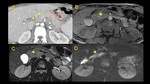
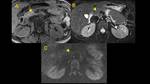
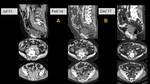
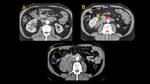
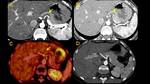
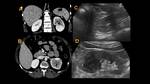
IgG4-related Pancreatitis (Fig. 1, Fig. 2)
IgG4-related pancreatitis is the most common intrabdominal manifestation of the IgG4-RD and it accounts for 5-11% of chronic pancreatitis.
Patients present with similar symptoms of pancreatic adenocarcinoma or chronic pancreatitis,
such as mild abdominal pain,
weight loss,
obstructive jaundice,
and new-onset diabetes.
Radiological features are key clues in the differential diagnosis along with involving of extrapancreatic organs and responsiveness to glucocorticoids.
On TC,
IgG4-related pancreatitis presents as a diffuse enlargement with loss of
pancreatic clefts (“sausage-shaped” sign) or segmental enlargement of the head and uncinate process.
A rare form has been described where multifocal hypodense
masses are present within a diffusely enlarged pancreas.
A hypoattenuating halo (capsule-like rim) caused by sclerosis of surrounding fat is frequently seen and the pancreatic duct is diffusely narrowed.
It shows reduced enhancement during pancreatic phase (40 seconds after contrast injection) and delayed enhancement on portal venous phase (70 seconds)
On MR,
hypointensity on T1WI and mild hyperintensity on T2WI are seen,
with delayed contrast-enhancement and high restriction of MR-diffusion sequences,
with ADC values even lower than pancreatic adenocarcinoma.
IgG4-related pancreatitis may be self-limiting in 74% of patients.
Glucocorticoid treatment achieve morphological and functional remission in 98% of patients,
but recurrence rates are high (24%)
Patients with pancreatic adenocarcinoma present with a hypodense poorly marginated focal mass with heterogeneous enhancement.
An extensive desmoplastic reaction,
encasement of vessels and dilatation of biliary and pancreatic ducts are also characteristic radiological features.
Hepatobiliary Tract Involvement
IgG4-related sclerosing cholangitis is the most common extrapancreatic manifestation of IgG4-RD in the abdomen.
70% of IgG4-related sclerosing cholangitis is associated with IgG4-related pancreatitis.
Clinical manifestations are similar to those observed in primary sclerosing cholangitis and cholangiocarcinoma.
MR-cholangiography depicts segmental and long strictures with prestenotic dilatation,
whereas primary sclerosing cholangitis displays band-like strictures of 1-2 mm with a beaded and pruned-tree appearance and diverticulum-like outpouching.
Strictures of the lower common bile duct are also more frequent in IgG4-related sclerosing cholangitis.
There are four types of IgG4-related sclerosing cholangitis according to the location of the biliary tree strictures:
-
Type 1: Distal common bile duct stricture.
-
Type 2: Distal common bile duct stricture with diffuse intrahepatic cholangiopathy with (2a) or without (2b) prestenotic dilatation.
-
Type 3: Hilar and distal common bile duct stricture.
-
Type 4: Hilar stricture.
Just like primary sclerosing cholangitis,
IgG4-related sclerosing cholangitis can also progress to end-stage liver disease and cholangiocarcinoma.
IgG4-related sclerosing cholecystitis is a rare condition,
usually presented along with IgG4-related sclerosing cholangitis,
that presents as diffuse thickening of the gallbladder wall or an infiltrating tumour,
difficult to differentiate from gallbladder carcinoma.
IgG4-related hepatopathy presents non-specific radiological features like hepatomegaly and periportal edema.
Benign pseudotumors have also been described.
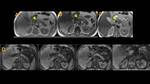
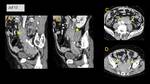
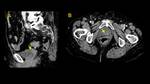
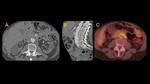
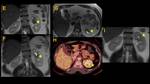
Retroperitoneal Fibrosis (Fig. 3, Fig. 4, Fig. 5, Fig. 6, Fig. 7, Fig. 8, Fig. 9)
It is present in 10-20% of patients with IgG4-related pancreatitis.
It can manifest 3 types of lesions according to the location of sclerosing inflammation in the aortic adventitia (periaortic),
in the submucosal layer of the urinary tract and in the peritoneum/fascia.
On imaging,
this condition appears as a soft-tissue mass with a smooth border to the surrounding aorta and its branches or renal parenchyma.
Periaortic type is the most common.
It often affects infrarenal abdominal aorta and its branches.
An inflammatory abdominal aneurysm or aortic dissection have been described.
Urinary tract type is often associated with unilateral hydronephrosis,
usually less severe than the other two types.
It seems that the less degree of fibrosis or the epithelium layer spare in this type could explain this feature.
Peritoneum/fascia type often presents as a plaque-like soft-tissue mass in presacral space,
with infiltration of pelvic organs.
Differential diagnosis with other retroperitoneal masses is important (lymphoma,
large-vessel vasculitis,
syphilis,
and sarcoidosis-induced aortitis).
Smooth borders of the mass and less severe hydronephrosis are key characteristics of IgG4-related retroperitoneal fibrosis.
Besides,
95% of patients with IgG4-related retroperitoneal fibrosis have lesions in other locations.
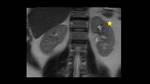
Renal Involvement (Fig. 10, Fig. 11, Fig. 12)
It is present in about one-third of patients with IgG4-related pancreatitis.
IgG4-RD most frequently appears as multiple round or wedge-shaped renal cortical nodules,
hypointense both on T1 and T2WI with delayed contrast-enhancement.
Differential diagnosis includes pyelonephritis,
vascular insult or metastases.
Renal involvement may also appear as diffuse patchy involvement,
a rim of soft tissue around the kidney,
bilateral nodules in the renal sinuses and diffuse wall thickening of the renal pelvis wall.
Lymph Node Involvement
It is present in 80% of patients with IgG4-RD,
either generalized lymphadenopathy or localized disease around the affected organ.
Radiological features of the lymph nodes are non-specific and diagnosis is based on histology and involvement of another abdominal organ.
The differential diagnosis in patients with generalized lymphadenopathy includes sarcoidosis,
multicentric Castleman disease,
infection (eg,
tuberculosis),
and lymphoma or other malignancy.
Others
IgG4-related sclerosing mesenteritis appears as a soft-tissue mass encasing the mesenteric vessels with a fat ring around them.
It can lead to small bowel obstruction.
Radiological features of lymphoplasmacytic gastritis include loss of fundal folds,
so stomach adopts a narrow tubular morphology,
similar to those observed in other types of atrophic gastritis.
Patients with IgG4-related prostatitis present with enlarged gland with heterogeneous contrast-enhancement and multiple adenopathies.