We conducted a review of the literature and retrospective analysis of around thirty cases of patients with vascular thoracoabdominal emergencies,
who were admitted to the emergency room and evaluated by MRI.
Imaging characteristics will be demonstrated by anatomical sections,
multiplanar reconstructions,
volumetric acquisition,
and simplified pictorial schemes.
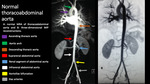
NORMAL THORACOABDOMINAL AORTA
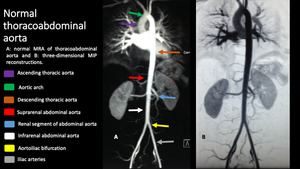
Fig. 1: Images from a normal Resonance Magnetic Angiography (MRA) shows the segments of aorta: ascending (purple arrow), aortic arch (green arrow), descending thoracic (orange arrow), suprarenal (red arrow), renal (blue arrow), infrarenal (white arrow), and aortoiliac bifurcation (yellow arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
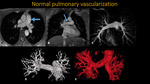
NORMAL PULMONARY VASCULARIZATION
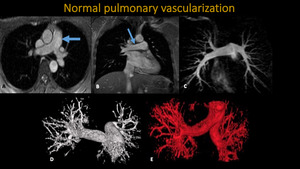
Fig. 2: MRI and MRA of thorax . A: Axial Trufisp. B: Coronal Trufisp. C: three-dimensional MIP reconstruction. D and E: three-dimensional surface reconstructions. Blue arrows demonstrating usual aspect of pulmonar trunk.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
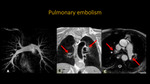
PULMONARY EMBOLISM
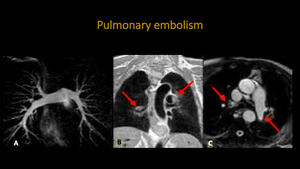
Fig. 3: MRI and MRA of thorax. A: MIP 3D demonstrating usual aspect of pulmonary vascularization. B: Coronal T1 "black blood". C: Axial Trufisp. Red arrows showing signals of pulmonary embolism.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
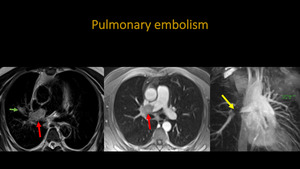
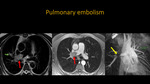
Fig. 4: Thoracic MRA. A: Axial T2 BLADE. B: Axial T1 post contrast. C: 3D MIP reconstruction. Images demonstrate thrombus occluding the right pulmonary artery (red arrow), extending to segmental branches (green arrow). Three-dimensional MIP reconstruction points non-opacificated segment of the occluded pulmonary artery (yellow arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
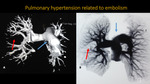
PULMONARY HYPERTENSION RELATED TO EMBOLISM
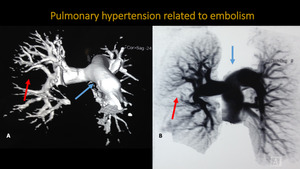
Fig. 5: Thoracic MRA. A: Three-dimensiona VR reconstruction. B: inverted three-dimensional MIP reconstruction. Images demonstrate signals of pulmonary embolism on right segmental branch associated with area of pulmonary oligaemia (red arrow). There is also pulmonary trunk ectasia indicating pulmonary hypertension (blue arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
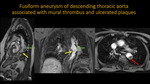
FUSIFORM ANEURYSM OF DESCENDING THORACIC AORTA ASSOCIATED WITH MURAL THROMBUS AND ULCERATE PLAQUES
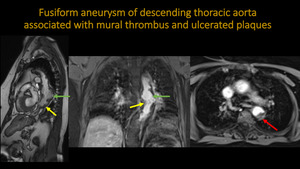
Fig. 6: MRA of thoracic aorta. A: Sagital TRUFISP. B: Coronal and Axial T1 three-dimensional post contrast. Images show fusiform aneurym of descending aorta (green arrow), presenting circular eccentric thrombus (red arrow), and multiple sparse ulcerated plaques (yellow arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
