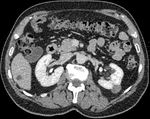
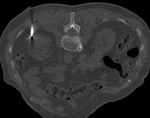
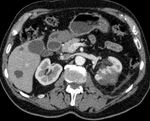
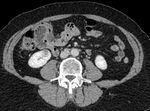
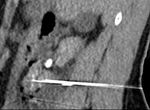
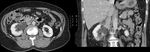
Our institution is the 2nd longest running RFA service within the UK.
We present retrospective data having reviewed cases for complications in >150 patients,
who underwent percutaneous radiofrequency ablation (pRFA) for renal masses in last five years. We recorded demographic data,
various complications including hemorrhage,
renal vascular injury,
urothelial injury,
pain,
pelvicalyceal leakage,
arteriovenous malformation,
infection,
bowel injury,
pneumothorax,
skin burn,
nerve injury,
tract seeding and miscellaneous complications and will be compared with published scientific data.
Percutaneous radiofrequency ablation of small renal lesions is an evolving technique gaining popularity around the world.
This is generally considered for patients who are poor surgical candidates,
while surgical resection remains the first choice for renal cell tumors.
The candidates that are not fit for surgery or decline operation for any reason can be treated with this method without major complications in majority of cases. Most common complications recorded and techniques to reduce risk of these complications and outcomes are discussed in our study.
The revised Clavien–Dindo classification is used to grade complications from I to V (Table 1) arising from renal mass ablation.1,2,3,4

Table 1: Modified Clavien–Dindo classification
References: 1. Kurup AN. Percutaneous ablation for small renal masses-complications. Semin Intervent Radiol. 2014 Mar;31(1):42-9. doi: 10.1055/s-0033-1363842. Review. PubMed PMID: 24596439; PubMed
Various complications related to renal tumor ablation include injury to vasculature,
upper urinary tract collecting system and surrounding soft tissue. Different urological complications from hemorrhage,
ureteral stricture,
urine leak to urinary tract infection are described in literature.
Further,
non urological complications including pneumothorax,
nerve injury,
skin burn,
tract seeding and other less common medical events are also identified.
Hemorrhage is the most common complication encountered,
keeping in view that some element is always expected following a percutaneous intervention and ablation of a renal mass.
Almost all scans during or straight away following renal ablation procedures show some perinephric hemorrhage,
which is not related to technique used for ablation. Hemorrhage was identified in 1.2% RFA procedures in a series of cases.3 Hemorrhage can be related to the size of electrode used and platelet dysfunction especially at low temperature4.
Post RFA injury to the proximal ureter and ureteropelvic junction remains a potential risk.1,6 RFA of medial and lower pole renal masses can result in proximal ureter injury.
The injury may result from direct puncture or secondary to thermal injury and can result in stricture or urine leak/ contrast extravasation.
The urinary injury usually heals spontaneously; however,
persistent urinoma can require drainage or temporary placement of a ureteral stent for diversion.7
Infection is another possibility in these procedures,
which may be involving the ablation zone,
urinary tract or adjacently placed bowel loops.
However,
it occurs in fewer than 1% of cases.3,8,9 Injury to bowel is a serious complication,
which may result in perforation and lead to development of a colonephric fistula and may require percutaneous drainage or surgical repair.
To avoid such injuries different maneuvers and modification can be done to target renal masses.
Repositioning of position to achieve greater distance between the bowel and the mass.8 Furthermore,
displacement techniques like hydrodisplacement with fluid,
gas or manual manipulation may solve the issue by increasing the distance.
Pneumothorax can occur in some cases,
especially when treating an upper pole renal lesion which is close to the lung base.
Various studies have reported the incidence of pneumothorax up to 2%.3,10 In most of cases this a self limiting and asymptomatic but in case of moderate or large pneumothorax interventions like aspiration or chest tube placement is required.
Other complications include skin burns,
nerve injury,
tract seeding and less common ileus,
hypertension,
arrhythmia,
myocardial infarction,
renal infarction, pneumonia,
pulmonary embolism and edema.3,7