Shoulder pain is a very common complaint and can be a source of discomfort for patients of all ages.
Pain attributed to degenerative and inflammatory etiologies can be relieved by utilizing targeted US-guided steroid and anesthetic injections.
These procedures can be performed in the outpatient setting and result in rapid symptomatic relief.
Examples of such etiologies include subacromial-subdeltoid bursitis,
adhesive capsulitis,
osteoarthritis,
as well as tendinopathy.
Subacromial-subdeltoid Bursitis
The subacromial-subdeltoid bursa (SASD) is a large synovial-lined potential space between the rotator cuff tendons,
deltoid muscle,
undersurface of the acromioclavicular joint and overlies the bicipital groove.
Inflammation of this bursa is non-specific and can be due to a range of pathologies which include,
but are not limited to: chronic repetitive trauma,
acute shoulder trauma,
acromioclavicular joint disorders,
impingement disorders,
rheumatoid arthritis,
calcium deposition arthropathy and infection [1]. This entity generally results in a painful arc of motion,
generally during abduction and internal rotation as well as all resisted movements around the effected shoulder.
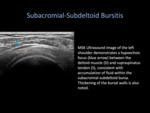
Generally appearing as a thin hypoechoic line of tissue on ultrasound,
inflammation of the bursa results in accumulation of fluid within this potential space.
Patients experiencing pain from subacromial-subdeltoid bursitis are able to find significant symptomatic relief from US-guided steroid and anesthetic injection into the SASD [2].
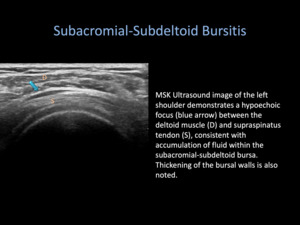
Fig. 1: Subacromial-Subdeltoid Bursitis
Adhesive capsulitis
Adhesive capsulitis (ADCAP) or frozen shoulder is a very common condition of the glenohumeral joint synovium and capsule.
This condition is usually seen between 40 and 60 years of age,
with a female predilection.
Although the pathogenesis of AC is poorly understood,
it is thought to be a combination of synovial inflammation and capsular fibrosis [3].
ADCAP is usually classified as primary or secondary.
Primary ADCAP can be idiopathic or may be related to immunologic,
biochemical,
or hormonal imbalances.
Secondary ADCAP can be due to known causes of stiffness and immobility such as recent trauma or surgery.
ADCAP results in pain,
stiffness and limited range of motion of the affected shoulder.
Although the diagnosis is usually clinical,
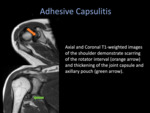
MRI of the affected shoulder can demonstrate thickening of the joint capsule,
rotator interval and thickening of the inferior glenohumeral ligament in the axillary pouch.
Patients suffering from ADCAP haven been shown to benefit from US-guided steroid and anesthetic injection into the glenohumeral joint [4].
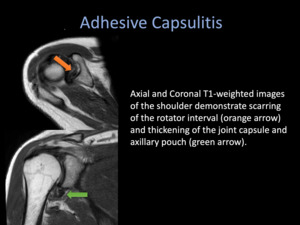
Fig. 2: Adhesive Capsulitis
Osteoarthritis
Osteoarthritis (OA) generally occurs in the older population,
following traumatic injury in younger patients,
or secondary to hydroxyapatite deposition or rheumatoid arthritis.
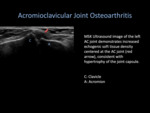
OA around the shoulder girdle generally affects the acromioclavicular (AC) and glenohumeral (GH) joints.
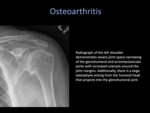
Radiological hallmarks of OA include joint space narrowing,
osteophytosis,
sclerosis at the joint margins and subchondral cyst formation.
Patients experiencing pain from OA are able to find significant symptomatic relief from US-guided steroid and anesthetic injection into the AC and GH joints [8].
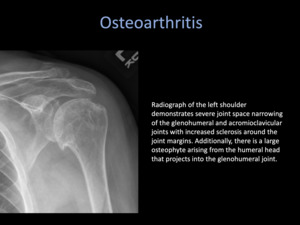
Fig. 3: Osteoarthritis
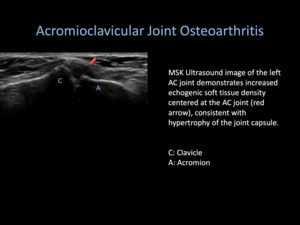
Fig. 4: Acromioclavicular Joint Osteoarthritis
Tendinopathy
Tendinopathy,
also known as tendinosis or tendonitis,
refers to nonspecific swelling of a tendon.
While most commonly seen in active patients and athletes,
tendinopathies can affect patients of all ages.
Most common causes include repetitive motion and microtrauma,
external impingement,
inflammatory conditions such as rheumatoid arthritis and gout,
hydroxyapatite deposition (calcific tendonitis),
as well as diabetes [5].
Around the shoulder,
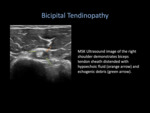
the most commonly affected tendons are the rotator cuff tendons and the long head of the biceps tendon (LHBT). Ultrasound demonstrates swelling of the tendon with loss of the normal fibrillar pattern,
which is replaced by a heterogeneous hypoechoic changes.
Doppler interrogation may demonstrate neovascularity around the tendon [6].
Patients suffering from calcific tendinits have been shown to benefit from US-guided lavage and those suffering from other tendinopathies have been shown to benefit from US-guided and steroid and anesthetic injections into the affected tendon sheath [7].
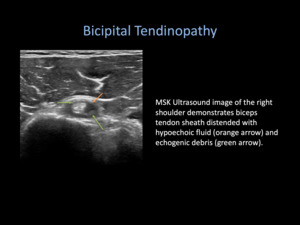
Fig. 5: Bicipital Tendinopathy