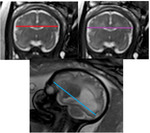
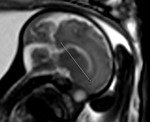
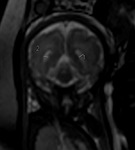
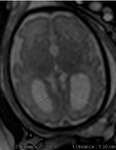
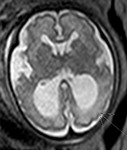
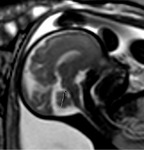
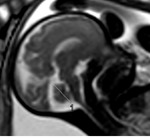
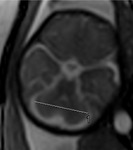
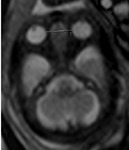
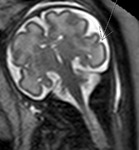
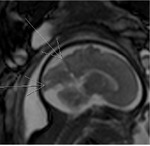
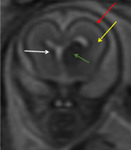
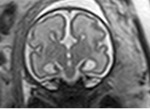
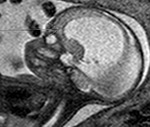
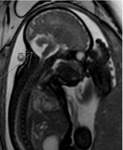
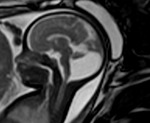
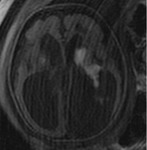
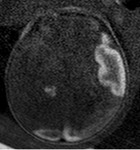
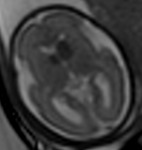
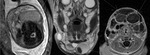
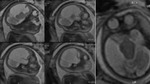
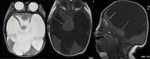
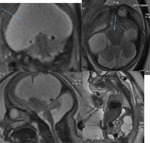
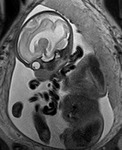
INDICATIONS OF THE FOETAL MRI
The strongest indications are the following:- Fetus: Abnormalities of the posterior fossa,
middle or midline cranial fossa,
ventricular space (ventriculomegaly,
ventricular cysts,
congenital infections,
alterations in cortical development,
myelomeningocele,
etc).
Maternal obesity,
multiple pregnancy,
oligohydramnios,
family history of genetic disorders,
coagulopathies,
extension study for anomalies that are usually associated,
etc.
ADVANTAGES AND LIMITATIONS:
Advantages:
-With multi-channel type receiving antennas we will obtain a high spatial resolution.
-Acceptable tissue characterization.
-Larger field of vision than ultrasound,
and in addition to seeing the fetal anatomy,
can also study the placental anatomy and surrounding tissue structures of the mother.
Inconvenients to consider:
-Unavoidable fetal movement (in some cases,
a small dose of sublingual lorazepam is given upon entry of the mother into the Resonance team).
Some authors recommend sedation.
In cases of short gestational age (mainly in studies performed below 20-23 weeks of gestation),
we will have a suboptimal spatial resolution.
-In women with gestation already in advanced stages,
there may be real physical discomforts.
-Maternal claustrophobia.
-If the mother present some implanted element that is not compatible with the magnetic resonance.
TECHNIQUE:
High field MRI (1.5 T).
Maternal-fetal exposure to higher magnetic fields is not accepted.Multi-channel body antennas are used.
The entrance of the patient can be caudo-cranial or cranio-caudal.The patient can be placed in the supine or lateral position (in advanced pregnancies the left lateral decubitus is preferred,
to avoid compression of the inferior vena cava).
In gestations outside the first trimester,
it is preferable to carry out the study after 20 weeks.bUsually fasting is not necessary.
Sometimes a fasting of about 4 hours is recommended to decrease intestinal peristalsis,
although it is true that in some cases maternal fasting can cause greater fetal irritability.
