In this work the key imaging findings of our false negative and false positive outcomes are revised.
False Negative Findings:
Of the 296 patients,
123 (42%) were allocated PIRADS 1 or 2 on MRI.
We reviewed these cases to identify patients subsequently shown to have cancer on biopsy.
A total of 15 patients were identified,
6 of which had Gleason 3+3 cancer which is not deemed clinically significant by PROMIS criteria.
The remaining 9 patients had at least Gleason 3+4 disease,
clinically significant prostate cancer and therefore classed as true false negatives.
We demonstrate a true false negative rate of 7% (n=9) in keeping with 7% in the PROMIS trial3.
These false negative cases were retrospectively reviewed.
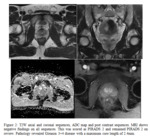
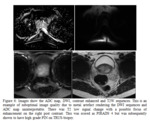
Five patients remained as PIRADS 1 or 2 (See example in figure 2).
Four patients had their PIRADS score upgraded on retrospective review.
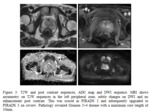
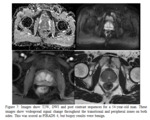
One was upgraded to PIRADS 3 (See figure 3),
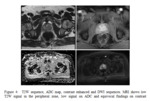
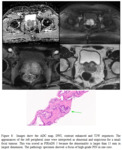
one to PIRADS 4 (See figure 4) and 2 were upgraded to PIRADS 3 or 4.
Using the definitions from the PROMIS trial,
3 of 9 patients had primary definition clinically significant disease (Gleason score 4+3 or cancer core length 6mm) and 2 of these had their PIRADS score upgraded on review.
False Positive Findings:
77 patients (26%) were scored as PIRADS 4 or 5.
95% (n=73) of these patients had a biopsy,
with cancer detected in 77% (n=56).
Therefore,
23% (n=17) had no cancer detected on biopsy despite highly suspicious findings on MRI.
These 17 cases were classed as false positive findings.
The pathology results these 17 cases showed the following:
We reviewed these 17 cases to identify the causes of these discrepant results to provide learning opportunity and improvement in clinical accuracy for future reporting.
There were 8 main learning points/pitfalls that we identified as causes of false positive results in our study and these are presented below.
Inflammation
Prostatitis,
or inflammation of the prostate gland,
is a common finding in men and appearances on MRI can mimic malignancy4.
Figure 5 shows an example of a MP-MRI that was scored PIRADS 5 which was subsequently shown to be prominent inflammation.
The prostate appearances demonstrated widespread,
diffuse changes with widespread enhancement.
We had 4 similar cases.
Clinical correlation and PSA dynamics can be invaluable in such cases it there is ambiguity about the diagnosis.
Artefact:
Artefact for example from a hip prosthesis can degrade image quality and often hinder accurate interpretation of the images.
In figure 6 metal artefact degraded the quality of the DWI/ADC sequences which could subsequently not be accurately interpreted.
When artefact impacts the image quality,
reporting confidence should be reduced,
and it may be prudent to proceed with biopsy if any uncertainty remains.
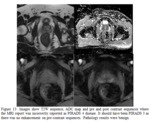
Patient age:
The MRI appearances of the prostate gland in younger patients (typically 50-60 years) can differ from older men as the prostate architecture changes with age5.
Figure 7 demonstrated the prostate appearances of a 54-year-old man in our study.
It shows diffuse T2,
ADC and enhancement changes which were misinterpreted as malignant change.
High grade PIN:
High grade PIN is considered a precursor of prostatic malignancy6.
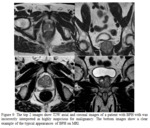
It manifests as cellular proliferation with cytologic changes that mimic cancer including nuclear and nucleolar enlargement6. Figure 8 is an example of a case that was scored as PIRADS 5 and was subsequently shown to have high grade PIN on biopsy.
There was no arterial enhancement,
so it should not have been scored PIRADS 5.
In our study,
on MP-MRI,
high grade PIN did not show arterial enhancement.
Benign prostatic hypertrophy (BPH):
BPH is the formation of encapsulated nodules in the transition zone and its prevalence increases with age7.
Often BPH can pose a diagnostic challenge as extruded BPH pushing out from the transitional zone to the peripheral zone can show low T2W signal intensity and low ADC which can be confused with malignancy7.
However,
BPH tends to be well defined and well circumscribed compared to malignancy7.
Use of all reconstructed planes can also aid accurate interpretation in this benign finding7.
We identified 2 cases where extruded BPH pushing out into the peripheral zone was misinterpreted as suspicious for malignancy on PIRADS scoring.
Figure 9 shows one such example.
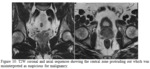
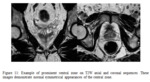
Central zone:
Figure 10 shows an example of where appearances of the central zone were incorrectly interpreted as malignancy.
The normal central zone should appear homogeneously hypointense on T2W sequences and low signal on ADC maps8.
Appearances of the central zone of the prostate can mimic malignancy.
Looking for a bilateral and symmetrical appearance of the central zone is key to avoiding this pitfall8 (See figure 11).
Also,
it is important to use coronal images for correlation.
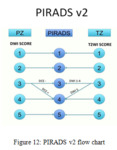
Incorrect use of PIRADS:
Knowledge of the PIRADS scoring system and its correct implementation is essential to ensure accurate reporting and interpretation of the images (See figure 12).
Figure 13 highlights a case where incorrect interpretation of the PIRADS scoring system led to PIRADS 3 disease being reported as PIRADS 4.
We identified 2 discrepant cases that resulted from incorrect use of the PIRADS scoring system.
From these cases,
we highlight the following points as important learning points as lack of proper understanding of these concepts led to errors in reporting in the case demonstrated below:
-
The need to demonstrate enhancement to change from PIRADS 3 to PIRADS 4,
-
The use of T2W sequences as the dominant scan for assessing the peripheral zone,
-
The use of Diffusion Weighted Imaging (DWI) and the ADC map as the dominant sequences for assessing the peripheral zone.
Biopsy method:
The location of the lesion can affect the accuracy of biopsy results.
For example,
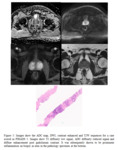
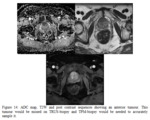
apical lesions are often missed on TRUS-biopsy and TPM-biopsy is needed to ensure the lesion is accurately targeted (See Figure 14).
We had one patient where the TRUS biopsy was benign but the subsequent TPM-biopsy was suspicious for malignancy.
If the TPM-biopsies results subsequently differ from the TRUS results,
close follow up is needed.