In this presentation,
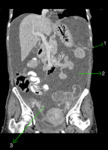
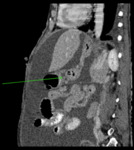
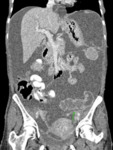
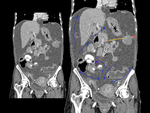
CECT images of a 53 year old lady who is a known case of Neurofibromatosis with complaints of abdominal distension and on imaging found to have gross ascites and bilateral adnexal lesions are used for demonstration of anatomy of peritoneal spaces and reflections.
Other cases for illustration of various pathological processes involving peritoneum with emphasis on route of spread will follow after review of anatomy.
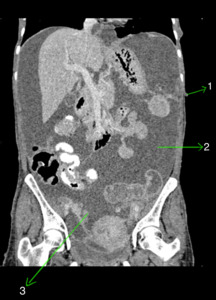
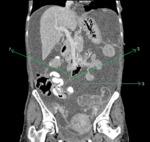
Fig. 4: Coronal CECT abdomen showing gross ascitis (2) and adnexal lesions (3) in a patient with neurofibromatosis. A small cutaneous neurofibroma is seen in abdominal wall (1).
Peritoneal ligaments
Suspensory ligaments of liver
Include the triangular and falciform ligaments.
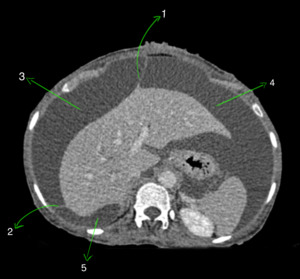
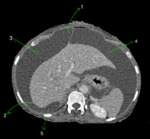
Fig. 5: Axial CECT abdomen showing peritoneal ligaments of liver - falciform ligament (1) separating right subphrenic space (3) and left subphrenic space (4). Right triangular ligament (2) is also seen separating right subphrenic space (3) and right sub hepatic space (5).
Triangular Ligaments
Outline the bare area of liver. The left triangular ligament is formed by fusion of inferior and superior reflections of left coronary ligaments. It is short and does not compartmentalize the left subphrenic space.
The right triangular ligament is formed by fusion of superior and inferior reflections of the right coronary ligament. It is long and separates the right subphrenic space from the right subhepatic space.
Falciform Ligament
Remnant of the most ventral part of ventral mesentery.
Falciform ligament contains the obliterated umbilical vein.
It acts as a relative (incomplete) barrier to transfer of fluid from the right subphrenic space to the left.
Subperitoneal tumor spread in the falciform ligament may mimic liver metastasis. Recanalized paraumbilical vein is also found in the falciform ligament.
Peritoneal Ligaments of the Stomach
Include Lesser omentum, Gastrosplenic ligament, Greater omentum and Splenorenal ligament.
Lesser Omentum
Remnant of the dorsal portion of ventral mesentery.
The gastrohepatic and hepatoduodenal ligaments form the lesser omentum.
The gastrohepatic ligament attaches the lesser curvature of stomach to the liver and contains the coronary vein and left gastric artery. The hepatoduodenal ligament attaches the duodenum to liver and contains the portal vein,
hepatic artery,
common hepatic ducts and part of cystic duct.
It acts as route of spread of pancreatic disease to the porta hepatis and liver.
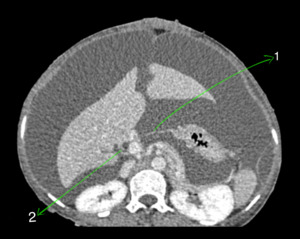
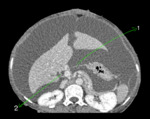
Fig. 6: Axial CECT abdomen showing the two components of lesser omentum - Gastrohepatic (1) and Hepatoduodenal (2) ligaments.
Gastrosplenic Ligament
The ventral part of dorsal mesentery extends between the greater curve of stomach and the spleen.
It contains the short gastric vessels and a collateral route of venous flow after splenic vein thrombosis.
It acts as a frequent route for subperitoneal spread of pancreatitis-related fluid,
especially from peripheral body and tail of pancreas.
Fluid within the gastrosplenic ligament is often mistaken for a lesser sac collection,
but do not communicate with the peritoneal cavity.
