Lesion description
The lesion was a mass in 70% (125/179),
a NME in 27.3% (49/179) and a focus in 2.7% (5/179).
The average lesion size was 18 mm (3-85 mm).
The size of 45/179 (25.1%) lesions was inferior to 10 mm; 49/179 (27.4%) lesions size ranged from 10 to 20 mm,
and 85/179 (47.5%) lesions were larger than 20 mm.
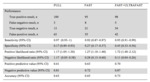
BI-RADS performance on FULL and FAST protocol readings
All cancers were detected on FAST protocol.
FAST protocol showed lower diagnostic performance (AUROC: 0.802) compared to FULL protocol (AUROC: 0.834)(p<0.01) with a higher number of cancers rated BI-RADS 3 (PPV of malignancy of 27.5% (8/29) in FAST versus 18.7% (3/16) in FULL protocol (Fig 3). Inter reader agreement of BI-RADS classification for FAST protocol was excellent with a Kappa value equal to 0.801 (0.715-0.887).
ULTRAFAST sequence analysis
171/179 (95.5%) lesions were visible on the ULTRAFAST sequence only.
Reading only the ULTRAFAST sequence,
we did not identify 8/179 (4,5%) lesions including 5/76 (3.9%) benign lesions and 3/103 (2.9%) breast cancers.
The 3 undetected cancers were 2 small intra ductal carcinoma (size =7mm),
1 papillary carcinoma that appeared as a NME smaller than 1cm.
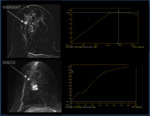
All visible lesions on ULTRAFAST sequence enhanced within the 7 first ranks (earlier than 1min after injection).
Inter reader agreement to determine the first ULTRAFAST rank to detect the lesion was good with a kappa value of 0.651 (0.535-0.768)
The wide majority of cancers (84%,
87/103) enhanced whithin the first four ranks (i.e 31sec after injection).
Malignant lesions were 5.6 times more likely to be associated with early enhancement (within the first four ranks,
with mean a Time To Enhancement (TTE) < 31 sec) rather than delayed (after the four rank) with an OR = 5.6 (IC 95%: 3.3 – 20.4; p < 0.0001) (Fig 4.).
Independently from size,
an earlier first rank of lesion detection was correlated with malignancy.
All semi-quantitative parameters were significantly different between benign and malignant lesions (except Rmax timing).
Malignant lesions displayed a higher enhancement integral,
a higher enhancement amplitude,
a shorter time of half rising,
a steeper maximal slope,
a higher maximal slope of increase,
a higher wash-in rate,
and a higher maximum enhancement rate (R Max).
Building the abbreviated protocol
A multivariate analysis including all significant features issued from ULTRAFAST analysis (TTE <31sec or rank 1-2-3-4,
EA,
EI,
THR,
MS,
MSI,
RMax,
WIR),
only TTE <31sec was significantly associated to malignancy (p<0.0001 OR= 3.9).
Thus,
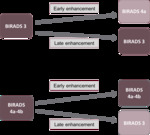
readers reclassified BI-RADS 3,
BI-RADS 4a,
BI-RADS 4b using the data issued from the ultrafast sequence (i.e early enhancement (TTE <31sec or rank 1-2-3-4) as following: BI-RADS 3 lesions with a suspicious early enhancement (TTE < 31s) were upgraded as BI-RADS 4a.
BI-RADS 4a and 4b lesions with a non-suspicious late enhancement (TTE > 31 s) were downgraded as BI-RADS 3 (Fig 5). No change was performed on BI-RADS 4c or BI-RADS 5 lesions.
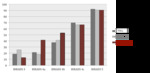
Predictive positive values as well as positive likelihood ratio for each BI-RADS category determined for each protocol are summarized in Figure 6 and percentage of malignant lesions in each reading protocols represented in Figure 7.
Performances of the ABBREVIATED PROTOCOL
Abbreviated protocol (combining FAST and ULTRAFAST data) had better diagnostic performance (AUROC = 0.826) compared to FAST protocol (AUROC = 0,
802) (p<0.01) and no significantly different performance compared to the FULL standard protocol (AUROC = 0.834).
Abbreviated protocol could have avoided unnecessary biopsies in 8.9% of lesions (16/179) rated BI-RADS 4a and 4b on FAST protocol and confirmed benign (p=0,0139) and 10.6% (19/179) of lesions incorrectly rated on FULL protocol (p=0,0034)(Figure 8).
Inter reader agreement for BIRADS performance of abbreviated protocol was excellent with a Kappa values equal to 0.889 (0.840-0.938)