First,
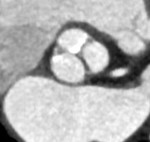
evaluation of the aortic valve should begin with confirmation of the aortic valve morphology (Fig.1),
differentiating tricuspid from bicuspid valvular anatomy.
The accuracy can be further improved with additional systolic reconstruction using ECG-gating,
which permits differentiation between a bicuspid valve with raphe and a tricuspid valve [1].
Next,
the assessment of the extent and location of the aortic valve calcification is important (Fig.1): very bulky calcification at the edge of native valvular leaflets has been related to increased risk of coronary occlusion when it is displaced over the coronary ostium [2].
Furthermore,
heavy calcification in the sinotubular junction may cause restriction during balloon expansion at the aortic end,
causing ventricular displacement of the device at the time of deployment [3].
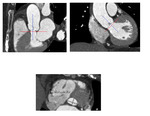
Rigorous evaluation of the aortic valve annular dimension is basic for appropriate selection of prosthesis size (Fig.2). The aortic annulus is defined at the lowest attachment point of the aortic valve leaflets within the left ventricle (LV),
forming a virtual ring,
which is not circular but oval in shape. MDCT permits reconstructions in unlimited planes,
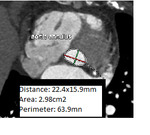
allowing multiple measurements of the aortic annulus: minimum (Dmin),
maximum (Dmax) and mean diameters (Fig.3) [4,5]. This step is critical as inaccurate sizing will result in undesirable periprocedural consequences such as prosthesis migration,
significant aortic regurgitation (if undersized) or rupture of the aortic root (if oversized). Currently,
the Edwards SAPIEN XT device is available in three sizes: 23mm,
26mm and 29mm [6],
the Medtronic CoreValve system has four sizes: 23mm,
26mm,
29mm and 31mm [7].
In addition,
the assessment of the dimensions of the sinus of Valsalva,
sinotubular junction and ascending aorta is an essential step in the pre-procedural evaluation.
Using the ‘‘center-line approach’’ and reformations of the aortic root and ascending aorta,
MDCT permits accurate measurement of these dimensions.
Moreover,
the 3D analysis of MDCT permits comprehensive and detailed evaluation of the spatial relationship of the aortic valve with the surrounding structures.
In particular,
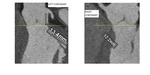
the information on the height of the coronary ostia relative to the aortic annular plane is important to ensure patency of the coronary arteries following ballooning and deployment of the transcatheter prosthesis (Fig.4).
Finally,
evaluation of the peripheral access artery and aortic anatomy is fundamental to plan the procedural strategy: retrograde (through a transarterial approach,
transfemoral or transsubclavian) or antegrade (through a transapical approach). Typically,
the curved multiplanar reformation planes (MPR),
using the ‘‘center-line approach’’,
permits reconstruction of the curved planes,
following the course of the vessel regardless of its tortuous course.