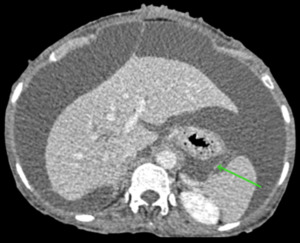
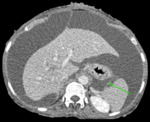
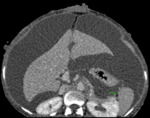
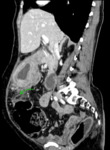
Fig. 7: Axial CECT abdomen showing the gastrosplenic ligament (green arrow).
Greater Omentum
It is also called the gastrocolic ligament.
The greater omentum may become visible if it is diseased or if ascites is present.
It is used to surgically move radiosensitive bowel out of a pelvic radiation field.
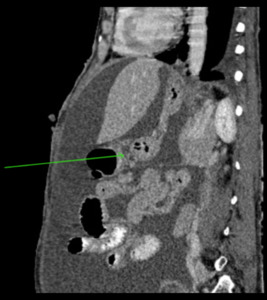
Fig. 8: Sagittal CECT abdomen showing gastrocolic ligament (green arrow).
Splenorenal Ligament
It is formed from the most dorsal aspect of dorsal mesentery.
It contains the pancreatic tail and splenorenal collateral vessels in patients with portal hypertension.
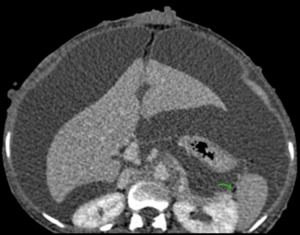
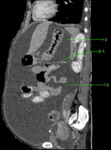
Fig. 9: Axial CECT abdomen showing splenorenal ligament (green arrow).
Transverse Mesocolon
Transverse mesocolon is the peritoneal fold that attaches the transverse colon to the retroperitoneum.
It contains the middle colic vessels.
In patients with pancreatic head cancer,
it is an important possible source of local extension.
Because of its numerous vessels,
vascular control is difficult and extension into mesocolon renders pancreatic cancer inoperable. The transverse mesocolon also may be a route for internal herniation after retrocolic Roux-en-Y gastric bypass surgery.
Gastric ulcers may involve transverse mesocolon to create Gastrocolic fistulas.
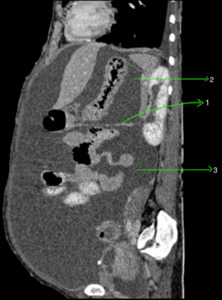
Fig. 10: Sagittal CECT abdomen showing transverse mesocolon (1) dividing peritoneal cavity into supramesocolic (2) and inframesocolic spaces (3).
Small Bowel Mesentery
Small bowel mesentery attaches the small bowel to retroperitoneum.
It extends from the ligament of Treitz to ileocecal valve.
It contains the superior mesenteric vessels and their branches.
Inflammation and tumor may involve the mesentery directly (eg,
from the pancreatic body or jejunum) or by way of the neurovascular plexus or lymphatic channels that run within it.
Rotational and fusion anomalies of the mesentery may lead to volvulus or internal hernia.
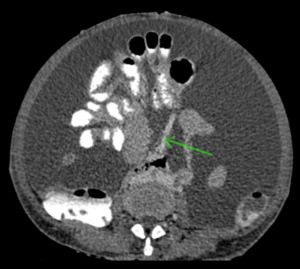
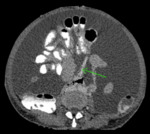
Fig. 11: Axial CECT abdomen showing small bowel mesentery (green arrow).
Sigmoid Mesocolon
Sigmoid mesocolon is the peritoneal ligament that attaches the sigmoid colon to the posterior pelvic wall.
It contains the hemorrhoidal and sigmoid vessels.
The most common pathologic process involving this structure is acute diverticulitis.
Perforated cancer and Crohn disease also may cause inflammation within the sigmoid mesocolon.
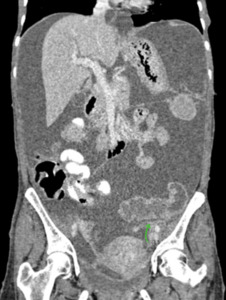
Fig. 12: Coronal CECT abdomen showing sigmoid mesocolon (green arrow).
Peritoneal Spaces
Transverse mesocolon divides the peritoneum into supramesocolic and inframesocolic spaces. Bilateral paracolic and pelvic spaces are also peritoneal spaces.
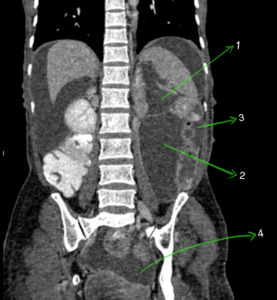
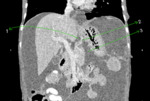
Fig. 13: Coronal CECT abdomen showing various peritoneal spaces - Supramesocolic space (1), inframesocolic space (2), paracolic (3) and pelvic spaces (4).
