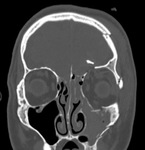
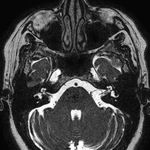
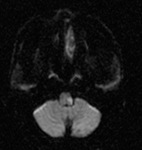
Nuclei of CNs,
except I and II,
are located in the brainstem.
From their origin,
nerves are divided in cisternal,
intracranial and extracranial segments.
CNs anatomy and functions are summarized in Table 2.
Pathology of CNs involves a wide spectrum of etiologies,
summarized in Table 3.
Neoplasms:
Schwannoma
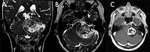
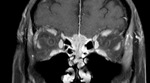
Schwannomas are benign nerve sheath tumors that originate from Schwann cells.
Typically (90%) they arise from the VIII CN; trigeminal involvement is the second most common (0.8%–5%) [6,7].
Intracranial schwannomas can be associated with Neurofibromatosis 2 (NF2).
Patients with NF2 can have bilateral vestibular schwannomas or non-vestibular schwannomas [8].
Imaging shows the slog grow of the tumor,
with osseous remodeling of neural foramina and deformation of the adjacent brain tissue.
Features of end-organ compromise can be present.
On CT schwannoma has a low-intermediate attenuation with variable enhancement.
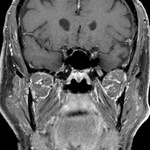
On MRI it shows iso-hypointensity on T1-weighted sequences,
high signal on T2 weighted sequences and marked enhancement on post-contrast images,
eventually with unenhanced cystic spaces [8] (Fig.1,2).
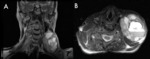
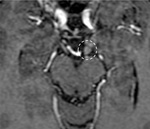
Neurofibroma
Neurofibromas rarely involve cranial nerves,
while are more commonly found extracranially.
They are typically associated with Neurofibromatosis 1 (NF1) and can show malignant transformation (Fig.3).
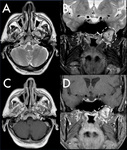
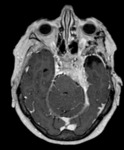
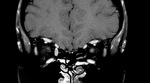
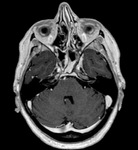
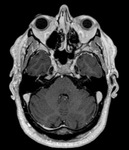
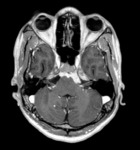
Optic nerve glioma
Optic nerve glioma is an uncommon tumor that typically occurs in children.
It can be associated with Neurofibromatosis 1 (NF1) and,
in this case, can be multifocal and bilateral.
On MRI it typically appears isointense on T1-weighted images and iso-hyperintense on T2-weighted images,
with variable contrast enhancement; in non-NF1 patients,
cystic components may be detected [9] (Fig.4).
Esthesioneuroblastoma
Esthesioneuroblastoma (ENB) is a rare malignant tumor of neural crest origin,
arising from the olfactory epithelium.
It occurs typically in the second and sixth decades of life,
without a gender predilection [10].
Clinical presentation can include epistaxis,
nasal obstruction,
decreased olfactory function,
diplopia,
and proptosis.
ENB may invade paranasal sinuses,
orbits,
and anterior cranial fossa,
and,
if metastatic,
involve local lymph nodes,
with distant metastasis to lungs,
liver,
and bone.
On CT,
ENB appears as a homogeneous soft tissue mass in the nasal cavity; however,
CT is useful to evaluate bone involvement.
On MRI,
it usually appears hypointense on T1-weighted sequences and iso-hyperintense on T2-weighted sequences.
Contrast enhancement is marked and homogeneous,
excepting for areas of necrosis or hemorrhage [10] (Fig.5).
Perineural spread of tumor
Perineural spread of tumor is the extent of tumor cells along the tissue of nerve sheath.
It may occur with any head and neck malignancy.
Typically,
the second (V2) and the third (V3) branches of the V CN, and the descending branch of the VII CN serve as conduit for perineural spread.
Clinically,
it may manifest with neural disfunction symptoms,
as pain,
dysesthesias or muscle denervation atrophy [4].
On MRI,
the nerve is thickened with enhancement on post-gadolinium sequences (imaging techniques with fat suppression are used to better increase the conspicuity of the enhancement) [11].
Tumoral growth may cause enlargement of skull base foramina (Fig.6).
Leptomeningeal spread of tumor
Primary (medulloblastoma,
ependymoma,
oligodendroglioma and glioblastoma) and secondary (leukemia/lymphoma,
breast cancer,
lung cancer and melanoma) tumors may spread through subarachnoid spaces with extension along the CNs.
VII and VIII CNs are the most affected.
[12].
Clinical findings include multiple cranial neuropathies and mental status changes,
secondary to meningeal irritation and hydrocephalus.
The nerve may enhance on post-gadolinium sequences and appear enlarged (Fig.
7).
Meningioma
Meningioma is the most common extra-axial tumor of central nervous system.
After the acoustic schwannoma,
it represents the second most common mass in the cerebellopontine angle.
Meningioma appears as a lobular,
extra axial mass with well-circumscribed margins and a broad-based dural attachment.
On MRI,
it is iso-hypointense on the T1-weighted sequences and iso-hyperintense on the T2-weighted sequences.
A rim of high T2 signal that separates the mass from the adjacent brain is often visible (“cleft signs”).
