MDCT Procedure Details:
Computed Tomography has a vital role in diagnosing congenital vascular anomalies.
For CT pulmonary angiography (CTPA) and cardiac anomaly CT examinations,
scan is performed from lung apex till level of adrenals with a large field of view.
A 1.25-mm collimation should be used,
which can be reconstructed at 0.75- 1 mm intervals with a targeted field of view.
A pitch of 3 or 6 is required depending on the the patient's ability to hold their breath.
Average of 120 mL of nonionic contrast material is injected at a rate of 4-5 mL/sec depending on the weight of patient.
For patients with known altered cardiac output,
a timing bolus (150) targeted to the region of interest (main pulmonary artery) is helpful to optimize vascular opacification.
Depending on the abnormality,
arterial and venous phase imaging can be performed through the same structure to characterize blood supply and drainage.
Volumetric imaging data can be reconstructed using algorithms such as shaded surface display,
maximum intensity projection,
or volume rendering,
which aid in vessel evaluation.
All images in this exhibit are from CT scans performed on 128 slice MDCT Toshiba scanner at Rehman Medical Institute.
Submm images were reviewed on state of the art vitrea workstations.
Congenital Pulmonary vascular anomalies:
Pulmonary vascular anomalies are divided into two main categories:
1.
Pulmoanry arterial anomalies.
2.
Pulmonary venous anomalies.
1.
PULMONARY ARTERIAL ANOMALIES:
Pulmonary arterial anomalies are mostly related to agensis of a part or whole of the pulmonary arterial system.
Cardiothoracic surgeons are interested to know the level of pulmonary stenosis and the status of central arteries for consideration of shunting.
Pulmonary stenosis is mostly associated with other cardiac congenital anomalies,
commonest is Tetrology of Fallots.
Pulmonary arterial anomalies diagnosed on CT angiography are:
◊ Pulmonary Stenosis:
Pulmonary artery stenosis can occur anywhere,
from the subvalvular RVOT and pulmonary valves to the peripheral pulmonary arteries,
and may be solitary or multiple.
Pulmonary artery stenosis may be isolated (20%),
but it is often associated with cardiac anomalies such as atrial septal defect (ASD) and perivalvular pulmonic stenosis.
Pulmonary artery stenosis is associated with syndromes like Williams syndrome,
Down syndrome,
Ehlers-Danlos syndrome etc.
Pulmonary stenosis can be unilateral or bilateral.
Main pulmonary artery Stenosis:
This can be seen at subvalvular level (RVOT stenosis),
valvular level (seen as thickening of pulmonary valves on CT images) and supravalvular level in pulmonary trunk.
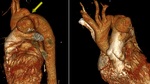
- Supravalvular pulmonary stenosis:
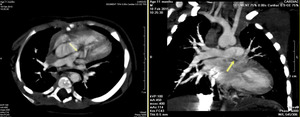
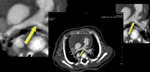
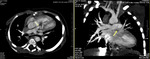
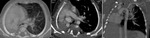
Fig. 2: Multiplanar CT Angiography images showing Pulmonary stenosis at supravalvular level
-------------------------------------------------
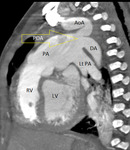
- Pulmonary valvular and RVOT stenosis:
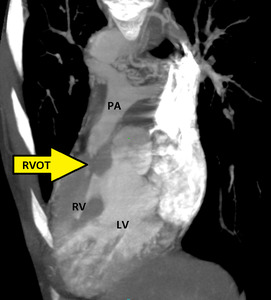
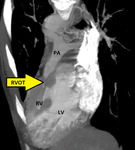
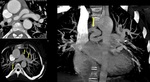
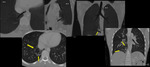
Fig. 3: Curved MPR CT image of a cardiopulmonary angiogram showing hypertrophy of right ventricle (RV) and severe stenosis of right ventricular outflow tract (RVOT) seen (arrow). PA=pulmonary artery, LV=left ventricle, RVOT=right ventricular outflow tract.