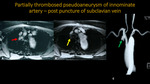
PARTIALLY THROMBOSED PSEUDOANEURYSM OF INNOMINATE ARTERY - POST PUNCTURE OF SUBCLAVIAN VEIN
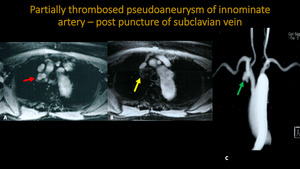
Fig. 7: MR and MRA of thorax . A and B: Axial T1 post contrast. C: 3D MIP reconstruction. There is a pseudoaneurysm of the innominate artery (red arrow), seen partially thrombosed on the yellow arrow. Three-dimensional MIP reconstruction also points the area of pseudoaneurysm (green arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
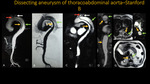
DISSECTING ANEURYSM OF THORACOABDOMINAL AORTA - STANFORD B
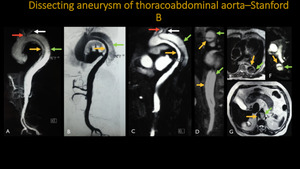
Fig. 8: A-D: Three-dimensional MIP reconstructions. E-G: Axial T2. Dissection of the thoracoabdominal aorta: angioresonance images show intimal flap dissection with origin in the aortic arch, right after the origin of the left common carotid artery (red arrow), extending to the adrenal segment of the abdominal aorta, dividing the aortic lumens into true (yellow arrow) and false (green arrow). The left subclavian artery (white arrow) originates from the false lumen in the aortic arch.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
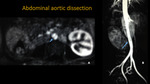
ABDOMINAL AORTIC DISSECTION
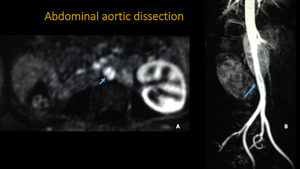
Fig. 9: Thoracic aorta MRA. A: 3D FAT-SAT post contrast reconstruction. B: 3D MIP reconstruction. Images demonstrate the área of dissection-intimal flap (blue arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
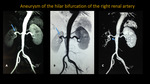
ANEURYSM OF THE HILAR BIFURCATION OF THE RIGHT RENAL ARTERY
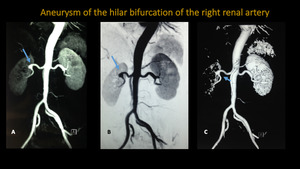
Fig. 10: MRA of aorta and renal arteries. A and B: 3D MIP reconstructions. C: 3D VR reconstruction.
Blue arrows pointing the aneurysm of the hilar bifurcation of the right renal artery in a 59 years old female patient.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
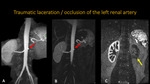
TRAUMATIC LACERATION / OCCLUSION OF THE LEFT RENAL ARTERY
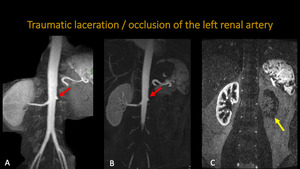
Fig. 11: Abdominal MRA. A and B: 3D MIP reconstructions. C: Coronal MRA. Patient suffered automotive trauma and evolved with occlusion/laceration of the left renal artery, just after its origin (red arrow). We see also absence of vascularization of the left kidney (yellow arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
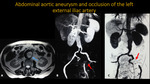
ABDOMINAL AORTIC ANEURYSM AND OCCLUSION OF THE LEFT EXTERNAL ILIAC ARTERY
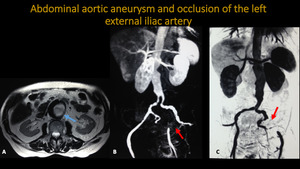
Fig. 12: Abdominal aortic MRA. A: Axial T2. B and C: 3D MIP reconstructions. Blue arrow: abdominal aortic aneurysm with slow flow demonstrated by loss of flow-void. Red arrows pointing occlusion of left distal common and external iliac arteries.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
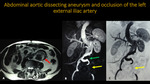
ABDOMINAL AORTIC DISSECTING ANEURYSM AND OCCLUSION OF THE LEFT EXTERNAL ILIAC ARTERY
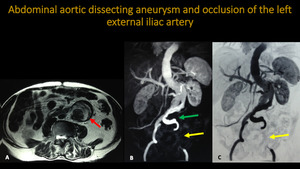
