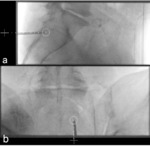
Ten bone biopsies were performed on 10 patients (median age 64 years; range 57–71years).
Nine (90%) of these 10 biopsies were representative and positive for tumor cells.
One biopsy (10%) was representative and negative for tumor cells.
However,
we should note that this lesion was PSMA positive and DWI/ADC negative (in the other cases all lesions were PSMA and DWI/ADC positive).
Less fat component was found in metastatic bone lesions in comparison with normal bone: median of the FF in positive bone biopsies was 14%; in normal bone - 71% (P < 0.05).
The median FF in TBL and NTL was compared: median FF in TBL was 14%; in NTL 20% (p=0.028) (Fig.3).
Accordingly the WF was significantly higher in TBL and NTL (76% and 80%),
thus in metastatic bone lesions,
compared to NMB (29%),
p<0.05 (Fig.4).
In addition,
we calculated and compared IVIM parameters (D and F fractions) in each patient.
Median IVIM D in target lesion was 0.615 х10−3mm2/s (min and max value,
0.5–0.78 х10−3mm2/s) and in non-metastatic bone this was 0.335 х10−3mm2/s (min and max value,
0.22–0.7 х10−3mm2/s) (P=0.005).
There were no statistical differences between target and non-target lesions: 0.615 х10−3mm2/s (min and max value,
0.5–0.78 х10−3mm2/s) and 0.604 х10−3mm2/s (min and max value,
0.41–0.78 х10−3mm2/s)respectively (p = 0.95) (Fig.5).
The median relative perfusion fraction (IVIM F) for the target lesions,
non-target lesion and normal bones were 6%; 7%; and 4% respectively and did not have any statistically significant differences (P>0.05).
It should be taken under consideration that the calculated IVIM F images were very noisy and had a very low signal intensity in all bone lesions.
Discussion
The growth of a malignant lesion in normal bone results in replacement of the bone marrow fat cells by tumor cells and reduction of marrow fat fraction [8].
This phenomenon could be used as one of the response criteria in the treatment of mCRPC,
assuming successful therapy causes normal bone marrow fat to return.
In our study we had statistically significant differences in fat component between the target malignant lesion and normal bone marrow.
Also,
we identified that the target bone lesion had a significantly lower fat fraction compared to a non-target lesion (p=0.028) which could be explained by an increasing replacement of fat for a water component.
This could indicate that target lesions were more aggressive than non-target lesions,
but that should be confirmed by advanced histopathological analysis.
In our study we found much or significantly higher IVIM D values in bone metastases than in normal bone,
which can be explained by a higher molecular metabolic activity.
Potentially,
this fact could be used as diagnostic criterium for monitoring the post-treatment response.
We investigated the diagnostic efficacy of IVIM F imaging and statistically significant differences between malignant and non-malignant bone were not found in our study.
In most cases the images were very noisy and had a very low signal intensity with a high standard deviation. This could probably be explained by the low perfusion in a bone lesion but more detailed analysis is needed.
The strength of this study was the controlled biopsy procedure.
The target was planned on PSMA-PET/CT and MRI,
and through image fusion this target was available during CBCT-guidance (Fig.
6).
Most target bone biopsies were positive (90%) and yielded material suitable for histological and molecular analyses.
Therefore imaging and histology parameters are directly comparable.
The molecular imaging shown on this poster will be compared to more advanced histology parameters in the next part of this study.