Table of Contents of Venous Pulsatile Tinnitus:
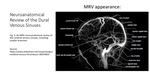
1. Cerebral Dural Venous Sinus Neuroanatomy (Fig.
1)
2. Common Venous Etiology – Systemic: Intracranial Hypertension
3. Common Venous Etiologies –Dural Venous Sinus Related:
- High Riding Jugular Bulb
- Dehiscent Jugular Bulb
- Sigmoid Sinus Diverticulum
- Transverse Sinus Stenosis
4. Uncommon Venous Etiologies
- Enlarged Posterior Fossa Emissary Vein
- Dural Sinus Thrombosis
Common Venous Etiologies – Intracranial Hypertension
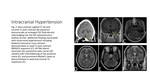
Idiopathic Intracranial Hypertension (IIH) is elevated intracranial pressure without evidence of mass or hydrocephalus.
Increased production of CSF,
impeded CSF absorption,
and increased vascular pressure have all been implicated.
IIH is most commonly seen in middle aged obese females presenting with headaches,
blurry vision,
and transient vision.
IIH is also a common cause of pulsatile tinnitus,
secondary to increased venous pressure. IIH has characteristic CT and MRI findings and must be considered in cases of pulsatile tinnitus.
Prominence of the subarachnoid spaces about the optic nerves,
tortuosity of the optic nerves,
partial empty sella,
flattening of the posterior sclera are the most common imaging findings (Fig.
2).
Venous sinus stenosis has been implicated as a potential cause of IIH and independently as a cause of pulsatile tinnitus (discussed below).
Treatment of IIH include large volume CSF removal,
ventriculoperitoneal shunting,
and venous sinus stenting.
Common Venous Etiologies – High Riding Jugular Bulb
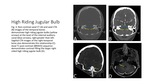
High riding jugular bulb is an anatomic variant that can cause pulsatile tinnitus where the roof of the jugular bulb extends more superiorly within the petrous temporal bone (Fig.
3),
although the exact definition varies.
It is thought that turbulent flow within the jugular bulb is the cause when patients present with pulsatile tinnitus.
On imaging,
a commonly accepted definition is extension of the jugular bulb superior to the level of the internal auditory canal.
Contrast enhanced CT or MR is valuable in demonstrating the extent of the jugular bulb.
Treatment is generally conservative management.
Common Venous Etiologies – Dehiscent Jugular Bulb
Similar to high riding jugular bulb,
dehiscent jugular bulb is an anatomic variant where there is,
instead,
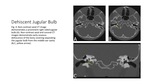
a discrete defect within the bony covering which leads to superior and lateral extension of the jugular bulb into the middle ear cavity.
CT on bone windows best demonstrates this focal defect of this bony covering (Fig.
4).
CTV or MRV evaluation shows an enhancing mass protruding into the middle ear cavity.
Treatment is mostly conservative with surgical repair reserved for the most symptomatic of cases.
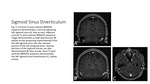
Common Venous Etiologies – Sigmoid Sinus Diverticulum
Sigmoid sinus diverticulum (SSD) is an anatomic anomaly where there is dehiscence or thinning of the mastoidal temporal bone/sigmoid plate (Fig.
5).
Similar to the high riding/dehiscent jugular bulb variants,
DDS is best demonstrated on CTV or MRV where an enhancing mass protruding through a sigmoid plate defect can be visualized.
Treatment is often conservative but endovascular coiling can be performed in severe cases.
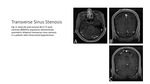
Common Venous Etiologies – Transverse Sinus Stenosis
Transverse sinus stenosis (TSS) is narrowing of the transverse sinus (Fig.
6) which can lead to turbulent flow causing pulsatile tinnitus.
It can be isolated or seen with other conditions such as IIH and SSD (both entities discussed above).
Etiologies of TSS include an underlying primary mass,
prior thrombosis,
or idiopathic conditions.
Digital subtraction angiography (DSA) is most sensitive for diagnosing the anomaly and evaluating pressure gradients for prognosis.
CTV and MRV are also useful in visualizing TSS,
although MRV is more sensitive.
Clinical improvement has been shown with stenting,
which decreases the pressure and turbulent flow.
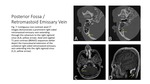
Uncommon Venous Etiologies – Enlarged Posterior Possa Emissary Vein
An enlarged emissary vein is an anatomic and embryonic variant where there is a residual venous tract that connects the sigmoid sinus to the extracranial venous drainage system.
It is postulated that this tract can have bidirectional flow due to lack of valves,
which can result in turbulent flow and pulsatile tinnitus.
Physical exam can show decrease in tinnitus with the Valsalva maneuver or compression of the ipsilateral jugular vein.
CT can show an enlarged tract with postcontrast CT or MRV evaluation demonstrating a vessel contiguous with the sigmoid sinus and superficial extracranial veins (Fig.
7).
Doppler ultrasound can be of value by showing the direction of flow.
Treatment often is conservative with endovascular repair considered rarely.
Uncommon Venous Etiologies – Dural Venous Sinus Thrombosis
Dural venous sinus thrombosis (DVST) occurs with clotting in a dural venous sinus resulting in flow obstruction and increased pressure within the affect vessel,
which can clinically cause pulsatile tinnitus.
The clot can also propagate into contiguous smaller veins potentially leading to complications.
A number of etiologies can cause DVST including trauma,
infection,
hypercoagulable states,
and dehydration.
Venous infarct and hemorrhage are the most dreaded of acute complications of DVST.
Sequelae of DVST include sinus stenosis (discussed above) and chronic thrombosis resulting in collateralization.
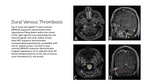
DVST has characteristic imaging findings on both CT and MRI (Fig.
8).
On noncontrast CT,
DVST can manifest as a hyperdensity of at least 60 Hounsfield units corresponding to a dural sinus.
Contrasted enhanced CT will demonstrate an intraluminal filling defect within the opacified dural venous sinus,
characterized as the 'empty delta' sign where the enhancing dura surround the clot.
GRE is one of the most sensitive MRI sequences for DVST,
showing blooming artifact in the region of the thrombus.
Contrast enhanced MRI or MRV appears similarly to CT where there is an intraluminal filling defect within the enhancing vessel,
causing varying degrees of obstruction and distension.
Treatment consists of thrombolytics with mechanical thrombectomy is reserved for severe cases.
In our case-based review,
common venous etiologies include intracranial hypertension,
transverse sinus stenosis,
dehiscent jugular bulbs,
high-riding jugular bulbs,
and sigmoid sinus diverticula.
Uncommon etiologies of venous pulsatile tinnitus include asymmetrically or unusually enlarged posterior fossa emissary veins,
and sinus thrombosis.
We will illustrate the neuroimaging findings of these entities in representative patient cases.