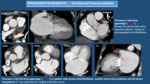
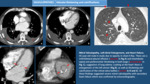
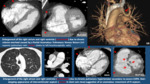
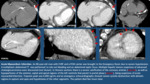
Systematic analysis of heart images is mandatory.
We start looking to axial images,
searching abnormalities in different cardiac structures. Points to Check in CT heart images Fig. 2.
If we find signs suspicious of cardiac pathology (especially in cases of possible abnormalities in the myocardium,
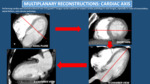
septal defects or valvular pathology) we recommend to reconstruct images in the different cardiac axis for better visualization.
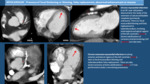
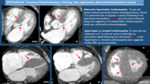
Multiplanar Reconstructions.
Fig. 3
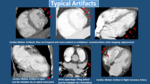
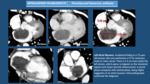
As these studies are not ECG-gated CT there will be many movement artifacts that can obscure images and lead to misinterpretation,
so we have to be aware of the most usual aspects of these artifacts. Typical Artifacts.
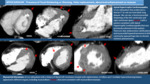
Fig. 4.
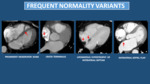
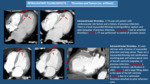
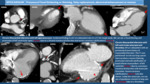
Frequent normality variants can also lead to misinterpretation and we have to be familiar with them. Frequent Normality Variants.
Fig. 5
Besides the presence of artifacts,
looking at the heart in a non-gated CT has two major inconveniences: 1) We don´t know in which part of the cardiac cycle the heart has been imaged is and 2) We can´t see cardiac movement nor assess cardiac function.
Due to these factors,
sometimes we won’t be able to make a precise diagnosis,
raising only a diagnostic suspicion that has to be confirmed or ruled out with other imaging techniques (Echocardiography,
Cardiac MRI or Cardiac ECG-gated CT).
Now we will review some of the most frequent and relevant imaging findings of heart diseases using the systematic approach described in Fig. 2 Points to Check in CT heart images and focusing on clinical cases.
Unfortunately,
a complete review is beyond the scope of this poster (we address the reader to the poster references for further information).
SYSTEMATIC ANALYSIS OF HEART IMAGES
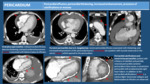
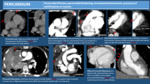
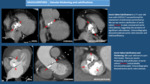
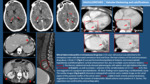
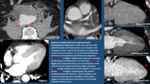
PERICARDIUM: Look for pericardial effusion and its amount,
the presence of pericardial thickening (and if it is smooth or irregular),
the presence of increased pericardial enhancement and presence of pericardial calcifications or masses.
- Acute Pericarditis: it is seen as mild or moderate pericardial effusion,
usually associated with mild pericardial thickening and increased enhancement.
Acute viral pericarditis can be accompanied by bilateral pleural effusion (pleuro-pericarditis).
Examples are shown in Fig. 6.
- Pericardial Calcifications: they are sequels of previous pericarditis,
trauma or previous surgery (Fig. 6).
If there are signs of heart failure it´s highly suggestive of constrictive pericarditis.
- Pericardial Metastasis: it is the most frequent localization for cardiac metastasis (context of disseminated neoplastic disease).
They can be seen as a nodule or as an irregular pericardial thickening (Fig. 7).
- Pericardial Cysts: cystic image in contact with pericardium.
They are benign,
frequent and usually located on the right side (Fig. 7).
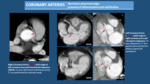
CORONARY ARTERIES: Check the normal origin of coronary arteries and the presence of coronary arteries calcifications.
- Origin of Coronary Arteries: Left Coronary Artery (LCA) must arise from left coronary sinus and Right Coronary Artery (RCA) must arise from right coronary sinus,
otherwise there is an abnormal origin of a coronary artery (Fig. 8).
Those which have an inter-arterial course (between ascending aorta and pulmonary artery) are related to an increased risk of myocardial infarction and sudden death.
- Coronary Arteries Calcifications: atheromatosis is the unique cause of calcium deposition in coronary arteries,
so its presence and amount are related to coronary disease (Fig. 9).
Occasionally we can also detect soft or mixed plaques (=non or only partially calcified atheromatosis).
Unfortunately,
grading of coronary stenosis cannot be assessed with conventional CT.
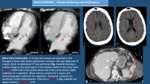
INTRACAVITARY FILLING DEFECTS: If the study is an intravenous contrast-enhanced CT we have to make sure that there are no intracavitary filling defects.
This could be the appearance of intracardiac thrombus (frequent) and cardiac tumors (infrequent).
- Linear filling defect in the left atrium (Artifact): it is an incomplete iv.
contrast opacification of left atrium that mimics a thrombus (Fig. 4).
