Ultrasonography (US) is the modality of choice for the initial evaluation of these patients,
because it provides excellent anatomic detail without subjecting the gametes to ionising radiation; by using color Doppler and power Doppler imaging,
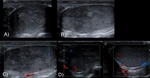
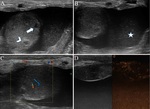
testicular perfusion can be assessed. The most important aim of imaging in these patients is to rule in or out testicular torsion,
which requires immediate intervention ( Fig. 1 ).
Scanning is performed with a high-frequency (8–15 MHz) transducer in sequential sagittal and transverse planes.
Testicular torsion
Testicular torsion,
or twisting of the spermatic cord,
implies primarily venous flow obstruction and subsequentely arterial obstruction.
The extent of testicular ischemia will depend on the degree of twisting (which ranges from 180° to 720° or greater) and the time after torsion.
In the early phases of torsion (1–3 hours),
testicular echogenicity appears normal.
After 4-6 hours,
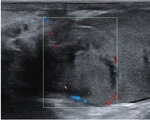
testicular swelling and decreased echogenicity are the most commonly encountered findings ( Fig. 2 ).
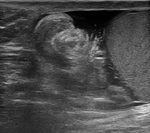
With progression,
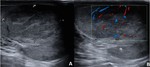
heterogeneous echogenicity and reactive hydrocele are common findings ( Fig. 3 ).
Color Doppler imaging demonstrates a complete absence of blood flow within the testis.
It is important to perform a comparative evaluation with the contralateral testis ( Fig. 3 ).
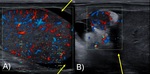
The “whirlpool sign”,
defined as an abrupt change in the course of the spermatic cord with a spiral twist at the external inguinal ring or in the scrotal sac,
is the most specific and sensitive sign of torsion,
both complete and incomplete ( Fig. 4 ).
Epididymitis
Epididymitis and epididymo-orchitis are common causes of acute scrotal pain in adolescent boys and adults.
In adolescents,
many instances are secondary to sexually transmitted organisms such as Chlamydia trachomatis and Neisseria gonorrhoeae.
In prepubertal boys and in men over 35 years of age,
the disease is most frequently caused by E coli and Proteus mirabilis.
Gray-scale US findings of acute epididymitis include an enlarged hypoechoic or hyperechoic (presumably secondary to hemorrhage) epididymis.
Indirect signs of inflammation,
such as reactive hydrocele or pyocele with scrotal wall thickening,
are present in most cases.
Orchitis develops in 20%–40% of cases due to direct spread of infection.
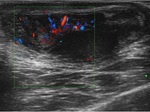
Diffuse testicular involvement is confirmed by the presence of testicular enlargement and an inhomogeneous testicular echotexture ( Fig. 5 ).
Color Doppler-US shows increased number and concentration of identifiable vessels with hyperemia,
resulting in a high-flow,
low-resistance pattern (Fig. 5,
Fig. 6 ).
Trauma
US is the first-line imaging test for scrotal trauma.
US findings are crucial in clinical decision making.
US imaging findings include fluid collections,
testicular disruption,
and vascular injury.
If the testis is ruptured,
emergent surgery can salvage the testis in 80%–90% of cases.
Hematomas may occur in intratesticular locations or extratesticular soft tissues (scrotal wall or epididymis).
The lesions are usually focal, hyperechoic (in acute bleeding) or hypoechoic (as the hemorrhage ages),
and a lack of vascularity may be found ( Fig. 7 ).
Hydrocele is a predominantly anechoic fluid collection that occurs in the virtual space between the two layers of the tunica vaginalis.
Similar to hydroceles,
hematocele is a complex collection that separates the visceral and parietal layers of the tunica vaginalis.
Subacute and chronic hematocele may contain fluid-fluid levels or low-level internal echoes ( Fig. 7 ).
A testicular fracture appears as a linear hypoechoic band that extends across the testicular parenchyma and represents a break in the normal testicular architecture ( Fig. 8 ).
An associated hematocele or testicular hematoma may be seen.
Heterogenous echotexture within testis,
testicular contour abnormality and disruption of tunica albuginea are very sensitive and specific signs for the diagnosis of testicular rupture.
Testicular tumors
Testicular cancer is the most common tumor in young adult men.
In the majority of cases,
it occurs in young men aged 15–35 year.
In young men,
approximately 95% of testicular cancers are germ cell tumors,
and 5% are sex cord–stromal tumors.
Approximately 50% of germ cell tumors are seminomas,
while approximately 50% are nonseminomatous germ cell tumors (NSGCTs).
US is used to distinguish between intratesticular masses,
which are more commonly malignant,
and extratesticular masses,
which are more commonly benign.
At imaging,
a solid intratesticular mass with internal vascularity is suggestive of a testicular tumor ( Fig. 9 ).
Seminomas are often hypoechoic and homogeneous with infrequent calcifications.
With contrast-enhanced Ultrasound (CEUS),
there is a rapid enhancement in the tumour (higher than the surrounding normal testicular parenchyma) and loss of the normal linear vascular pattern.
Washout of the contrast within the lesion may be rapid.
NSGCTs are more commonly heterogeneous in echotexture,
mostly demonstrating cystic spaces.