Type:
Educational Exhibit
Keywords:
Trauma, Tissue characterisation, Imaging sequences, Contrast agent-intravenous, Nuclear medicine conventional, MR, CT, Spleen, Gastrointestinal tract, Abdomen
Authors:
G. Porrello; Palermo/IT
DOI:
10.26044/ecr2019/C-1320
Background
The term “splenosis” was first defined by Buchbinder and Lipkopf in 1939[1].
It is a rare,
benign,
acquired condition,
defined as the auto-transplantation of splenic tissue in a heterotopic location.
It arises in patients who underwent a splenic rupture or removal and results from the spillage of cells from the damaged pulp of the spleen in nearby body cavities[2].
Splenosis has been reported to occur in up to 67% of patients who have had splenic trauma[3],
even though the real incidence is unknown,
since it is an incidental finding[4].
Splenic nodules can be found in liver,
pancreas,
kidney,
but are most often seen within the parietal peritoneum,
mesentery,
greater omentum,
small and large bowel and the diaphragmatic surface[5],
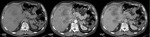
in a pattern that typically resembles metastatic seeding[3].
(Figure 1)
The history of splenosis is deeply connected to the diagnosis of cancer.
The first known case of hepatic splenosis,
was based on a misdiagnosis of liver cancer[4] and there are cases of splenosis mistaken for metastatic spread of almost all types of cancers[3;6-8].
Splenosis implants are similar to malignant diseases on imaging and acknowledging this rare condition is essential to consider it in the differential diagnosis[9; 10].