Fig. 13: Abdominal aortic MRA. A: Axial T2. B and C: 3D MIP reconstructions. Pictures show infrarenal abdominal aortic dissecting aneurysm (red arrow). We can see the left common iiac artery being filled by false lumen (green arrow). There is also occlusion of the left external iliac artery (yellow arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
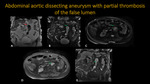
ABDOMINAL AORTIC DISSECTING ANEURYSM WITH PARTIAL THROMBOSIS OF THE FALSE LUMEN
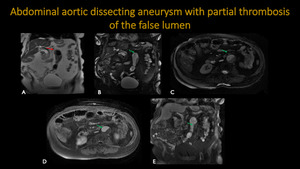
Fig. 14: MR Images (A – coronal T2, B – coronal FIESTA, C – sagital FIESTA, D – axial post-contrast, E – sagital post-contrast) show diffusely ectasiated, tortuous e atheromatous abdominal aorta (red arrow) with infrarrenal aortic aneurysm and partial thrombosis of its lumen (green arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
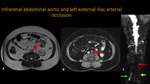
INFRARENAL ABDOMINAL AORTIC AND LEFT EXTERNAL ILIAC ARTERIAL OCCLUSION
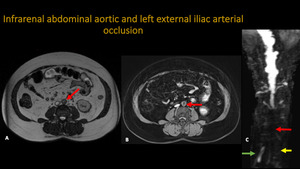
Fig. 15: MRA. A: Axial T2. B: Axial T1 post-contrast. C: 3D MIP reconstruction. Pictures demonstrate abdominal aortic occlusion, that extends from the infrarenal segment to the aortoiliac one, with occlusion of both internal and the left external iliac arteries (yellow arrow). We can see also refilling of the distal segment of right external iliac artery (green arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
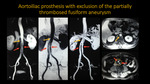
AORTOILIAC PROTHESIS WITH EXCLUSION OF THE PARTIALLY THROMBOSED FUSIFORM ANEURYSM
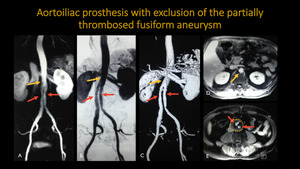
Fig. 16: Abdominal aortic prosthesis with exclusion of the aneurysm: angioresonance images show a prosthesis (red arrow) in the infrarenal segment of the abdominal aorta with bilateral extension to the respective common iliac arteries and exclusion of the partially thrombosed fusiform aneurysm (yellow dotted line), not identified in the angiographic reconstructions post-contrast. Note the usual characterization of the adrenal aortic segment (yellow arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
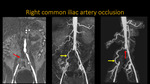
RIGHT COMMON ILIAC ARTERY OCCLUSION
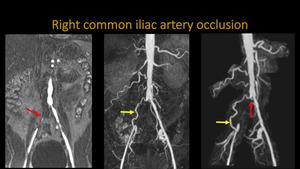
Fig. 17: Abdominal and thoracic aortic MR angiography. A: Coronal T1 post contrast. B and C: 3D MIP reconstructions. Notice the right common iliac artery occlusion (red arrow), with filling of ipsilateral external and internal iliac arteries by colateral branches (yellow arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
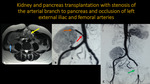
KIDNEY AND PANCREAS TRANSPLANTATION WITH STENOSIS OF THE ARTERIAL BRANCH TO PANCREAS AND OCCLUSION OF THE LEFT EXTERNAL ILIAC AND FEMORAL ARTERIES
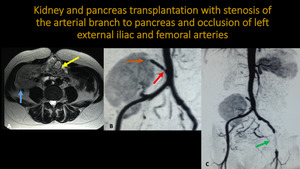
Fig. 18: Abdominal MR and abdominal aortic MRA. A: Axial T2. B and C: 3D MIP reconstructions. Images show kidney (blue arrow) and pancreas (yellow arrow) transplanted in right iliac fossa. There is stenosis of the proximal segment of the arterial branch to pancreas (red arrow) and occlusion of the distal branch (orange arrow). It is still observed occlusion of left external iliac and femoral arteries (green arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
