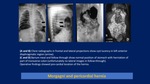
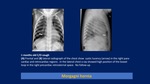
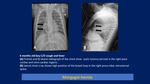
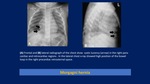
Prenatal diagnosis of Bochdalek and Morgagni hernia:
Ultrasound:
Using ultrasonography,
congenital diaphragmatic hernia (CDH) may be prenatally diagnosed as early as the second trimester.
ultrasound detects more than 50% of CDH cases at a mean gestational age of 24 weeks.
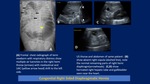
The definitive sonographic diagnosis of fetal CDH relies on the visualization of abdominal organs in the fetal chest.
Left-sided CDH is characterized by the presence of a heterogeneous lesion (small bowel) in the left chest that often results in right mediastinal shift.
Fluid and peristalsis in the heterogeneous mass help to distinguish CDH from other intrathoracic masses.
The fluid-filled stomach may be absent from the abdomen.
The liver may be herniated,
as well,
appearing as a homogeneous mass in the chest at the level of the heart and continuous with the intraabdominal liver.
Color Doppler ultrasound can be used to document the location of the liver by demonstrating the course of the intrahepatic vessels.
The gallbladder and hepatic or umbilical veins may be abnormally located within the abdomen,
which can be scaphoid.
The abdominal circumference may be smaller than expected for gestational age.
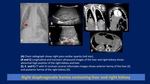
Right-sided CDH is characterized by the presence of a homogeneous mass (liver) in the right chest that often results in left mediastinal shift.
Pleural fluid is often present and bowel may herniate with the liver.
The left shift of the heart is a key finding since,
sonographically,
the liver is similar in appearance to fetal lung and bowel does not reliably herniate.
As discussed above,
color Doppler ultrasound can be used to document the location of the liver.
Sometimes the gallbladder can be seen in the chest,
which when present is another key finding diagnostic of right-sided CDH.
Right CDH is more frequently missed or misdiagnosed than left CDH because the herniated viscera consist predominantly of the right lobe of the liver,
which may have similar echogenicity to the lung or be confused with a solid mass in the chest.
With either left- or right-sided CDH,
esophageal compression secondary to mediastinal shift can result in polyhydramnios,
which is common.
Obstruction of venous return due to mediastinal shift rarely occurs and can result in hydrops fetalis.
Three-dimensional ultrasound imaging,
fetal echocardiography and fetal magnetic resonance imaging (MRI) are other prenatal diagnostic modalities used.
MRI:
MRI confirm presence of CDH and differentiate CDH from other chest masses.
It is superior to ultrasonography in demonstrating position of fetal liver above or below diaphragm.
It can clearly depict diaphragmatic discontinuity,
fetal compressed lung,
and connecting bowel segments between abdomen and chest.
Fetal MRI protocol should include T2WI in all three planes and T1WI breath hold gradient recalled echo images in the coronal plane to assess for liver and meconium positions.
Meconium-filled bowel loops are low signal on T2-weighted images and high signal on T1-weighted images,
making location of the bowel easy.
The liver is high signal on T1-weighted images and intermediate signal on T2-weighted images,
also making it easy to separate from bowel and adjacent lung.
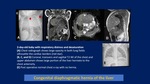
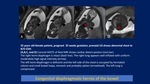
MRI is most helpful in the evaluation of right and bilateral CDH.
In these cases,
with the stomach often located below the diaphragm in the abdomen,
it may be difficult to differentiate a CPAM from a CDH by ultrasound.
MRI easily distinguishes abdominal contents within the chest from cystic lesions and provides specific information on hernia content,
size of diaphragmatic defect,
and amount of ipsilateral and contralateral lung.
Postnatal diagnosis of Bochdalek and Morgagni hernia:
Chest X Ray:
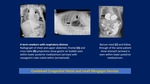
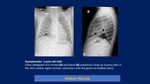
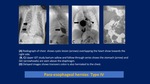
Bochdalek hernia: X- Ray initially,
hemi thorax appear opaque because loops are fluid-filled,
paucity of bowel loops beneath the diaphragm.
Once air swallowing begins,
multiple cystic lucencies and mediastinum shifted to opposite side.
In the case of intraabdominal solid organ herniation such as the liver and spleen,
the hemi thorax can remain homogeneously opacified.
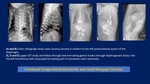
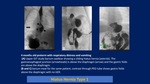
Deviation of lines: endotracheal tube,
nasogastric tube,
umbilical arterial and venous catheters.
The nasogastric (NG) tube deviates to the side opposite to the hernia in the chest.
If the stomach is herniated within the hemi thorax,
the tip of the NG tube can project in the chest.
The position of umbilical venous catheters also is affected according to the location of the liver,
which is shifted either in the abdomen or chest.
In contrast,
the position of umbilical arterial catheters is rarely affected because of their retroperitoneal location.
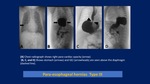
Morgagni hernias: Most cases are discovered incidentally on chest radiographs that are obtained for evaluation of other conditions in older children and adults.
When solid organs such as the liver or spleen are involved,
the appearance may not be specific and can resemble focal diaphragmatic eventration,
lymphadenopathy,
or a foregut duplication cyst.
Ultrasound,
CT,
or MRI can be helpful in the diagnosis when solid organs are herniated.
Fluoroscopy: in elective cases,
contrast gastrointestinal studies performed to confirm diagnosis and delineate the contents.
MRI: has been found to be useful in detecting fetal anomalies and can be a valuable adjunct to evaluate the position of the liver and estimating
lung volume.
Associated cardiac and neural tube defects may affect the outcome of infants with CDH.
CT: for better delineated of position of herniation and help to rule out differential diagnosis like mediastinal masses,
bronchogenic cyst,
and other congenital lung malformations.
Postoperative assessment of Bochdalek and Morgagni hernia:
However,
chest radiographs often are obtained routinely for confirmation of an intact diaphragm and early detection of a possible CDH recurrence.
On follow-up chest radiographs,
abnormalities including persistent lung hypoplasia,
decreased pulmonary vascularity,
and mediastinal shift may be observed.
An ipsilateral pneumothorax is a common finding and should not be rapidly evacuated.
A rapid evacuation of a pneumothorax in this situation may cause mediastinal rotation and subsequent venae obstruction because
of the increased mobility of the neonatal mediastinum.
The pleural air subsequently reabsorbs by itself and sometimes is replaced by fluid.
Hiatal hernia:
Radiographic features:
Plain radiograph:
Retro-cardiac opacity with air-fluid level or lucency.
Fluoroscopy
-Numerous coarse thick gastric folds within the supra-hiatal pouch.
-Tortuous esophagus with an eccentric gastro-esophageal junction.
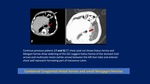
CT:
- Focal fat collection in the middle mediastinum
Omentum herniates through the phrenico-esophageal ligament.
May see an increase in the fat surrounding the distal esophagus.
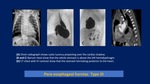
- Para-esophageal hernia through a widened esophageal hiatus
Visualize contents,
size,
orientation of herniated stomach within the lower thorax.
Herniated contents lie adjacent to the esophagus.
- Widening of esophageal hiatus
Dehiscence of diaphragmatic crura (>15 mm): increased distance between crura and esophageal wall.