Ultrafast sequences are used to counteract fetal movement.These studies are not made with contrast,
in the absence of evidence of safety of gadolinium contrasts,
the passage of gadolinium chelates,
with a route that passes to the fetal bladder through the placenta,
and then to the amniotic fluid,
with a reasonable risk of nephrogenic systemic fibrosis.
STUDY PROTOCOL:
-Ultra-fast sequences.
-It is necessary to make 3 orthogonal planes to the mother,
and on these planes the axial,
coronal and sagittal sections of the fetus are planned,
always using as reference the last sequence used to plan the next one,
due to predictable fetal movements.
-Axial,
coronal and sagittal bFFE locators.
T1 WATS,
FSE Sshot T2 +/- GRAD T2 *,
FLAIR; Other possible protocol is one based on ultra-fast sequences with T2 (SSFSE T2),
T1 (EG-3D),
EG and DWI enhancement.
-Parameters normally used: Matrix 300,
FOV of about 40cm,
and a Thickness / Distance ratio of 3 to 4.
DWI with b = 0 and b = 1000.
-The b-FFE sequences produce a sequence of pulses of gradient echoes without refocus pulses of 180 °,
and the b-FFE value will provide us with a very strong signal for tissues with a high T2 / T1 ratio.3D T1-FFE → we will obtain a lot of very thin cuts,
with high signal strength in short times,
and we can also perform multiplanar reconstructions.
FFE causes artifacts.
However,
the FFE sequences present artifacts,
although this does not have to be bad: As these sequences are sensitive to susceptibility artifacts,
we can examine the presence of haematic material (hemosiderin deposits) if the blood material is old.
-To avoid water-fat misalignment artifacts: TE=value in phase.
-The sequence enhanced in T1 is useful for characterization of: bleeding,
calcium clusters,
fat.
THE PROPOSED RADIOLOGICAL REPORT:
-Clinical information.
-The justification for carrying out a fetal MRI should be included,
if this is not the case,
the applicant should be contacted.
-Image acquisition protocol: Name the sequences used.
If the study could not be completed,
specify why.
If some sequence presents images with artifacts of movement or another type,
it must also be described before transcribing the findings in image.
-Evaluate the presence of calcifications or bleeds/microbleeds (echo-gradient sequences will be useful for this).
-Evaluate the ventricular size (the atria are usually measured in the coronal or axial plane,
although in cases in which the ventricular size is pathological,
it is preferable to take several measurements).
-Presence of septum pellucidum / cavum vergae,
or cysts.
-Evaluation of the periventricular area (subependymal heterotopias,
germinal matrix hemorrhages,
subependymal nodules,etc).
-Interhemispheric line (arachnoid cysts,
pineal cysts,
etc).
-Assess presence or absence of corpus callosum and development of posterior fossa structures.
In case of posterior fossa anomalies,
the spine must be evaluated in great detail,
looking for associated anomalies.
-Evaluation of myelination (whether or not according to gestational age).
-Evaluation of the rotation/sulcation (if it is according to gestational age or not).
-Analysis of neuronal migration.
-Signal intensity of the cerebral parenchyma,
cerebellar and brainstem.
-Biometric study:
- Biparietal bone diameter (BBD).
Distance between both internal tables,
measured in coronal plane.
- Biparietal cerebral diameter (BCD).
The largest cerebral transverse diameter,
in coronal plane,
at the same level as the bone diameter.
- Pericerebral space: It is BBD-BCD.
It decreases as the gestational age advances.
- Cranio-cerebral index.
It is BBD-BCD/BBD.
- Cephalic index.
It is the relation between the short axis and the long cerebral axis obtained in the plane in which the biparietal diameter is measured.
- Fronto-occipital diameter.
Measured in sagittal plane.
- Atrial diameters (usually the ventricular atrium is the largest portion of the ventricular system).
- Length of the corpus callosum from knee to splenius.