Left Supramesocolic Spaces
Include the left subphrenic and perisplenic spaces. The phrenicocolic ligament is a relative but incomplete impediment to the spread of pathologic processes from the left paracolic gutter to left subphrenic space.
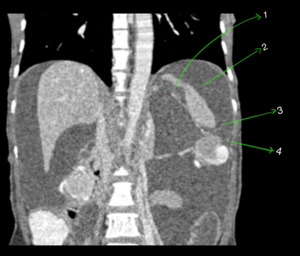
Fig. 14: Coronal CECT abdomen showing left supramesocolic space- Left subphrenic space (2) and perisplenic space (1). Left subphrenic space (2) is separated from left paracolic space (4) by the phrenicocolic ligament (3).
Right Supramesocolic Spaces
Include the right subphrenic space,
Morison pouch (subhepatic or hepatorenal space) and lesser sac (omental bursa) (fig.5).
The right subphrenic space is separated from the left by falciform ligament which serves as an incomplete barrier to the spread of disease. The right subhepatic space is an important site of fluid collections resulting from liver injuries because it is the most gravity-dependent space at this site.
Lesser sac
Contains a superior recess and inferior recess separated by a peritoneal fold that accompanies the left gastric artery. Superior recess is a boomerang-shaped recess that is in close proximity to the caudate lobe.
The inferior recess is larger and lies between the stomach and pancreatic body.
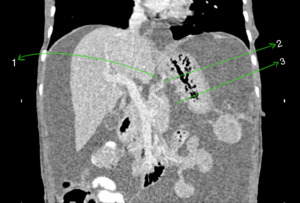
Fig. 15: Coronal CECT abdomen showing the two recesses of lesser sac, the superior recess (1) and inferior recess (3) being separated by the peritoneal fold containing left gastric artery (2).
Foramen of Winslow
On the right side,
the inferior recess communicates with the subhepatic space through the foramen of Winslow.
Thus,
it is possible for bowel to herniate into lesser sac through the foramen of Winslow.
It is bounded anteriorly by the hepatoduodenal ligament,
posteriorly by inferior vena cava, superiorly by caudate lobe and inferiorly by the duodenum and hepatic artery.
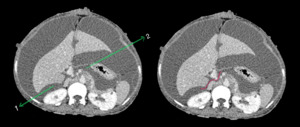
Fig. 16: Axial CECT abdomen showing Foramen of Winslow (curved red line) which is the route of communication between right subhepatic space (1) and inferior recess of lesser sac (2).
Right and Left Inframesocolic Spaces
The right and left inframesocolic spaces are separated from the supramesocolic spaces by the transverse mesocolon and from the paracolic gutters laterally by the ascending and descending colon.
The smaller right inframesocolic space is limited inferiorly by the attachment of small bowel mesentery to cecum; collections in this space generally do not extend into pelvis.
However,
the larger left inframesocolic space communicates freely with the pelvis.
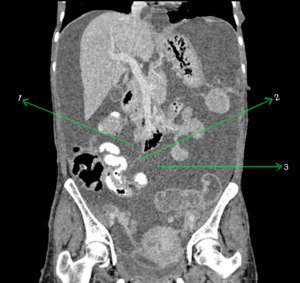
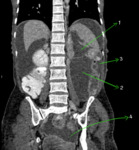
Fig. 17: Coronal CECT abdomen showing the inframesocolic spaces. The smaller right inframesocolic space (1) being limited inferiorly by the attachment of root of mesentery (2) to caecum and the larger left inframesocolic space (3) communicating freely with the pelvis.
Paracolic Spaces
The paracolic spaces (gutters) are located lateral to peritoneal reflections of left and right sides of colon.
The right paracolic gutter is larger than the left and communicates freely with the right subphrenic space. The connection between the left paracolic gutter and left subphrenic space is partially limited by the phrenicocolic ligament. Both the right and left paracolic gutters
communicate with the pelvic spaces.
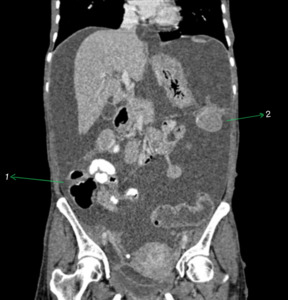
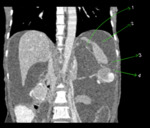
Fig. 18: Coronal CECT abdomen showing the right paracolic space (1) in the lateral aspect of ascending colon and left paracolic space (2) in the lateral aspect of descending colon.