----------------------------------------
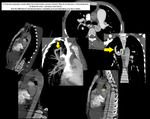
- Pulmonary stenosis in Tetrology of Fallots with Situs inversus:
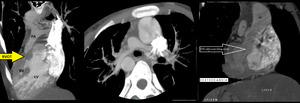
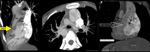
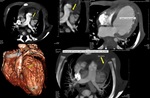
Fig. 4: Situs inversus with dextrocardia and Tetrology of Fallots. Myltiplanar reformatted CT images showing Tetrology of Fallots i.e. Pulmonary stenosis at valvular and subvalvular level, hypertrophied RV, VSD with overriding of aorta. There is hypoplastic right pulmonary artery. Situs inversus seen with dextrocardia. Multiple collaterals seen along central pulmonary arteries.
----------------------------------------
◊ Pulmonary agenesis:
Pulmonary agenesis is complete absence of pulmonary artery.
It can be unilateral or bilateral.
Absent Pulmonary valve:
Absent Pulmonary Valve Syndrome (APVS) is a rare variant and makes up about 3-6% of patients of Tetralogy of Fallot (ToF).
Apart from the hallmark features of ToF,
these patients have an absent / rudimentary pulmonary valve,
leading topulmonary regurgitation during foetal life,
causing aneurysmal dilatation of pulmonary vessels,
compressing the trachea or the main stem bronchi.
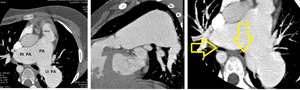
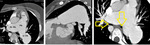
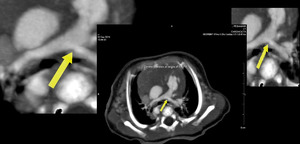
Fig. 7: Multiplanar CT images of 11 year old girl showing marked aneurysmal dilatation of central pulmonary arteries associated with absent / rudimentary pulmonary valve and focal pulmonary stenosis at valvular level. Dilated pulmonary arteries are causing significant airway compression on mainstem bronchi (arrows).
----------------------------------------------
Anomalous origin of Coronary artery from pulmonary artery (ALCAPA)
Coronary artery can have anomalous origin from pulmonary artery,
usually at the supravalvular trunkal level.
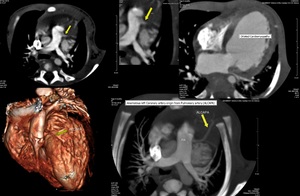
Fig. 8: Multiplanar images of Cardiac CT scan showing anomalous origin of left coronary artery from pulmonary artery (ALCAPA). There is secondary left ventricular dilatation and cardiomyopathy.
---------------------------------------------
◊ Pulmonary artery aneurysm:
Pulmonary artery dilatation can be seen due to a number of congenital causes e.g.
cardiac shunts,
PDA,
valvular atresia or fistulas.
- Large functional PDA presenting with pulmonary artery aneurysm:
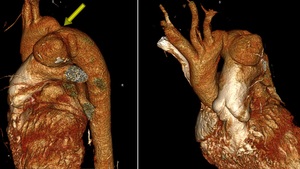
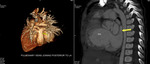
Fig. 9: 3D Volume rendered images from a CT angiogram showing large functional PDA presenting with pulmonary artery aneurysm.
--------------------------------------------
- Large PDA and pulmonary artery aneurysm in aortic coarctation / interrupted arch variant:
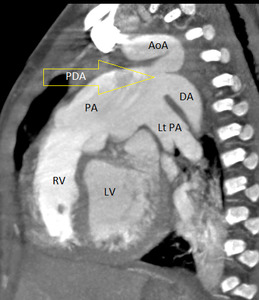
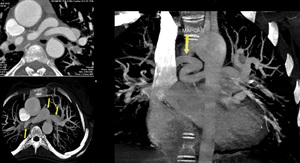
Fig. 10: Aneurysmal dilatation of pulmonary artery due to a large PDA (arrow). There is coarctation / interrupted aorta variant and PDA is acting as a conduit between arch and descending aorta.RV=right ventricle, LV= left ventricle, PA= pulmonary artery, DA=descending aorta, AoA=aortic arch, LtPA= left pulmonary artery.
