Chronic calcifying pancreatitis is the most common cause of pancreatic calcifications.
Alcohol consumption is the most common cause of chronic calcifying pancreatitis,
accounting for as many as 50–70% of cases.
The formation of pancreatic calcifications is theorized to be due to ductal obstruction by proteinaceous plugs and accumulation of calcium carbonate. This obstruction results in ductal ectasia and periductal fibrosis.
Ductal calcifications can present in the main pancreatic duct or in side-branch ducts and can vary morphologically and in size, from microscopic to greater than 1 cm in diameter.
Focal or diffuse intraparenchymal calcification could be also found.
The degree of calcifications appears to parallel the course of the disease.
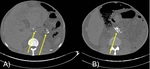
Chronic pancreatitis caused by hyperparathyroidism,
tropical pancreatitis,
and idiopathic pancreatitis can also result in intraductal calculi ( Fig. 1).
Cistic lesions
Pancreatic cystic lesions include inflammatory (pseudocysts),
benign (serous cystadenomas),
precancerous (intraductal papillary mucinous neoplasms [IPMNs] and mucinous cystic neoplasms [MCNs]),
and malignant (cystadenocarcinomas).
Since management varies,
due to the nature of the cystic lesions,
an accurate characterization is essential.
The presence of mural nodules,
septa-like structures,
or calcification on imaging examination contributes to the differential diagnosis.
Pseudocyst is among the most common cistic lesions; it is usually seen as unilocular round or oval shaped with a wall.
Occasionally,
pseuodocyst can have curvilinear or rim (egg-shell like) calcification and should be differentiated from the nodular and granular calcification of chronic pancreatitis,
which is usually within the pancreatic duct.
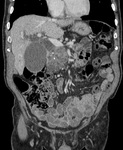
Serous cystic neoplasm commonly calcify ( Fig. 2 ).
Calcification pattern is characterized by a central calcified scar with calcified septations radiating outward,
resulting in a sunburst pattern.
The calcified central scar is highly specific for the diagnosis,
although not often present.
Curvilinear or peripheral egg shell-like calcifications are present in the cyst wall or septa in 15% of mucinous cystic neoplasms.
Multilocular macrocystic lesions with thick and calcific walls have a higher risk of malignancy than do unilocular lesions with thin walls without calcification.
Echinococcal cyst,
such as Mucinous cystic neoplasm,
may have curvilinear calcification and need to be further differentiated from calcified pseuodocyst.
Imaging features that favor a pancreatic pseudocyst include inflammatory changes within the peripancreatic fat,
pancreatic calcifications associated with chronic pancreatitis,
and the temporal evolution of the lesion at serial examinations.
The calcification pattern in IPMN is indistinguishable from that in chronic pancreatitis; calcifications can be found in the pancreaticduct,
parenchyma,
or diffusely throughout the gland.
Punctate calcification is the most common pattern (87%),
followed by coarse calcification (33%).
Cystic fibrosis,
tuberculosis,
cavernous Lymphangioma of the pancreas can also present as cystic lesions with calcification.
The calcification of cystic fibrosis and tuberculosis is typically granular in appearance,
while a collection of phleboliths in and adjacent to the pancreas is the characteristic feature of cavernous lymphangioma.
Solid lesions
Among solid pancreatic masses,
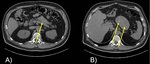
calcifications are more common in nonhyperfunctioning neuroendocrine tumors,
and tend to be focal,
coarse and located relatively centrally in a large pancreatic mass ( Fig. 3 ).
Functioning NETs,
such as insulinomas,
have been associated with calcifications in approximately 20% of cases.
Calcifications are not usually present in adenocarcinomas of the pancreas.
However,
pancreatic carcinoma may develop in a pancreas with underlying chronic calcific pancreatitis.
The presence of calcifications can also be caused by pancreatic ductal obstruction by adenocarcinoma.
Calcifications have also been reported in 6–50% of cases of Acinar Cell Carcinomas and are common (30%) in case of Solid Pseudopapillary Tumors,
in which they are characteristically peripheral and punctuate.
Mimics
There are several mimics of pancreatic calcifications.
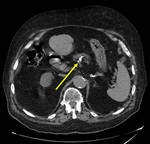
Vascular calcifications typically involve the splenic,
gastroduodenal,
and pancreaticoduodenal arteries and are generally identifiable by their characteristic linear,
tram-track appearance ( Fig. 4 ).
Calcified gallstones in the distal common bile duct are a potential mimic.
Oral contrast medium or hyperdense ingested material retained in duodenal or gastric diverticula can also be mistaken for calcification in the pancreas.