1.0 Congenital Abnormalities
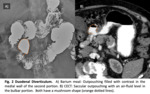
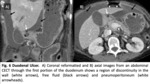
1.1 Duodenal Diverticulum
Are classified as primary or secondary.
Primary diverticula are believed to be due to abnormalities of recanalization of the duodenal lumen during gestation.
They usually occur within the 2nd part,
most are seen on the medial wall around the ampulla.
(5)
Secondary diverticula are related to an underlying chronic duodenal ulcer.
Acquired type is more common than the congenital.
(4)
Findings. Fig. 2
- Barium meal: Contrast filled outpouching of the duodenal lumen.
- CT: Saccular outpouching with air,
fluid,
contrast or air-fluid level.
They are usually asymptomatic,
only 10% cause symptoms and only 1% or less require treatment for perforation,
haemorrhage,
obstruction or acute diverticulitis.
(5)
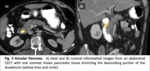
1.2 Annular Pancreas
The pancreas develops from two buds,
normally the ventral bud it is bifid,
with atrophy of one of the buds and fusion with the dorsal.
(5) The uncinate process and the inferior portion of the head arise from the ventral bud.
(6)
Annular pancreas is an uncommon congenital abnormality that causes duodenal obstruction.
The presentation is due to pancreatitis in adults.
Has a prevalence of 5 -15 cases of 100,000 adults in an autopsy.
ERCP have reported a prevalence of 1 - 250 or 400 cases per 100,000 adults.
(6)
The pancreas surrounds completely or partially the second portion of the duodenum.
The risk of duodenal obstruction is similar in incomplete (33%) and complete annular pancreas (40%,
p=0.75).
(6)
Findings. Fig. 3
- Radiograph: “Double bubble” sign,
dilatated stomach.
- ERCP: Pancreatic duct of Santorini folding around the duodenum.
- Barium meal: Postbulbar excentric narrowing of the lumen.
- CT: A crocodile jaw configuration of pancreatic tissue anterior and posterior to the duodenum is highly suggestive of incomplete annular pancreas.
The posterolateral extension of pancreatic tissue to the second part of the duodenum is more specific for annular pancreas than the anterolateral extension.
- MRCP: The best non-invasive method of ascertaining the ductal configuration.
2.0 Inflammatory/Infectious
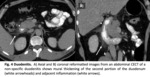
2.1 Duodenitis
Duodenal inflammation from any cause,
the most common cause of duodenal inflammation is secondary involvement from pancreatitis.
(4,5) The most common infectious cause is Helicobacter pylori.
(5)
Findings. Fig. 4
- Barium meal: Fold thickening in antrum and duodenal bulb,
duodenal spasm,
mucosal nodularity.
(7)
- CECT: Thickened duodenal wall,
increment of enhancement,
and adjacent inflammation.
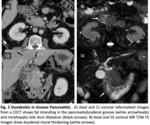
“Groove pancreatitis” is a form of a disease that involves a potential space between the pancreatic head,
the duodenum and the terminal common bile duct called the pancreatoduodenal groove.
The typical clinical scenario is a middle-aged male alcoholic with abdominal pain and nausea.
(4) This entity has been divided into two forms.
The pure form affects only the pancreatoduodenal groove and appears as inflammatory changes or soft tissue in the groove with a “sheet-like” shape and thickening of the medial duodenal wall with a small cyst.
The segmental form extends into the pancreatic head and shows as mass-like enlargement of the pancreatic head,
differentiating from a pancreatic mass can be very difficult.
In both forms,
the common bile duct can appear attenuated and narrowed.
(8) Fig. 5
2.2 Duodenal Ulcer
Peptic ulcer disease refers to the development of gastric or duodenal mucosal defects which penetrate through the muscularis mucosa.
(9) Duodenal peptic ulcer usually occurs in the bulb.
(2) Postbulbar ulcers are rare,
and when they occur,
causes such as Crohn disease and Zollinger-Ellison syndrome should be considered.
(5)
Findings. Fig. 6
- Crater-like collections of barium that persist despite paddle compression and peristaltic motion.
(4)
- Exophytic wall thickening with associated oedema.
(4)
Upper gastrointestinal studies should be made with water-soluble contrast agents.
The most frequent complication is bleeding.
Perforation is seen as extraluminal gas or coral contrast,
periduodenal fluid and wall thickening.
(2) Fig. 7
3.0 Vascular Disorders
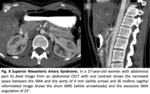
3.1 Superior Mesenteric Artery Syndrome
Is characterized by compression of the horizontal portion of the duodenum between the superior mesenteric artery (SMA) and aorta and causes a subacute or recurrent obstruction.
The principal underlying cause is the loss of retroperitoneal fat tissue.
(2)
The SMA arises at the L1-L2 level and forms an angle with the aorta (AMA).
Usually,
the third portion of the duodenum is surrounded by fat which maintains a wide AMA and AMD (aorto-mesenteric distance).
The normal range is 28°– 65° and 10-34 mm respectively.
The common presentation is females between 10-39 years with postprandial epigastric pain and fullness,
nausea,
vomiting,
weight loss,
and anorexia.