---------------------------------------
- Bronchial artery-Pulmonary artery Fistula causing Pulmonary hypertension:
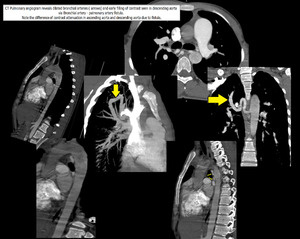
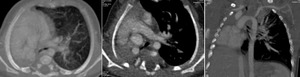
Fig. 11: Multiplanar images of CT Pulmonary angiogram showing Bronchial artery - pulmonary artery fistula, presented as pulmonary arterial hypertension.
--------------------------------------------
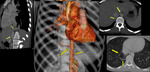
◊ Pulmonary sequestration:
Bronchopulmonary sequestration is a congenital malformation in which a segment of nonfunctioning lung is isolated from the normal airways and receives its blood supply from a systemic artery.
It is classified as intralobar (in the visceral pleura of normal lung) or extralobar (in a separate pleural envelope).
Sequestrations can be accurately diagnosed on contrast-enhanced CT by seeing a feeding vessel from the aorta.
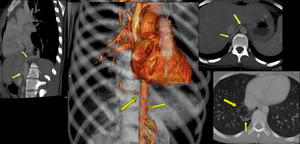
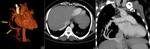
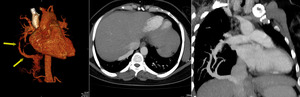
Fig. 12: Sequestration. Multiplanar and 3D volume rendered images showing intralobar pulmonary sequestration. Arrows along the vessel point at the anomalous supply from infra-diaphragmatic part of aorta. Lung window image reveals patch of nodules and atelectasis in right lower lobe medially (arrows)
----------------------------------------
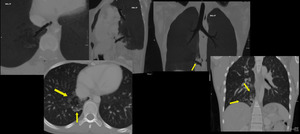
Fig. 13: Sequestration: Multiplanar lung window images showing intralobar pulmonary sequestration. Accessory bronchus seen in the sequestration abutting the esophagus, better visualized on Min-IP images
---------------------------------------
◊ Pulmonary arteriovenous malformation:
Abnormal direct communication between pulmonary arteries and veins can be an isolated lesion in or associated with arteriovenous malformations involving the skin,
mucous membranes,
and other organs known as hereditary hemorrhagic telangiectasia or Oslar-Weber-Rendu syndrome.
Small arteriovenous malformations may be asymptomatic and incidentally found on MDCT.
However,
as the size and number of lesions increase,
patients are at risk for hypoxemia,
cyanosis,
and paradoxical emboli.
PULMONARY VENOUS ANOMALIES:
These are mostly related to anomalous return to heart; can be partial or total anomalous venous return. Anomalous pulmonary venous drainage occurs when pulmonary venous blood enters the systemic circulation or the right heart
Total anomalous pulmonary venous return (TAPVR):
Bilateral pulmonary veins join to form a single channel and can drain into SVC (supracradiac type),
Right atrium ( cardiac type) or into IVC ( infracradiac type).
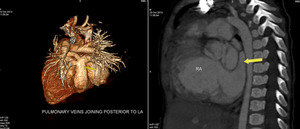
Fig. 14: TAPVR. 3D volume rendered and sagittal oblique reconstructed image from a CT angiogram reveal total anomalous pulmonary venous return (TAPVR). Bilateral pulmonary veins are joining to form a single channel posterior to Left atrium of heart, which opens into the right atrium near opening of coronary sinus.
------------------------------------------
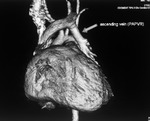
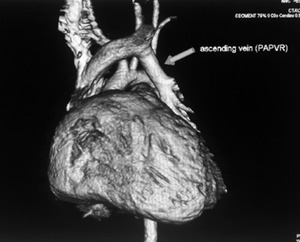
Partial anomalous pulmonary venous return (PAPVR):
Segmental,
lobar or unilateral pulmonary veins drain either into SVC,
IVC or right atrium.