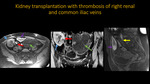
KIDNEY TRANSPLANTATION WITH THROMBOSIS OF RIGHT RENAL AND COMMON ILIAC VEINS
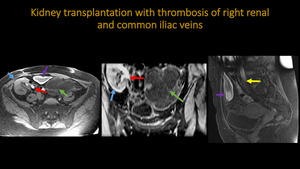
Fig. 19: Abdominal MR. A: Axial T1 FS. B: Coronal T1 FS. C: Sagital T1 FS. Pictures point transplanted kidney in right iliac fossa (blue arrow), abrupt tapering with occlusion of the right renal and common iliac veins (red and yellow arrows respectively). Additional findings include hemorrhage ovarian cyst (green arrow)) and an adjacent small hemorrhage collection (purple arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
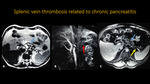
SPLENIC VEIN THROMBOSIS RELATED TO CHRONIC PANCREATITIS
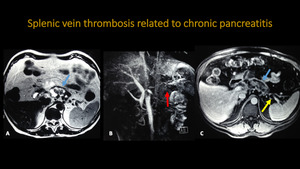
Fig. 20: Abdominal MR and MRA. A: Axial T2. B: 3D MIP reconstruction. C:. Axial T1 post contrast.
There are signals of chronic pancreatitis (blue arrow), associated with splenic vein thrombosis (yellow arrow), and no opacification of the vessel on 3D reconstruction (red arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
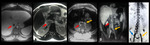
INFERIOR VENA CAVA THROMBOSIS
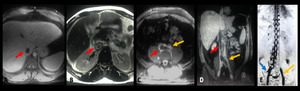
Fig. 21: Thrombosis of the left common iliac vein and inferior vena cava: angioresonance images show inferior vena cava (red arrow) and left common iliac vein thrombosis (yellow arrow), also hepatic veins and left renal vein thrombosis (images not included). Note the extensive collateral circulation established through the vertebral plexus from the right common iliac vein (blue arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
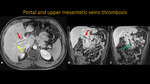
PORTAL AND UPPER MESENTERIC VEINS THROMBOSIS
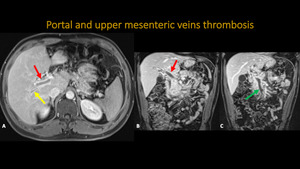
Fig. 22: Abdominal MR and MRA. A: Axial T1 post contrast. B and C: Coronal T1 post contrast. Notice the signals of portal vein and its right branch occlusion (red and yellow arrows respectively), extending to upper mesenteric vein (green arrow). There is portal parietal thickening with hyperenhancement, inferring inflamatory process/vasculitis.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
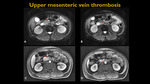
UPPER MESENTERIC VEIN THROMBOSIS
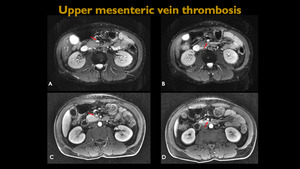
Fig. 23: Abdominal MR – A and B Axial diffusion. C and D: Axial T1 post-contrast. Images evidence partial filling failure on the upper segment of upper mesenteric vein.
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil
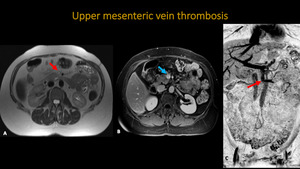
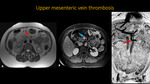
Fig. 24: Abdominal MR and MRA. A: Axial T2. B: Axial T1 post-contrast. C: 3D MIP reconstruction. Images show occlusion of the middle segment of the upper mesenteric vein (red arrow) and filling failure inside the vessel (blue arrow).
References: Hospital Alvorada/ Americas Serviços Médicos, São Paulo / Brazil