Pelvic Spaces
In men,
the most gravity-dependent site for fluid accumulation is the rectovesical space and in women,
it is the retrouterine space (Pouch of Douglas).
Anteriorly,
the medial umbilical folds,
which contain the obliterated umbilical arteries,
divide the pelvic spaces into lateral and medial compartments.
On each side,
the inferior epigastric artery divides the lateral pelvic compartments into lateral and medial inguinal fossae,
the sites of direct and indirect inguinal hernias respectively.
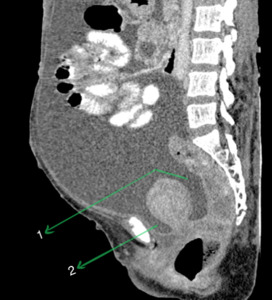
Fig. 19: Sagittal CECT abdomen showing the rectouterine pouch (1) and vesicouterine pouch (2).
ROUTE OF SPREAD
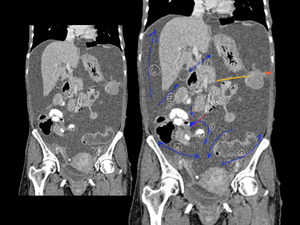
Fig. 20: Schematic representation of route of spread
Fluid in the right inframesocolic space (1) cascades down the leaves of the small bowel mesentery (red line) pools at the medial aspect of the cecum,
and then overflows into the pelvis (2).
Fluid in the left inframesocolic space (3) seeks the pelvis directly.
Fluid in the pelvis may ascend the left paracolic gutter (5) but is stopped by the phrenicocolic ligament (orange line).
Fluid in the right paracolic gutter (4) ascends to the Morison pouch (7) and then to the subphrenic space (6),
where it is stopped by the bare area of the liver.
There is potential communication with the lesser sac through the foramen of Winslow (8).
Yellow line is transverse mesocolon.
Pathologies involving solid organs/ viscus can extend to adjacent structures along the peritoneal ligaments and spaces as illustrated by the following examples.
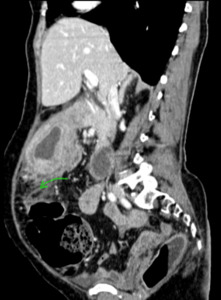
Fig. 21: Sagittal CECT abdomen of a 60 year old female showing spread of gastric lymphoma along the gastrocolic ligament (green arrow).
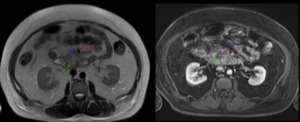
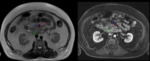
Fig. 22: Axial MR abdomen of a 52 year old male, T2Wi and post contrast T1Wi showing carcinoma uncinate process of pancreas (green arrow) infiltrating into mesentery with invasion of superior mesenteric vein (blue arrow). Red arrow is superior mesenteric artery.
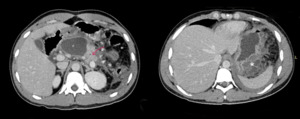
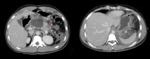
Fig. 23: Middle aged male with acute on chronic pancreatitis. CECT abdomen axial sections shows inflamed pancreas (red arrow) with a walled off necrosis (P) in head and body. Cranial section of same patient shows fluid collection and inflammation extending to gastrosplenic ligament (asterix).
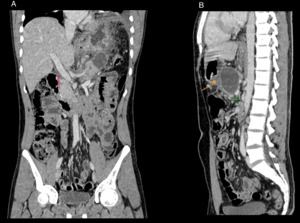
Fig. 24: Coronal (A) and sagittal (B) images of the same patient. In A, red arrow shows rim of hypodensity surrounding portal vein suggestive of spread of inflammation along hepatoduodenal ligament. In B, yellow and green arrows indicate inflammation extending to lesser sac and transverse mesocolon respectively.
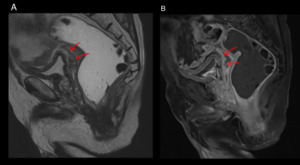
Fig. 25: Elderly male who is a known case of carcinoma head of pancreas. Sagittal T2 Wi (A) and post contrast T1 Wi (B) images show necrotic deposit in rectovesical pouch (red arrows), which is the most dependent peritoneal space in men.