(10)
Findings.
(2,4,10) Fig. 8
- Upper gastrointestinal barium study: Dilated stomach and proximal duodenum a vertical extrinsic impression on the third portion of the duodenum.
- Angio-CT: AMA 6°-22° and AMD 2-8 mm,
transverse compression and proximal dilatation.
3.2 Duodenal Bleeding
Upper gastrointestinal bleeding is more frequent in men and affects younger patients.
Presents proximal to the ligament of Treitz.
Upper endoscopy is the first-line tool for diagnosis and treatment.
In 14% it can not identify a specific cause.
Catheter angiography and surgery are options for patients with life-threatening bleeding and should be used as a therapeutic procedure.
The principal cause of bleeding in the duodenum is peptic ulcer disease and duodenitis.
(11)
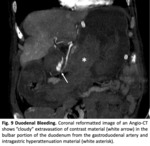
Findings. Fig. 9
- NECT (Recent bleeding): Intraluminal hyperattenuation material,
unclotted extravascular blood has an attenuation of 30-45 UH and clotted blood has 45-70 UH.
- Angio-CT (Active bleeding): Intraluminal extravasation of contrast,
changing the appearance of the site of extravasated contrast material from arterial to portal-venous phase.
The bleeding can adopt different shapes: jetlike,
linear,
“cloudy”,
pooled.
Fig. 10
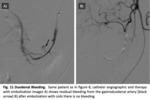
CT angiography detects active bleeding with a rate that exceeds 0.3-0.5 mL/min,
catheter angiography detects 0.5 mL/min and scintigraphy with 99mTc-labeled red blood cells detects active bleeding at a rate higher than 0.1 mL/min.
(11) Fig. 11
3.3 Ischemic Duodenitis
Ischemic duodenitis caused by splanchnic arterial insufficiency it is a very rare entity because of the rich collateral blood supply.
It needs at least two of three main splanchnic arteries occluded or severely stenosed by atheromatous disease.
(2) Smoking,
hypertension and atherosclerotic vascular diseases can be major risk factors.
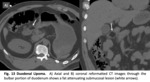
Findings. Fig. 12
- CECT: Segmental thickening of the duodenal wall,
lack of mucosal enhancement,
submucosal hyperaemia,
pneumatosis intestinalis and gas in the mesenteric or portal veins.
4.0 Benign Neoplasm
4.1 Duodenal Lipoma
Are solitary,
slow-growing,
benign mesenchymal duodenal mass-forming tumors that contain adipose tissue.
The duodenum is the third common location,
following colon and ileum.
Can present as a submucosal or intraluminal mass,
if large can show necrosis,
calcifications or cystic degeneration and ulceration leading to acute or chronic anemia (1,12)
Findings. Fig. 13
- Barium meal: smooth,
oval or spherical mass with very distinct margins.
- CT: Fat content (-100 to -50 UH) oval or round submucosal mass.
- MR: High signal intensity on T1 and T2-weighted images,
drop in signal intensity on fat-suppressed sequences.
5.0 Malignant Neoplasm
5.1 Duodenal Adenocarcinoma
Adenocarcinomas are tumors of the glandular epithelium.
They are the most common primary malignancy of the small bowel and the majority occur in the duodenum,
represents up to 80-90%.
(1,13) The peak prevalence is in the 7th decade,
patients present with signs of bleeding,
jaundice,
or obstruction.
(5) 50% or more has metastases at the time of the diagnosis.
(4,5)
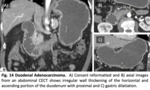
Findings. Fig. 14
- CT: Soft-tissue polypoid mass or an asymmetric thickening with irregular borders or ulceration.
Short segment involved,
mild,
heterogeneous and late enhancement.
- MR: Infiltrative lesions,
causing stenosis and obstruction.
Post-gadolinium demonstrates heterogeneous and moderate enhancement.
Stage liver metastases,
lymph node involvement,
and peritoneal carcinomatosis.
5.2 Duodenal Lymphoma
Gastrointestinal lymphoma accounts for 5-20% of extranodal lymphomas,
the stomach is the most common site,
the duodenum only represents the 6-8%.
Most frequently occur in the sixth decade of life,
they are rare in childhood,
but it is the most common gastrointestinal tumour in this age.
(14) The most frequent type in the duodenum is non-Hodgkin T-cell lymphoma.
(1)
They are five patterns of small bowel lymphomas:
- Polypoid: Homogeneous submucosal,
solid nodule.
- Infiltrative: Segmental infiltrating lesion with a medium diameter of 1.5-2 cm,
with mild circumferential thickening of the wall.
- Aneurismal: Dilatation of the lumen >4cm.
- Stenosing: Concentric fibrotic stenosis.
- Mesenteric: Development of lymphoid tissue outside the intestinal wall.
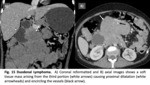
Barium studies may show single or multiple polypoid lesions,
diffuse or segmental ulcerative.
At ultrasound,
these tumors are hypoechoic and shown circumferential wall thickening.
(15) Lymphadenopathy and splenomegaly are suggestive features.
(1) Fig. 15