Patients with abdominal pain from a private hospital in São Paulo-Brazil were evaluated by MRI.
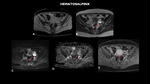
HEPATITIS
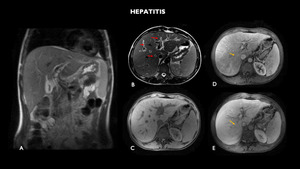
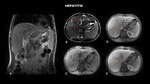
Fig. 1: MRI (A – coronal T2, B – axial T2, C – axial before, D- axial arteriosus phase, E- axial portal phase,) shows liver of slightly enlarged dimensions, associated with diffuse periportal edema (red arrow) and associated perfusion disorder (yellow arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
ACUTE CALCULOUS CHOLECYSTITIS AND CHOLEDOCHOLITHIASIS
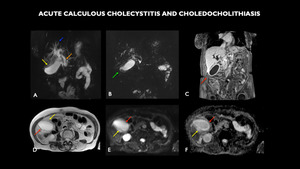
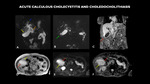
Fig. 2: MRI (A – coronal 3D, B – Magnetic Resonance Cholangiopancreatography - MRCP coronal, C – coronal post contrast, D – axial T2, E- axial diffusion-weighted imaging - DWI, F – axial apparent diffusion coefficient-ADC) shows distended gallbladder with diffuse parietal thickening (red arrows) and with small calculi / deposited biliary mud (green arrow). Diffuse perivesicular edema (yellow arrows) is associated. Moderate diffuse dilation of the bile ducts to the plane of the papilla (blue arrow). An elongated calculus measuring 4.0 x 1.5 mm is observed in the middle third of the common bile duct, 3.2 cm apart from the papilla (orange arrow). Diffuse parietal enhancement of the bile ducts is associated with enhancement heterogeneity in the periphery of the right hepatic lobe, inferring inflammatory component associated.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
CHOLELITHIASIS AND CHOLEDOCHOLITHIASIS
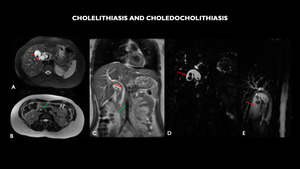
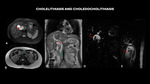
Fig. 3: MRI (A – axial T2 with fat-sat, B – axial T2, C – coronal T2), shows multiple calculi in the gallbladder (red arrow) and filling failure in the plane of the duodenal papilla, corresponding to micro calculi (green arrow). Choledochal dilated with calculus in its interior. Cholangioresonance (D and E). Multiple calculi in the gallbladder.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
ACUTE OEDEMATOUS PANCREATITIS
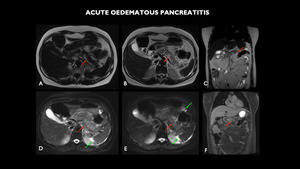
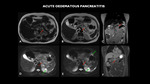
Fig. 4: MRI (A – axial T1 dixon F, B – axial T2, C – coronal T2, D – axial T2 with fat-sat, E – axial DWI, F –coronal T2 post contrast) shows the enlarged pancreas, with loss of usual acinar lobulated contours, with marked parenchymal edema (red arrows). It is associated with a change in the sign of the peripancreatic adipose plane, with a moderate amount of fluid that extends to the gastroesplenic space and to the flanks through the anterior pararenal and lateral canals (green arrows). Post-contrast enhancement areas are not characterized.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
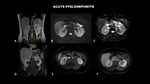
ACUTE PYELONEPHRITIS
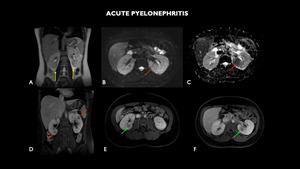
Fig. 5: MRI (A – coronal T2, B – axial diffusion-weighted imaging - DWI, C – axial apparent diffusion coefficient-ADC, D – coronal T1 post contrast, E and F- axial T1 post contrast) shows undefined areas of signal change sparse in the bilateral renal parenchyma, more numerous and larger on the left (red arrows). They are characterized by tenuous hypersignal foci in T2 interspersed with low-signal focus, showing heterogeneous contrast enhancement, with predominance of hypo-contrast, configuring the appearance of striated nephrogram (green arrows). Signal alteration of the perinephric fatplane is associated with a small amount of fluid, larger on the left, and thickening of the pararenal fascia (yellow arrows).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