- Size of the posterior fossa,
with the following measures: Maximum AP diameter in vermis; Maximum CC diameter in vermis; Maximum cerebellar transverse diameter; Area of the vermis (in sagittal plane).
BIOMETRIC STUDY:
Cephalic index:
- Dolichocephaly (IC <74).
- Brachycephaly (IC> 84).
Ventricular size: Assess the asymmetry / ventricular symmetry.
The size of the ventricular system varies throughout pregnancy,
and the portion with the least variation in size is the atrium,
which measures normally between 6-9mm from week 15 to the end of pregnancy,
and for this reason biometrics of the ventricular system should include the atria.
Degrees:
- Mild ventriculomegaly: 10-12mm.
- Moderate ventriculomegaly: 13-15mm.
- Severe ventriculomegaly: More than 15mm.
It should be noted that hydrocephalus and ventriculomegaly are not synonymous: There is talk of hydrocephalus when the dilation is secondary to an obstruction (and with an increase in ventricular pressure); if not,
you should talk about ventriculomegaly.
However,
given the impossibility of measuring prenatal ventricular pressure,
there are authors who use both terms interchangeably when there are dilatations> 15mm and there are cortical thinnings,
macrocrania and other anomalies.
In short,
the diagnosis of hydrocephalus should be (if there is no clear prenatal obstructive cause) postnatal.
Neuronal migration pattern: Starts between weeks 12 and 16,
and ends after 24 weeks.
It is important mainly in MRI performed in early stages of pregnancy.It consists of 6 layers,
and begins in the periventricular germinal region and is directed towards the pial surface.According to the gestational age,
we will find a trilaminar (immature) or bilaminar (mature) pattern: At 16-19 weeks the trilaminar pattern translates the internal germinal matrix that surrounds the lateral ventricles (hypointense on T2-weighted sequences),
the neuronal zone intermediate (isointense) and the immature outer cortical layer (hypointense).
At 32-33 weeks the pattern is clearly bilaminar,
with white (internal) and cortical (external) substance in normal fetuses.
Sulcation/rotation: The rotation precedes the sulcation,
and the superior temporal gyrus is considered a marker of giral development,
so we must pay attention to its presence or absence.
At 20 weeks: The lateral sulcus and the interhemispheric fissure should be visualized.
At 25 weeks: Parieto-occipital,
hippocampal,
calcarine and cingular sulcus.
At 29 weeks: fissure of Rolando and precentral and postcentral sulcus,
lower frontal sulcus and inferior temporal sulcus.
At 35 weeks: Superior frontal and superior temporal sulcus.
At 35 weeks,
the definitive pattern will be present,
and all temporary sulcus must be present.
Myelination:
- From dorsal to ventral.
- From central to periphery.
- From caudal to cranial.
Around the 20th week myelination begins in the dorsal region of the brainstem.
In week 27 we will see myelination of the upper vermis,
the middle cerebellar peduncles,
as well as the basal ganglia.
In week 33-34 we will see with signs of myelination the posterior arm of the internal capsule and the globus pallidus; in week 36 we will see myelinated the anterior pontine region,
and finally by week 38-39 we will have the corona radiata in the process of myelination.
It must be remembered that supratentorial myelination does not usually begin until week 34-35.
Due to the deposits of phospholipids and other substances during myelination,
the zones that show maturation with myelin formation appear with a hyperintense signal in the sequences with T2 potentiation.
Posterior fossa: The area of normal vermis depends on gestational age:
- 28-29 weeks: 2.1 cm2.
- 30-31 weeks: 2.4 cm2.
- 32-33 weeks: 3.4 cm2.
Other findings:
-Evaluate the umbilical cord (sometimes presents multiple loops in the fetal neck).
-In very advanced gestation,
it is also convenient to assess the placenta.
-In addition to focusing on the fetal brain,
we must study the rest of the fetal body visible in the MRI study.
-Evaluate maternal findings (the presence of hydronephrosis is common.