Post-contrast sequences show marked and homogeneous enhancement with rare central nonehancing areas,
corresponding to necrosis or calcifications.
Osteolysis,
hyperostosis and enlargement of the adjacent foramina can be found [13] (Fig.
8).
Inflammation:
Optic neuritis
Optic neuritis (ON) usually refers to inflammatory process that involve optic nerve.
ON may be observed in autoimmune (for example Multiple Sclerosis and Neuromyelitis Optica Spectrum Disorders) and systemic diseases (Sarcoidosis,
Bechet disease,
Lupus erythematosus,
Wegener disease,
Sicca syndrome) [14].
Clinical findings are painful eye movements and visual loss.
On MRI the nerve appears swollen and hyperintense on T2-weighted sequences,
with contrast enhancement best seen on fat-suppressed T1-weighted sequences [7] (Fig.
9).
Tolosa-Hunt syndrome
Tolosa-Hunt is an uncommon disease related to a retro-orbital pseudotumor extending in the cavernous sinus [15,16].
It is an idiopathic disorder and it consists in a granulomatous inflammation of the lateral wall of the cavernous sinus or superior orbital fissure.
Clinical findings are unilateral painful ophthalmoplegia,
diplopia and deficit of the V1 branch of V CN.
On imaging,
an infiltrative soft tissue mass within the cavernous sinusmay be found.
The tissue is iso-hypointense on T2-weighted sequences,
whit avid contrast enhancement on post-gadolinium images.
After diagnosis,
a good response to steroid therapy can be achieved (Fig.10).
Bell’s palsy
Bell’s palsy (idiopathic facial palsy) is the most common cause of unilateral peripheral nerve neuropathy.
Clinically,
it may present with dysgeusia,
mastoid pain,
impaired salivation and lacrimation.
Herpes-Simplex-Virus reactivation seems to be the most probable aetiology [4].
Typical Bell’s palsy does not require imaging studies.
MRI may be useful to exclude other lesions responsible of atypical Bell’s palsy or recurrent palsy [17].
The facial nerve shows increased enhancement on post-contrast sequences with involvement of one or more segments,
without nodularity.
Enhancement of distal intrameatal and labyrinthine segments is typical [17].
On T2-weighted sequences the nerve may appear hyperintense.
In case of irregular or nodular enhancement,
other causes of pathology (such as perineural spread of tumor) should be considered.
Prognosis is often good and the treatment is based on corticosteroid therapy,
often with the addition of acyclovir (Fig.11).
Infection:
Viral infections (Herpes simplex virus type 1,
Cytomegalovirus and Varicella zoster) may manifestwith cranial nerve involvement and abnormal enhancement of the nerve on MRI [18].
As regards bacterial meningitis (Haemophilus Influenzae,
Streptococcus Pneumoniae and Neisseria Meningitidis), they may have normal imaging or leptomeningeal enhancement on MRI post-contrast sequences [4].
Also intracranial Tuberculosis can manifest as leptomeningitis with involvement of cranial nerves (Fig.
12).
Cryptococcus neoformans is associated with the Cryptococcal meningitis,
characterized by II nerve neuropathy.
Fungal infections (Rhinocerebral mucormycosis) occur in immunocompromised patients,
with sinonasal disease that may progress to the orbit and cavernous sinus.
Vascular and perineural invasion and local thrombotic infarction have been describes as complications.
Lyme disease may involve any of cranial nerve (typically VII CN) that appears thickened and enhanced [18].
Trauma:
CT is the best imaging modality to detect skull base fractures and foraminal involvement.
However,
MRI may demonstrate intraneural edema or hemorrhage,
especially on T2* weighted-sequences. I CN may be involved in the closed injury of basal frontal lobe,
with or without association of cribriform plate fracture (Fig.13). II and III CNs may be affected in the orbital and optic canal fractures.
Lesions of the VI CN are reported in the fracture of the clivus and petrous apex.
Injuries of the VII CN are associated to temporal bone fractures [4,5,19,20].
Also iatrogenic injuries may be the complications of a variety of surgical procedures. VII CN paralysis may follow temporal bone and parotid surgery,
while lower cranial nerves may be involved during neck dissection; in particular,
the recurrent laryngeal nerve may be injured during thyroid and parathyroid surgery [21].
Vascular:
Neurovascular compression
Neurovascular compression syndromes are caused by vascular structures that directly contact the cisternal tract of a cranial nerve (Fig.14).
Clinical features include neuralgia of V and IX CNs,
vestibular paroxysms and hemifacial spasm.
Also nonhemorrhagic aneurysms may be associated to nerve disfunction,
for example in case of vision loss due to compression of II CN or optic chiasm by proximal internal carotid artery,
and III,
IV,
or VI CNs palsy secondary to intracavernous aneurysm.
Imaging may demonstrate displacement and compression of a nerve by redundant arteries.
Steady-state sequences and TOF or 3D T1-weighted post contrast images are very useful for diagnosis and preoperative evaluation [22].
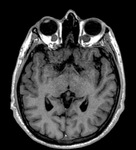
Ischemia:
Ischemic lesions of the brainstem may cause isolated nerve palsies,
more commonly in elderly population.
Diffusion weighted imaging (DWI) sequences are the best to visualize an acute ischemic lesion,
whereas FLAIR and T2-weighted sequences are useful to visualize subacute or old infarctions [5].
The anatomical knowledge of nuclei of CNs is fundamental to interpret ischemic nerve palsies (Fig.
15).