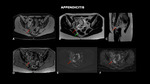
APPENDICITIS
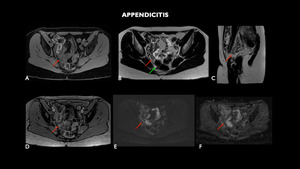
Fig. 6: MRI (A – axial T1 with fat-sat, B – axial T2, C – sagittal T2, D – axial T1 post contrast, E – axial DWI, F – axial ADC) shows cecal appendix of posterior and medial tract, located in the pelvic excavation, with a slightly enlarged diameter (0.9 cm) and parietal post-contrast enhancement and certain blurring of adjacent adipose planes, findings compatible with acute appendicitis (red arrows). There are no organized collections, evidencing only small amount of free fluid in the pelvis.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
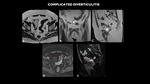
COMPLICATED DIVERTICULITIS
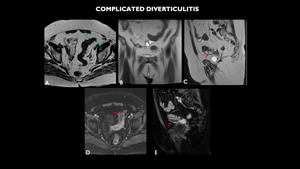
Fig. 7: MRI (A – axial T2, B – coronal T2, C – sagittal T2, D – axial post contrast, E - sagital post contrast) shows diverticulum sparse in sigmoid (green arrow), associated with mild regular parietal thickening of this intestinal segment, with small collection adjacent to the lower contour of this, with gaseous foci of permeation (red arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
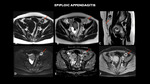
EPIPLOIC APPENDAGITIS
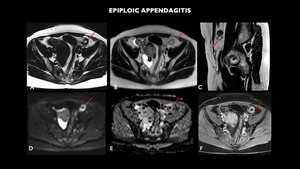
Fig. 8: MRI (A – axial T1, B – axial T2, C- sagittal T2, D- axial diffusion-weighted imaging - DWI, E – axial apparent diffusion coefficient-ADC, F- axial T1 post contrast) shows nodule with fat attenuation measuring 1.7 cm on the antimesenteric border of the sigmoid / descending colon transition with peripheral enhancement, associated with the densification of local adipose planes, compatible with epiploic appendagitis.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
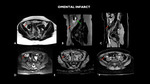
OMENTAL INFARCT
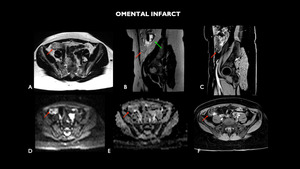
Fig. 9: MRI (A – axial T1, B – sagittal T2, C- sagittal T1 post contrast, D- axial diffusion-weighted imaging - DWI, E – axial apparent diffusion coefficient-ADC, F- axial T1 post contrast) shows densification of the fat with diffusion restriction on the antimesenteric face in the right iliac fossa, inferring omental infarction (red arrows). Adnexial formation left, suggestive of chronic hematosalpinx (green arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
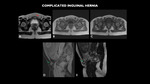
COMPLICATED INGUINAL HERNIA
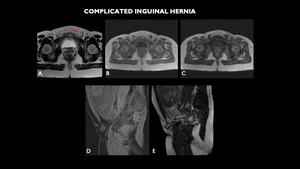
Fig. 10: MRI (A – axial T2, (A – axial T2, B – axial in phase, C – axial out of phase, D- sagittal without effort- DWI, E – sagittal with Valsalva maneuver) shows enlargement of the left inguinal canal (red arrow), with dislocation of intestinal portion and mesentery, which does not suffer significant alterations to the Valsalva maneuver (green arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
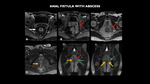
ANAL FISTULA WITH ABSCESS
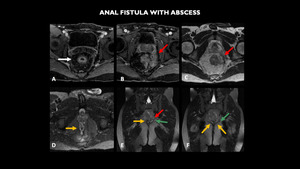
Fig. 11: MRI (A - axial T1 post contrast, B - coronal T1 post contrast, C - axial T2, D - axial T2 with fat-sat, E and F - coronal T2) shows left pararetal abscess (red arrow), just above the anus levator muscle (green arrow) and in close contact with it, associated with surrounding soft tissue edema and diffuse fistulae (yellow arrow), sometimes communicating, that are externalized in the gluteal fold (images not included). Note the parietal thickening of the rectum with engorgement of the straight vessels (white arrow), suggesting inflammatory disease in activity.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
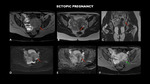
ECTOPIC PREGNANCY
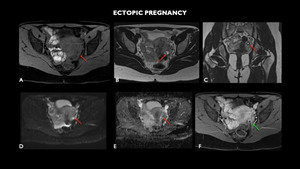
