Diagnostic interventions
Revised International Myeloma Working Group diagnostic criteria for multiple myeloma
| Clonal bone marrow plasma cells ≥10% or biopsy-proven bony or extramedullary plasmacytoma and any one or more of the following myeloma defining events |
|
Hypercalcaemia: serum calcium >0·25 mmol/L (>1 mg/dL) higher than the upper limit of normal or >2·75 mmol/L (>11 mg/dL)
|
|
Renal insufficiency: creatinine clearance <40 mL per min† or serum creatinine >177 µmol/L (>2 mg/dL)
|
|
Anaemia: haemoglobin value of >20 g/L below the lower limit of normal,
or a haemoglobin value <100 g/L
|
|
Bone lesions: one or more osteolytic lesions on skeletal radiography,
CT,
or PET-CT
|
| Any one or more of the following biomarkers of malignancy: |
| Clonal bone marrow plasma cell percentage* ≥60% |
| Involved:uninvolved serum free light chain ratio ≥100 |
| >1 focal lesions on MRI studies |
A bone marrow examination showing presence of clonal plasma cells or histopathological evidence of a plasmacytoma is a definite requirement for the diagnosis of multiple myeloma.
The estimate of bone marrow plasmacytosis should be determined by conventional bone marrow aspirate or biopsy examination.
INTERVENTIONAL OPTIONS
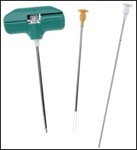
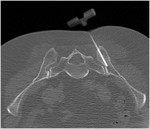
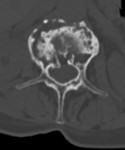
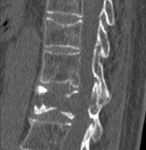
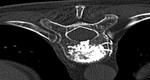
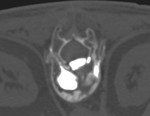
- Clinical biopsy of random bone marrow Fig. 1 / CT guided iliac biopsy Fig. 2
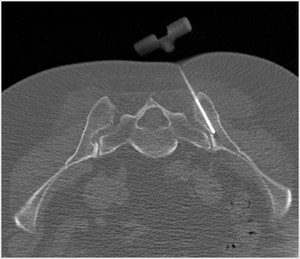
Fig. 2: CT guided iliac biopsy
These two options have similar results.
- Bone biopsy of focal lesion
- Axial (spine)
- Peripheral.
Assess fracture risk before the procedure.
Greater detection of cytogenetic alterations.
Differential diagnosis with other lytic lesions.
Advantages with regard to blind aspiration:
Higher performance if focal lesion biopsy diagnosed by imaging.
Tracking the needle (useful in obese patients).
Assessment of immediate complications.
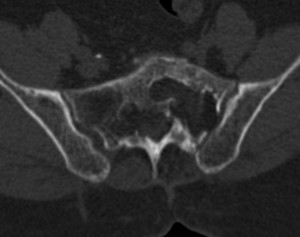
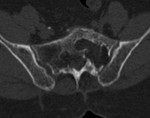
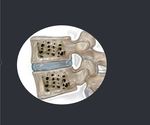
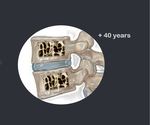
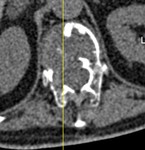
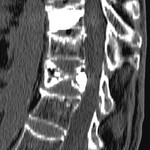
Fig. 3: 70 years. Low back pain
History of plasmacytoma treated with RT.
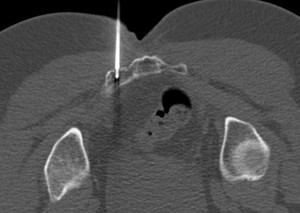
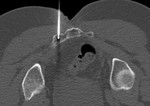
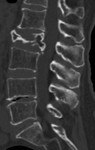
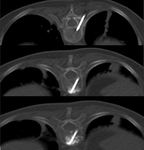
Fig. 4: Result: Post-treatment changes
Biopsy of focal soft tissue lesion
- Superficial: US guided biopsy
- Deep: CT guided biopsy
Therapeutic interventions
34-64% of patients develop pathological/insufficiency vertebral fractures,
usually multiple.
There is increased risk of fracture with each new fracture.
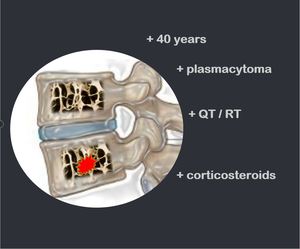
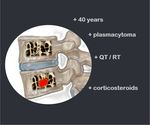
Fig. 7: 40 years / plasmacytoma / QT/RT / corticosteroids
Conservative treatment includes rest,
analgesics,
corset,
chemotherapy,
corticosteroids,
bisphosphonates and radiotherapy; Unfortunately,
some patients fail to mitigate their symptoms despite such treatment.
