Type:
Educational Exhibit
Keywords:
Extremities, Lymph nodes, Interventional vascular, Conventional radiography, Fluoroscopy, CT, Embolisation, Ablation procedures, Technical aspects, Fistula, Outcomes, Trauma
Authors:
C. M. Sommer1, F. Offensperger1, A. Hatopp1, C. Goerig1, J. Hornung1, T. Hupp1, J. Köninger1, H. U. Kauczor2, G. M. Richter1; 1Stuttgart/DE, 2Heidelberg/DE
DOI:
10.26044/ecr2019/C-0660
Findings and procedure details
Transpedal lymphangiography:
Transpedal lymphangiography applying iodized oil as contrast and occlusion material and radiography and CT as imaging modalities is the first-line approach to visualize type (e.g.
lymphopseudoaneurysm or lymphocele),
degree (e.g.
unifocal or multifocal) and exact location (e.g.
efferent to lymph nodes) of post-operative therapy-refractory lymphatic fistula in the groin region.
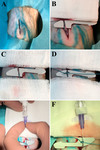
The major steps of transpedal lymphangiography - including preparation,
cut-down and iodized oil application - is presented in Figures 2 and 3.
In a considerable number of patients,
transpedal lymphangiography alone is a curative treatment due to blockage of afferent lymph ducts and sterile inflammation processes with subsequent scarring in the location of the pathological iodized oil extravasation (Figures 4-7). According to our clinical experience with more than 500 transpedal lymphangiographies during the last 25 years, cure of lymphatic fistula located at or below the level of the inguinal ligament can be expected after single or repetitive transpedal lymphangiography in approximately 50% of patients within some days or few weeks.
Thereby,
technical success and procedure-related complication rates are approximatelly 90% and <0.5%,
respectively.
After transpedal lymphangiography,
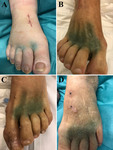
patent blue at the injection site undergoes resorption within different intervals (Figure 8).
Percutaneous lymphatic second-line interventions:
In case of clinical failure after transpedal lymphangiography,
which should be confirmed not earlier than 2 weeks after transpedal lymphangiography,
percutaneous lymphatic second-line interventions are indicated.
Depending on type,
degree and exact location of the lymphatic fistula,
fluoroscopy-,
ultrasound- and/or CT- or cone-beam CT-guided sclerotherapy or embolization of afferent lymph ducts,
lymph nodes,
pathologic iodized oil extravasation,
and/or the lymphopseudoaneurysm (e.g.
applying ethanol 95% and/or histoacryl/iodized oil mixtures in different ratios) can be performed safely and effectively.
In a substantial number of patients,
these different percutaneous lymphatic second-line interventions can be performed without repeated transpedal lymphangiography (Figures 9 and 10).
Alternatively,
different percutaneous lymphatic second-line interventions can be combined with transpedal lymphangiography in a one-stage procedure with the intention to accelerate cure of the lymphatic fistula (Figure 11-13).
According to our current clinical experience,
percutaneous lymphatic second-line interventions increase the clinical success rate of transpedal lymphangiography alone by >25%.
Additionally,
the cure of lymphatic fistula after percutaneous lymphatic second-line interventions can be expected in less time compared with transpedal lymphangiography alone.

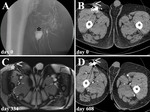
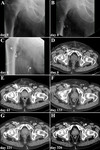
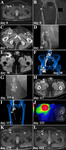
![Fig. 9: SCLEROTHERAPY APPLYING ETHANOL – TWO-STAGE PROCEDURE
Lymphatic fistula after inguinal melanoma resection with lymphadenectomy:
(A) diagnostic sentinel lymphoscintigraphy, (B) transpedal lymphangiography (16th postoperative day; 16 ml iodized oil) demonstrating an unifocal iodized oil extravasation (lymphopseudoaneurysm, white asterisk), (C) dual-energy CT lymphangiography confirming the pathologic iodized oil extravasation (lymphopseudoaneurysm white arrowhead), (D) X-ray control 22 days after transpedal lymphangiography (indicated due to persistant [but decreased] lymphatic drainage volume) demonstrating constant iodized oil distribution within the lymphatic fistula (lymphopseudoaneurysm) and in afferent lymph ducts, (E) CT-guided puncture (21 G cannula) and sclerotherapy (3 ml ethanol 95% [after simulation of ethanol 95% distribution applying a test injection with contrast material) of afferent lymph ducts, (F) ultrasound control 7 days after CT-guided sclerotherapy demonstrating a lymphocele after removal of the drainage catheter, (G) ultrasound control 10 days later and after draining of the lymphocele demonstrating only minimal persistance of the lymphocele, and (H) cure of lymphatic fistula and lymphocele (white asterisk) during follow-up (PET-CT).](https://epos.myesr.org/posterimage/esr/ecr2019/149643/media/797522?maxheight=150&maxwidth=150)
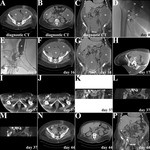
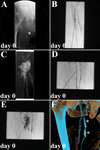
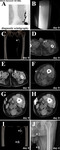
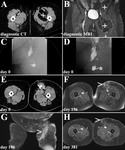
![Fig. 13: EMBOLIZATION AND SCLEROTHERAPY APPLYING GLUE AND ETHANOL – COMBINED WITH TRANSPEDAL LYMPHANGIOGRAPHY IN A ONE-STAGE PROCEDURE
Lymphatic fistula after inguinal hernia repair and lymphadenectomy:
(A) and (B) transpedal lymphangiography (>30th postoperative day; 18 ml iodized oil) demonstrating a complex iodized oil extravasation (lymphopseudoaneurysm, white asterisks; sponge [negative pressure wound therapy], white arrowhead), (C) (D), (E), (F) and (G) CT lymphangiography confirming the pathologic iodized oil extravasation (D and G, lymphopseudoaneurysm white arrowhead) and severe wound healing disorder (C and G, sponge, white arrowhead) as well as a prominent afferent lymph node (E and G, white arrowhead) and multiple afferent lymph ducts (F and G, white arrowhead), (H), (I), (J) and (K) fluoroscopy-guided puncture (I, 21 G Chiba needle) and embolization of the lymphopseudoaneurysm (J, 4 ml glue/iodized oil 1:3 mixture) as well as fluoroscopy-guided puncture (K, 25 G spinal needle, under 3D embolization guidance after image fusion) and embolization of the prominent afferent lymph node (K, 2 ml glue/iodized oil 1:7 mixture), (H) and (L) fluoroscopy-guided puncture (L, 21 G cannula, under 3D embolization guidance after image fusion) and sclerotherapy of the afferent lymph ducts (L, 3 ml ethanol 95% [after simulation of ethanol 95% distribution applying a test injection with contrast material]), and (M), (N), (O) and (P) cone-beam CT lymphangiography demonstrating adequate glue/iodized distribution (M and P, lymphopseudoaneurysm; N and P, prominent afferent lymph node) and ethanol (contrast material) distribution (O and P). ANNOTATION: In the further course after step-by-step downsizing of the sponge and finally secondary wound closure, unremarkable wound healing and evidence of only minimal and temporal lymph edema of the leg.](https://epos.myesr.org/posterimage/esr/ecr2019/149643/media/797544?maxheight=150&maxwidth=150)
