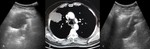
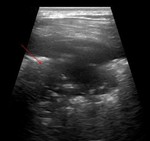
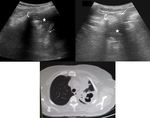
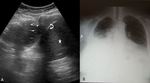
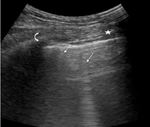
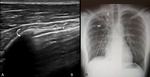
Normal lung appearance
When performing a thoracic ultrasound,
structures explored are skin,
subcutaneous tissue,
intercostal muscles,
endothoracic membrane and the pleura (parietal and visceral pleura).
Several sign have been described:
1. Pleural line- the interface between the soft tissue structures and the air in the lung; it is an echogenic line measuring < 3 mm.
2. Sliding sign or ‘sliding lung’- the pleura that glides during respiratory movements.
The presence of the sliding sing rules out pneumothorax at that site.
Lung sliding generates the seashore sign in M-mode.
3. A lines- horizontal hyperechoic repetitious lines,
representing dry interlobular septa and normal aeration.
The predominance of A pattern has 67% sensibility and 90% specificity for pulmonary artery wedge pressure <= 13 mmHg [1].
A line pattern suggests that fluids can be given without the concern for pulmonary edema.
4. B lines or comet tail artifact- vertical hyperechoic reverberations extending from the pleural line.
In normal lung there are no more than three B lines per costal space.
A predominance of B lines bilaterally indicates fluid in the interlobular septa,
suggesting interstitial edema or pulmonary edema.
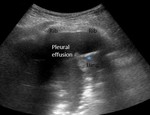
Pleural effusion
Effusion is seen as well demarcated,
echo-free fluid accumulation,
that displaces the pleural line.
Two types of signs have been described:
1.
quad sign: appears in free pleural effusions; it is the image formed by pleural line,
lung line and rib shadows.
2.
sinusoid sign: indicates free pleural effusion with low viscosity; it appears when the effusion moves with the position of the patient [2].
The fluid may be:
- anechoic: transudate
- complex nonseptate: transudate or exsudate
- complex septate: empyema
- echoic: haemothorax
The accuracy of chest ultrasound is higher than bed chest radiography in detecting pleural effusion [3].
Actually,
in the upright position,
chest radiography can detect pleural effusion only when the volume of fluid is higher than 200-300 mL; in supine position,
the sensitivity of chest radiography is even smaller.
Unlike chest radiography,
ultrasound can detect pleural effusions as small as 20 ml.
Pneumothorax
Key features in pneumothorax are:
1. Absence of lung sliding and B lines– highly suggestive for pneumothorax.
However,
lung sliding can also be absent in pleural effusions,
pleural adhesions,
chest tubes or advanced COPD.
In these situations,
the sky-ocean-beach sign can be appreciated,
whereas in pneumothorax,
the stratosphere sign is present in M-mode.
2. Stratosphere sign- representing pneumothorax,
in M-mode; the sky-ocean-beach sign or seashore sign represents the normal lung.
3. Lung point- the interface between normal lung and pneumothorax.
It a specific sign for pneumothorax.
The diagnostic accuracy of chest ultrasound is higher than supine chest radiography in the diagnosis of pneumothorax [4] [5].
Lung consolidation
Consolidation of the lung means loss of air in the alveoli and can be due to:
-pneumonia: which appears as hypoechoic lesion with ill-defined margins.
There may be present fluid bronchogram- numerous,
small hyperechoic lines within the consolidated lung parenchyma,
representing fluid-filled bronchi.
Ultrasound is a reliable diagnostic tool for detection of pneumonia when CT chest imaging is used as gold standard [6].
-atelectasis: can be easily detected on ultrasound.
It has an homogenous pattern similar to liver parenchyma.
-pulmonary neoplasm: appears as solid,
hypoechoic lesions with ill-defined margins and can be easily detected in peripheral locations.
Hyperechoic or anechoic patterns can also be seen due to necrosis.
Important to note- pulmonary abscesses cannot be distinguish from pulmonary neoplasm undergoing central necrosis.
However,
ultrasound is a good image tool for transthoracic biopsy.
Interstitial syndrome and pulmonary edema
Interstitial syndrome is defined by the presence of three or more B lines between two ribs,
generating the lung rockets sign.
In interstitial syndrome,
the distance between the B lines is 7 mm (the anatomic space between interlobular septa),
while in pulmonary edema the distance between two B lines is 3 mm ( the anatomic space between alveoli).
Ultrasound-guided pleural and pulmonary procedures
Ultrasound can be an excellent image guide for thoracentesis,
chest tube placement,
abscess drainage,
pulmonary biopsy.
The diagnostic accuracy rates for transthoracic ultrasound guided biopsy varies between 85-95 %.
The complication rate is less than 1%,
with pneumothorax being the most frequent complication,
followed by mild hemoptysis [7].
The BLUE-protocol
The Bedside Lung Ultrasound in Emergency protocol,
designed by French intensivist Daniel Lichtenstein,
is a fast protocol that allows the diagnosis of acute respiratory failure.
The BLUE protocol includes eight profiles that allow the rapid diagnosis of the main causes of dyspnea: pulmonary edema,
COPD and asthma,
pulmonary embolism,
pneumothorax and pneumonia.
1.Pulmonary edema: B profile- lung sliding with lung rockets.
2.COPD and asthma: A profile with no DVT and no PLAPS (posterolateral alveolar and/or pleural syndrome).
3.Pulmonary embolism: A profile- anterior lung sliding with predominant A lines associated with deep venous thrombosis.
4.Pneumothorax: A’ profile- absence of lung sliding with A lines; lung point.
5.Pneumonia: B’ profile- absence of lung sliding with anterior lung rockets.
- A/B profile: unilateral lung rocke
- C-profile: anterior lung consolidation
- A-no-V-PLAPS profile