Fig. 12: MRI (A – axial T1, B – axial T2, C- coronal T2, D- axial diffusion-weighted imaging - DWI, E – axial apparent diffusion coefficient-ADC, F- axial T1 post contrast) shows small cystic formation with thick walls in the left adnexal region (red arrows), located between the medial ovarian surface and the uterine wall, measuring about 0.9 cm, showing parietal enhancement to the intravenous contrast (green arrow). This formation, although nonspecific, confirmed that it was ectopic gestation on ultrasonography.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
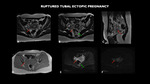
RUPTURED TUBAL ECTOPIC PREGNANCY
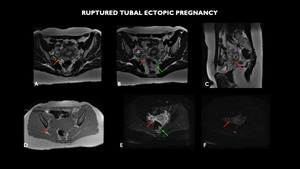
Fig. 13: MRI (A and B– axial T2, C- sagittal T2, D – axial T1 in phase, E- axial diffusion-weighted imaging - DWI, F – axial apparent diffusion coefficient-ADC) shows in the right adnexal region, between the ovary and the uterine body, the presence of elongated nodular formation and cystic appearance, with thick and amphoraous walls, measuring 3.7 x 1.7 cm (red arrows). Fluid with a higher protein / hemorrhagic level and with hydro-air level occupying much of the pelvic excavation, compatible with hematopneumoperitoneum (green arrows).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
HEMATOSALPINX
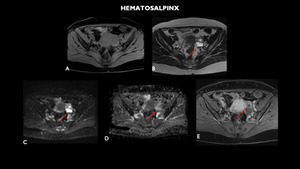
Fig. 14: MRI (A- axial T1, B- axial T2, C- axial diffusion-weighted imaging - DWI, D – axial apparent diffusion coefficient-ADC, E- axial T1 post contrast) shows tubular and sinuous formation in the left adnexal, just-ovarian region, measuring 4.4 x 2.5 cm, with a liquid content and sometimes thick, leveled formation suggestive of hematosalpinx (red arrows).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
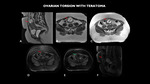
OVARIAN TORSION WITH TERATOMA
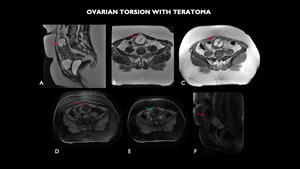
Fig. 15: MRI (A - sagittal T2, B - axial T2, C - axial T1, D - axial T1 with fat-sat, E - axial post contrast, F - sagittal post contrast) shows expansive lesion with hypersignal T2 (red arrow). Note also the absence of post-contrast enhancement of the entire ovary, with adjacent vascular pedicle (green arrow), suggesting ovarian torsion.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
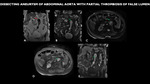
DISSECTING ANEURYSM OF ABDOMINAL AORTA WITH PARTIAL THROMBOSIS OF FALSE LUMEN
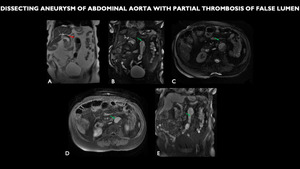
Fig. 16: MRI (A - coronal T2, B - coronal FIESTA, C - axial FIESTA, D - axial post contrast, E - coronal post contrast) shows diffuse abdominal ectasia, tortuous and atheromatous (red arrow) aortic aneurysm of the infrarenal aorta, with partial thrombosis of its lumen (green arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
INFERIOR VENA CAVA THROMBOSIS
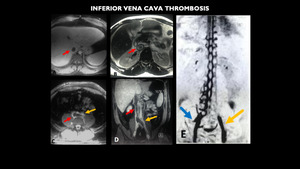
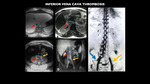
Fig. 17: MRI (A e C – axial T1 venous, B – axial T2, D – coronal T1 venous, E – 3D MIP reconstruction) shows inferior vena cava (red arrow) and left common iliac vein thrombosis (yellow arrow), also hepatic veins and left renal vein thrombosis (images not included). Note the extensive collateral circulation established through the vertebral plexus from the right common iliac vein (blue arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
SUPERIOR MESENTERIC VENA THROMBOSIS
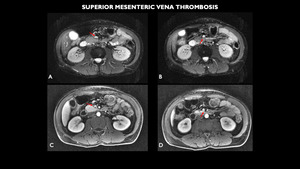
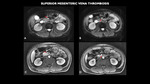
Fig. 18: MRI (A and B- axial diffusion-weighted imaging - DWI, C and D- axial T1 post contrast) shows small partial filling failure in the upper segment of the superior mesenteric vein (red arrows).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil