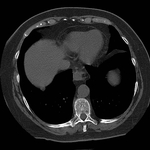
1.
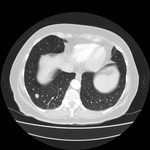
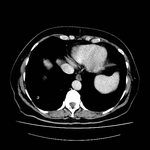
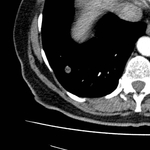
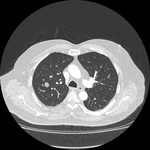
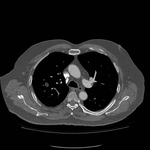
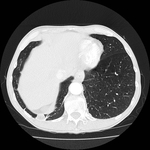
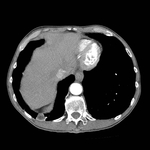
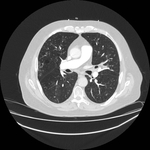
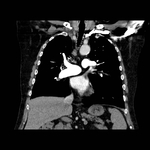
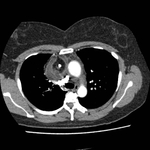
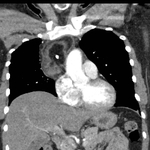
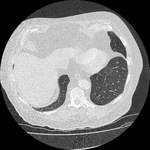
Pulmonary hamartoma
Hamartomas are congenital indigenous benign tumors that can be found in various part of body.
Hamartomas constitute 75% of benign pulmonary lesions.
80 percent of these hamartomas are intraparenchymal while 20 % are endobronchial.2 Intrapulmonary hamartomas also appear as small well delineated round to ovoid solitary nodules on the radiographs.
These are mostly picked as an incidental finding.
CT can help in differentiating hamartoma from simple lipomas and sinister pathology.
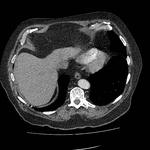
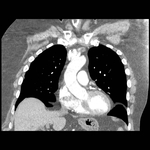
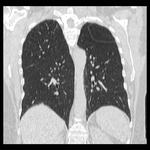
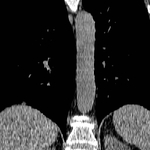
These appear as small foci of heterogenous density containing intralesional fat,
soft tissue with or without internal calcification.
(case 1,
Fig 2-4) Larger hamartomas are more frequently associated with pop-corn type calcifications.
Peripheral location,
size and lack of measurable enhancement in the soft tissue differentiates it from lipoosarcoma.
Metastasis are usually of homogenous soft tissue density with or without cavitation,
lack intralesional fat and can be multiple.
Hamartomas (50 %) with homogenous soft-tissue attenuation are categorized as pulmonary nodules of unknown origin.
Hamartomas can be found in endobronchial location as well.
Correct CT categorization can obviate the need of biopsy.3
2.
Pulmonary lipoma
Fat cells in the interstitial space of the lung can form a benign encapsulated soft-tissue neoplasm,
lipoma.
Lung parenchymal lipoma is a rare entity.
It can be seen as an incidental focal well circumscribed soft tissue density nodule on routine chest radiograph because of the small size.
These can be mistaken for metastasis or infective foci depending on the clinical setting.
On CT imaging these are seen as homogenously low density foci with fat attenuation typically in the periphery surrounded by normal lung tissue (Case 2 and 3; Fig 5-8). In contrast to lipomas, liposarcomas are larger in size with inhomogeneous appearance containing intralesional fat with irregular areas of enhancing soft-tissue.4
3.
Endobronchial lipoma
Endobronchial lipomas are well marginated mesenchymal tumors that originate from submucosal or interstitial fat cells.
These constitute only 0.1% of all pulmonary tumors and roughly 3.2%– 9.5% of all benign endobronchial tumors.5 These can be symptomatic,
patient may present with persistent cough,
chest pain,
dyspnea,
recurrent fever and pneumonia and wheezing.
Conventional radiographs can be normal or may show post obstructive atelectatic changes.
CT images show a well circumscribed endobronchial lesion with homogenous fat attenuation.
Perilesional bronchocele or atelectasis can also be seen because of partial or complete obstruction of the bronchus.
(Case 4; Fig 9 and 10)
4.
Dermoid / teratoma
Teratomas are germ cell neoplasms arising from ectopic pluripotent stem cells that contain one or more well-differentiated tissues from the ectoderm,
mesoderm,
or endoderm.
Majority of the germ cell neoplasms are teratoma frequently seen in anterior mediastinum.
Teratomas are round encapsulated benign neoplasms with lobulated margins.
These are typically seen in younger male population.
Conventional radiography depicts teratomas as soft-tissue-opacity lesions in the anterior mediastinum.
Approximately 21% of teratomas demonstrate calcification,
6% have a visible fat radiolucency and only 2% demonstrate visible fat-fluid level.6 CT imaging shows lobulated well defined masses with heterogenous density.
Teratomas are bigger in size on comparison to the hamartomas.
Soft-tissue,
fluid,
fat,
and calcium attenuation can be seen in the tumor parenchyma (Case 5; Fig 11 and 12).
Fat-suppressed MR imaging sequences can be used to confirm fat content.
On the contrary,
teratocarcinomas are more nodular,
locally invasive,
poorly defined tumors that frequents show post contrast capsular enhancement.
5.
Intrafissural fat
Intrafissural fat appears as a small collection of supradiaphragmatic fat invaginating into the inferior aspect of the major interlobar fissure.
On chest radiographs,
the intrafissural fat corresponded to a sharply marinated density and can be confused with pleural effusion.7 CT images can reveal fat density in the major fissure with triangular morphology,
the base of which abutted the anterior diaphragmatic surface and the apex of which tapered into the proximal part of fissure.
(case 6;Fig.
13-15)
6. Pleural Lipoma
Pleural lipomas arise from the submesothelial layers of parietal pleura.
These can extend into the subpleural,
pleural or extrapleural space.
They are soft,
well circumscribed encapsulated fatty tumors that demonstrate slow growth.8 Only large sized pleural lipomas are incidentally detected on radiography.
CT images demonstrate homogeneous fat attenuation lesions close to the diaphragm.
(Case 7; Fig.
16-18)