Its linear morphology and the fact that disappears in a delayed scan (complete opacification) allow to differentiate it from a thrombus.
- Left Atrial Thrombus: it is seen as an irregular filling defect (that do not resolve in a delayed scan).
Its associated with atrial fibrillation and enlarged left atrium (Fig. 10 y Fig. 11).
The most frequent location is inside the left atrial appendage.
- Ventricular Thrombus: it is seen as a nodular or crescent-shape filling defect.
It usually appears attached in an akinetic/dyskinetic zone due to prior myocardial infarction (Fig. 13).
- Myxoma: it is the commonest cardiac tumor and it’s benign.
It can be seen as an intracavitary round or nodular shaped mass and it’s more frequent location is left atrium,
being attached to the interauricular septum (Fig. 12).
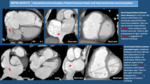
VALVULOPATHIES: Check the presence of valvular calcifications and thickening.
They are more frequently observed in:
- Aortic Valve: Calcification of aortic valves is usually due to degenerative or rheumatic etiology and is strongly related to valvular stenosis.
(Fig. 14).
In aortic valve stenosis,
concentric hypertrophy of left ventricle and dilation of the ascendant aorta can also be seen.
- Mitral Valve: Calcification of mitral valves can be seen in rheumatic etiology.
Enlargement of left atrium can be seen if there is mitral insufficiency (Fig. 15).
Calcification of mitral annulus can also be seen but is usually asymptomatic.
- Endocarditis: In clinical scenarios where endocarditis is possible,
look for the presence of nodular imaging in cardiac valves (= vegetation).
This finding is more consistent if is seen in two different phases of the study (i.e.
arterial and portal phases) and if it is associated with systemic embolism (in case of involving left cardiac valves) or bilateral cavitated and randomly distributed lung nodules (in case of involving right cardiac valves).
Fig. 16 and Fig. 17.
SEPTAL DEFECTS: Check the continuity of atrial and ventricular septum.
- Atrial Septal Defect: congenital focal discontinuity of atrial septum.
There are many subtypes but the commonest is Ostium Secundum type,
accounting for 70-80% (Fig. 18).
If significant can be associated with right ventricle enlargement due to chronic volume overload (better seen when we compare right and left ventricular diameters in a short axis view).
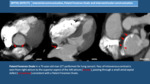
- Patent Foramen Ovale: lack of closure of foramen ovale.
It is seen as a tiny communication between the right and left atrium.
Its detection can be easier if we see some contrast from right atrium passing to the left atrium through the communication (Fig. 19).
CAVITY ENLARGEMENT: Look for a dilated cardiac cavities.
- Left Atrial Enlargement: is a risk factor for atrial fibrillation and can also be seen in mitral insufficiency.
We can use a cut-off value of approximately 7 cm of transverse diameter to diagnose enlargement12.
Fig. 20
- Left Ventricular Enlargement: it can be seen in cases of dilated cardiomyopathy and valvular disease.
We can use a cut-off value of 5.6 cm measuring the internal diameter of the left ventricle to diagnose enlargement11.
Fig. 21
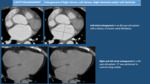
- Right Ventricular Enlargement: it can be seen in pulmonary hypertension (Fig. 22 and Fig. 23),
left to right shunts (Fig. 23 and Fig. 18) and right ventricle cardiomyopathies (rare).
The right ventricle is enlarged if its transverse diameter is greater than left ventricle (this is better assessed in short axis view).
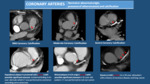
MYOCARDIUM: Look for focal thickening or thinning,
presence of subendocardial fat in the left ventricle,
abnormal enhancement or cardiac masses.
- Chronic Myocardial Infarction: it is seen as focal myocardial thinning in coronary artery dependent territory.
It can be associated with subendocardial fatty replacement,
mural calcifications,
and coronary artery calcifications (Fig. 24).
Occasionally,
ventricular aneurysms can also be seen (Fig. 25).
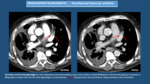
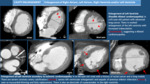
- Acute Myocardial Infarction: it can be seen in iv contrast-enhanced CT as a perfusion defect in coronary artery dependent territory (Fig. 26 and Fig. 27).
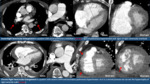
- Hypertrophic Cardiomyopathy (HCM): usually consists in asymmetric hypertrophy of left ventricular walls (septal thickness equal or more than 15 mm).
There are few different patterns (excellently described in the article in reference 17) but they usually involve the interventricular septum.
Here we show cases of an incidental diagnosis of Obstructive HCM in Fig. 28 and Apical HCM in Fig. 29
- Amyloid Cardiomyopathy: can be seen as increased thickness of ventricular walls and is a differential diagnosis of HCM (Fig. 28).
- Myocardial Metastases: can be seen as nodular masses in the myocardium in the setting of disseminated neoplastic disease.