Vertebral cementation
The objective is to treat the pain associated with the fracture,
in order to improve the quality of life of the patient.
Indications
- Image compatible with fracture +/- focal lesion.
- Moderate-severe pain resistant to conservative treatment (more than 6 weeks).
- Clinico-radiological correlation of symptoms.
- Progressive kyphosis.
Preferential treatment
- Pain that requires hospitalization (treatment during admission).
Contraindications
Absolute
- Uncontrolled anticoagulation.
- Active infection.
- Asymptomatic fracture.
- Allergy to cement.
Relatives
- Flat vertebra (loss of >70% of the vertebral height).
- Canal / Foraminal severe stenosis.
- Limb weakness.
- Gait inestability.
- Sensitive dermatome.
- Fecal / urinary incontinence.
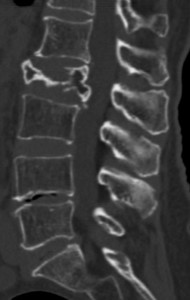
Fig. 8: Flat vertebra
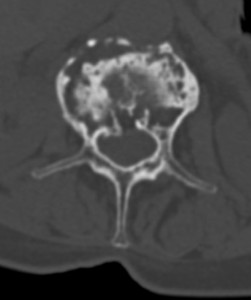
Fig. 9: Canal / Foraminal severe stenosis
Vertebroplasty and Kyphoplasty
Vertebroplasty
- Injection of bone cement into the fractured bodies.
- Maximum 3-4 levels per session.
- It does not reconstitute the morphology or height of the vertebra.
- Guide: fluoroscopy or CT.
Pain control
- 1 week - 1 year: decrease of 2.5 points in VAS (visual analogue scale).
- Use of analgesics: 1 week - 1 year: decrease in 81-85% of patients.
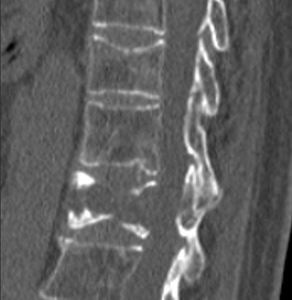
Fig. 10: Image compatible with vertebral fracture +/- focal lesion
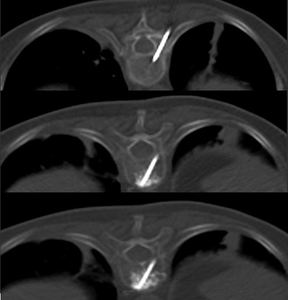
Fig. 12: Injection of bone cement into the fractured bodies.
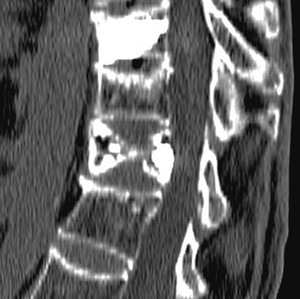
Fig. 13: Injection of bone cement into the fractured bodies.
Kyphoplasty
Injection of bone cement into the vertebral body after insufflation of a balloon that creates a cavity inside of it.
Pros
- Reconstitutes the height of the vertebral body.
- Better control of the disposal of cement.
No difference with Vertebroplasty
- Similar pain control.
- Similar procedure.
- 3-4 levels / session.
Cons
- Risk of retropulsion of the posterior wall.
- Higher cost than vertebroplasty.
Complications of the cementation
Minors
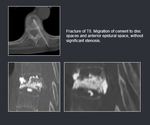
- Migration of cement: foramen,
distal space,
epidural; usually asymptomatic.
- Migration to paravertebral veins: probability <1% pulmonary embolism; usually asymptomatic.
Greater
- Fat ebolism.
Triad: neurologic dysfunction,
respiratory failure and petechiae.
- Anaphylactic reaction to cement.
Other complications
- Fracture of adjacent vertebra within the first two weeks.
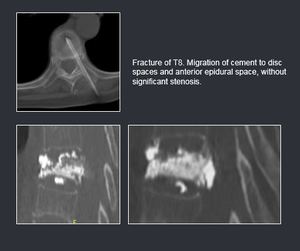
Fig. 16: Complications
Other alternatives:
Radiofrequency + vertebroplasty:
It does not add benefit and it increases the cost.
Risk of neurologic injury if the lytic lesion erodes the posterior wall of the affected vertebra.
Integration of the medical team and doctor-patient relationship
A not negligible number of medical specialties are involved in the management of the MM patients,
specially the fractured ones,
which includes hematologist,
oncologist,
orthopedic surgeon,
anesthesiologist and radiologist,
among others.
Clinical indications for vertebral cementation are commonly encountered in daily practice and because of it,
clinicians must know the available diagnostic and therapeutic interventions radiology can offer.
In our environment many radiologist do not have a dedicated outpatient medical consultation to see patients prior to the procedures, then it is important that clinicians know these techniques so that they can be explained to the patients who need them.