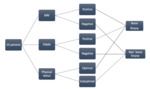
In our prospective pilot single center study we included 10 consecutive mCRPC patients with a suspicion of bone metastases on imaging.
The study was conducted in the Radboud Medical University (Nijmegen,
Netherlands) from February 2018 untill August 2018.
All patients had a full clinical examination,
MRI of the pelvic bone and lumbar spine,
PSMA-PET/CT,
and cone beam CT-guided bone biopsy.
Study inclusion and exclusion criteria are represented in Fig.1.
Our study was approved by the local ethical committee and all patients were informed about research details and signed the informed consent.
Clinical data collection
All patient data was anonymized and added to a CASTOR database.
The data included age,
prior treatments and laboratory parameters.
All MRI and PET/CT examinations were performed within 2 weeks before the bone biopsy.
MRI
MRI was performed on a 3.0T MRI scanner (Magnetom Prisma Siemens MRI was performed on a 3.0T MRI scanner (Magnetom Prisma Siemens Healthineers,
Erlangen,
Germany),
using surface body.
The study protocol included T1-dixon weighted imaging (WI) (T1 WI in and out phase,
fat and water maps) in the coronal plane and reconstructed imaging in the axial plane; T2 STIR (short tau inversion recovery) in the sagittal plane.
The DWI was performed in the coronal plane using multiple b-values: 0,
25,
50,
75,
100,
200,
400,
800 s/mm2.
Imaging analysis
Images were processed and analyzed with open-access imaging assistant software (Horos v3.0.1,Horosproject.org) by a single radiologist.
The process of imaging analysis in each patient included:
1) Calculation of intravoxel incoherent motion diffusion fraction (IVIM D) images were performed using Horos plug-in - IB Diffusion (Imaging Biometrics).
2) Calculation of intravoxel incoherent motion perfusion fraction (IVIM F) images were performed using Horos plug-in - IB Diffusion (Imaging Biometrics).
3) Calculation of ADC maps.
4) Fat (FF) and water (WF) fractions were calculated using an in-house Horos plug-in (FF = 100%/ Sfat/(Sfat + Swater); WF=100%/ Swater/(Sfat + Swater),
where S indicates signal at every voxel location).
Pre-biopsy sequences were co-registered using the Horos Insight Segmentation and Registration Toolkit.
The regions of interest (ROIs) were copied to the ADC,
FF and WF (Dixon-imaging),
and IVIM D and IVIM F images.
Target bone lesion (TBL),
non-target lesion (NTL) and non-metastatic bone (NMB) were annotated on MRI.
The NTL was positive on PSMA-PET/CT and MRI but was not biopsied.
In these annotated areas we calculated FF,
WF,
IVIM D and IVIM F.
Cone beam CT-guided bone biopsy
All patients underwent a cone beam CT (CBCT)-guided bone biopsy.
The CBCT scanner (Artis Zeego,
Siemens Healthineers,
Forchheim,
Germany) acquires projection images during isocentric rotation of a C-arm,
which are then reconstructed to a 3D volume.
Only the TBL was biopsied.
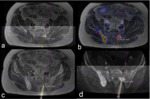
Target planning was done on a fusion of 68Ga-PSMA-PET/CT and MRI images (Fig.
2). All biopsies were performed by one interventional radiologist with more than 15 years of experience.