximum value
On each of these parameters,
mean,
median,
skewness (skewn) and kurtosis (kurt) are computed for a total amount of 24 different features.
Then,
all possible couples (276 combinations) of the features are considered in order to discriminate patients developing liver metastases.
Assessment of results
The 276 couples of features were analyses to look for linear separations of patients who will develop liver metastases.
The discrimination process is performed to identifying the features showing the maximum specificity (100%),
thus neglecting sensibility measurements due to the reduced amount of metastases over the total number of patients.
In addition,
the metastases are ranked based on the frequency they can be linearly separated by the selected 23 couples of features.
The skewness is measured in arbitrary units (a.u.).